Types of Anesthesia in Labor

The arrival of the baby is a very mobilizing event for the whole family, even more so for the mother who’s about to give birth. The sensations and experiences are so unique that it’s not possible to generalize them, much less put them into words. But if there’s something that most women have in common when it comes to giving birth, it’s pain, and that’s why today we’re going to tell you about the types of anesthesia that exist to have a less uncomfortable experience during labor and delivery.
As we always say, anticipation and prophylaxis strategies before delivery are very important. Still, we can’t deny or ignore the benefits of these pharmacological measures. With good information, we’ll be able to make better decisions. Keep reading to learn more.
The pain of childbirth, a unique experience
Surely you’ve wondered why there are women who can give birth without external help, while others come to faint from the pains of contractions. The explanation for this is quite simple: Pain is a relative and subjective sensation.
Next, we’ll share the latest definition of this sensation prepared by the International Association for the Study of Pain in 2020:
“Pain is an unpleasant sensory and emotional experience, associated with or similar to that associated with an actual or potential tissue injury.”
Experts in the field agree that labor pain is an individual response to the different stimuli that the woman receives. It means that these signals are received and interpreted in a unique way, as the context of each delivery is different (Hawkins, 2010). In this sense, physical sensations, emotions, motivation, previous experiences, and social and cultural components play a key role in the painful experience.
So, as pain is such a complex entity, it’s not always possible to control it voluntarily. In fact, many times, physiological responses to painful stimuli can put the well-being of mother and baby at risk. They can even interfere with the normal progression of labor. And in this sense, adequate anesthesia and analgesia can favor the desired outcome.
Types of anesthesia for childbirth
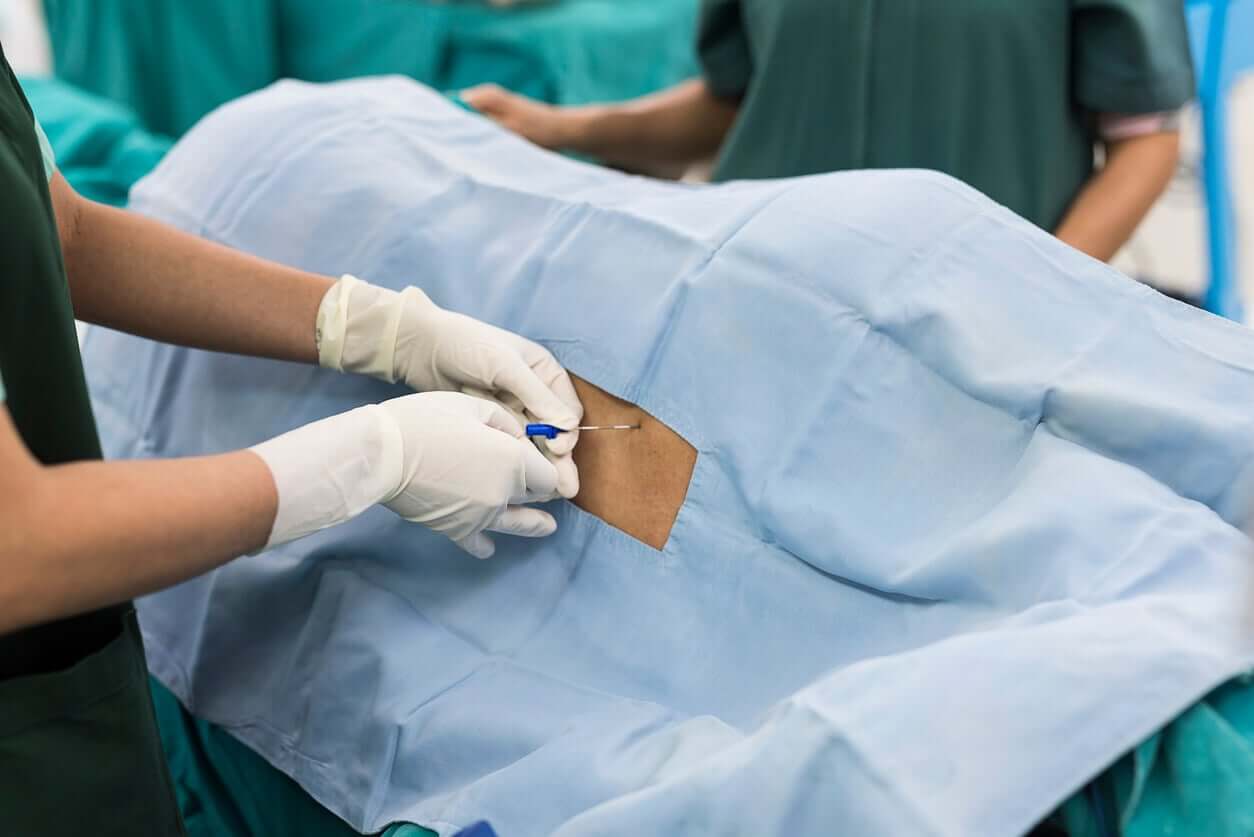
The main objective of anesthesia is to reduce the sensation of pain before an invasive or traumatic procedure, such as surgery or the delivery itself. For this, drugs are administered that cancel the sensitivity of a certain region of the body temporarily and reversibly. This is known as analgesia.
In some cases, it’s also necessary to relax the muscles or put a woman under in order to perform more complex procedures. These effects are myorelaxation and sedation, respectively.
In the case of delivery (either vaginal or by cesarean section), there are several types of anesthesia possible and the choice of one or the other is subject to individual circumstances. In this sense, not only are maternal preferences considered but medical staff also seek to provide the best care conditions for the pregnant woman and her baby.
As a practical matter, we’re going to classify the types of anesthesia for childbirth as follows:
- Local: This is the administration of the anesthetic in a specific area of the body, through an injection that’s placed in the subcutaneous cellular tissue (the one that’s below the dermal layer of the skin).
- Regional: In this case, the drug seeks to numb a certain region of the body. For example, the lower half of the body. In this case, the anesthetic is administered into the medullary canal.
- General: This type of anesthesia involves complete sedation of the patient (putting the woman into a stage of unconsciousness), muscle relaxation, and of course, analgesia. Medications are administered through the veins and require external ventilation and other advanced life support measures.
Some anatomical concepts
To understand each procedure, you need to know some basic notions regarding human anatomy. For example, it’s essential that you know where the painful stimulus circulates to understand why anesthetic drugs are administered in such a way.
Inside the skull is the brain, and this connects with the rest of the body’s organs through nerves. The latter are like wires that send sensitive information (such as pain or touch) from the viscera, muscles, or skin to the brain and in turn, return the “brain orders” to these tissues. The messages from the brain can be motor stimuli (such as removing your hand from a heat source) or behavioral (such as the urge to run away in fear), among others.
Nerves, in general, don’t leave directly from the brain, but from its attached structures: The brain stem and the spinal cord. The latter extends from the base of the head to almost the waist through a hole that remains within the vertebrae, called the canal or medullary canal.
Within the medullary canal, there are different cavities, as the medulla passes through it wrapped in membranes and liquid. One of the main medullary envelopes is called the dura mater, and according to this, the following spaces are defined:
- Epidural or epidural: This is the one that’s included between the bone of the vertebrae and the dura mater.
- Subdural or intradural: This is the space between the dura mater and the medulla, which is occupied by the cerebrospinal fluid.
Depending on the site where the drugs are administered and their characteristics, the different types of anesthesia may be carried out.
1. Local anesthesia
As we’ve mentioned, this type of anesthesia is used to block the sensitivity of a limited and determined area. For example, the perineal area where an episiotomy will be sutured in a mother who didn’t receive another type of anesthesia during childbirth.
This type of anesthesia is called infiltration and is done by injecting the drug through the skin of the vaginal frenulum. In this act, the thin fibers of the pudendal nerve are blocked and the woman loses sensitivity in this part of her vagina.
Due to the thinness of the tissue, it begins to act quickly and for a short period of time. Therefore, it’s ideal for performing the episiotomy and for its closure.
On the other hand, due to its short time of action and its localized effect, it’s not an adequate alternative to alleviate the pain of labor contractions.
2. Loco-regional anesthesia
This type of anesthesia is the most used for obstetric procedures, as it allows the blocking of intense pain in the lower half of the body. This way, the mother can go through the delivery in a more bearable way and avoid the adverse effects of the intolerable painful sensation.
Depending on the route of delivery (vaginal or cesarean section), one of the following techniques will be chosen:
- Epidural anesthesia: This is the most appropriate for vaginal delivery, as it allows the administration of medications in a sustained way over time. This is thanks to the placement of a thin catheter in the epidural space.
- Spinal anesthesia: This type of anesthesia favors the administration of higher doses of drugs, which allows a gradual numbing of the area for surgery. First, it blocks the pain, then the touch, and finally, the mobility of the muscles. In this case, the drug is injected into the subdural space only once before the surgical act.
To perform both procedures, a professional must perform a puncture on the mother’s back. But despite the fears, this’s done at a height where there’s no spinal cord, but rather thin filaments of it. Therefore, the risk of injuring it is quite low.
Like any invasive procedure, it has associated adverse effects, but in general, it’s a safe technique for both mother and baby.
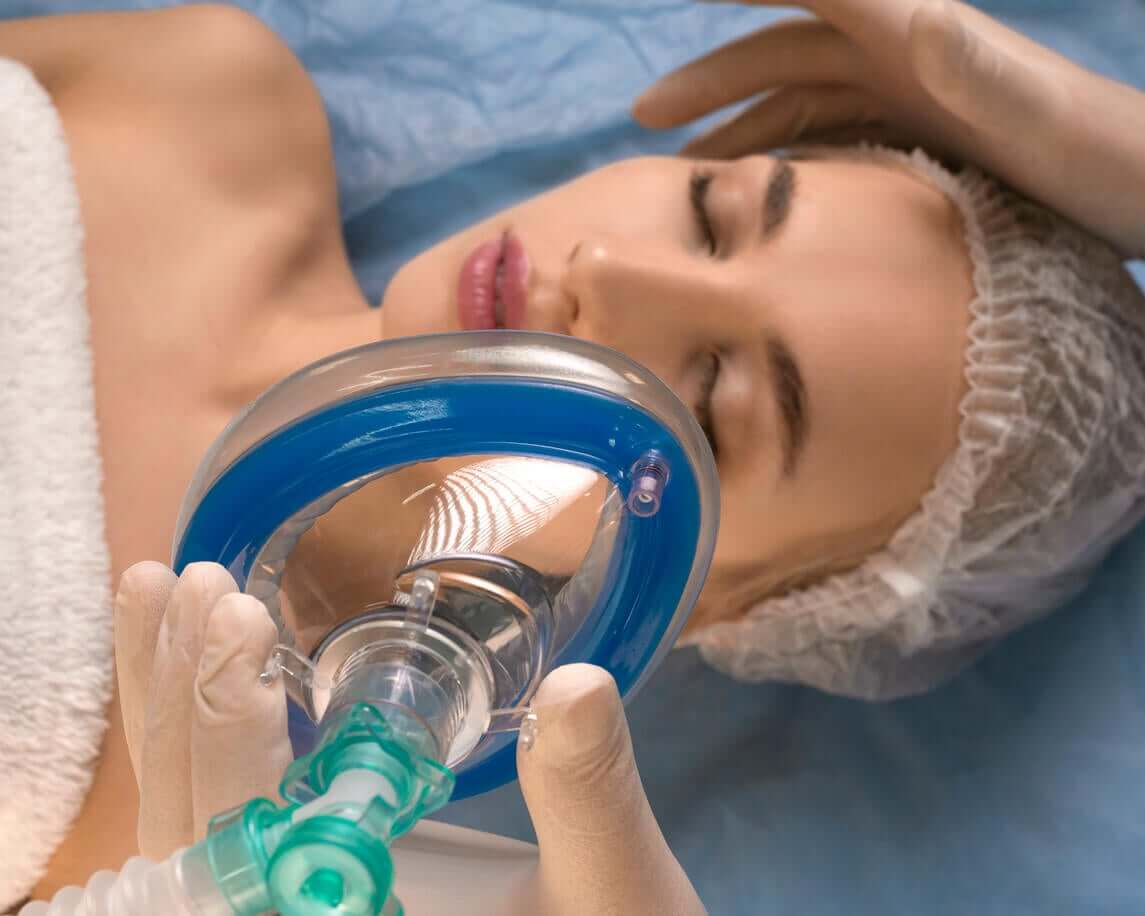
3. General anesthesia
This type of anesthesia is reserved for emergency situations, such as massive bleeding or advanced fetal distress. Likewise, for those cases in which loco-regional anesthesia is contraindicated, such as a severe bleeding disorder, a generalized infection, or diseases of the spine.
In this case, the drugs are administered intravenously and inhaled. The patient remains completely asleep and requires respiratory assistance and advanced life support throughout the procedure.
About the types of anesthesia in childbirth, we can say…
Labor anesthesia is a safe practice that has evolved a lot over the years.
At present, serious complications for mother and baby are low (maternal mortality is estimated at 5 per 1,000,000 births). On the other hand, the benefits obtained through it are considerable and very important to guarantee the well-being of both.
For this reason, if you’re about to give birth and want to know your options, talk to your obstetrician about it. Information is key to being able to make a conscious and correct decision.
The arrival of the baby is a very mobilizing event for the whole family, even more so for the mother who’s about to give birth. The sensations and experiences are so unique that it’s not possible to generalize them, much less put them into words. But if there’s something that most women have in common when it comes to giving birth, it’s pain, and that’s why today we’re going to tell you about the types of anesthesia that exist to have a less uncomfortable experience during labor and delivery.
As we always say, anticipation and prophylaxis strategies before delivery are very important. Still, we can’t deny or ignore the benefits of these pharmacological measures. With good information, we’ll be able to make better decisions. Keep reading to learn more.
The pain of childbirth, a unique experience
Surely you’ve wondered why there are women who can give birth without external help, while others come to faint from the pains of contractions. The explanation for this is quite simple: Pain is a relative and subjective sensation.
Next, we’ll share the latest definition of this sensation prepared by the International Association for the Study of Pain in 2020:
“Pain is an unpleasant sensory and emotional experience, associated with or similar to that associated with an actual or potential tissue injury.”
Experts in the field agree that labor pain is an individual response to the different stimuli that the woman receives. It means that these signals are received and interpreted in a unique way, as the context of each delivery is different (Hawkins, 2010). In this sense, physical sensations, emotions, motivation, previous experiences, and social and cultural components play a key role in the painful experience.
So, as pain is such a complex entity, it’s not always possible to control it voluntarily. In fact, many times, physiological responses to painful stimuli can put the well-being of mother and baby at risk. They can even interfere with the normal progression of labor. And in this sense, adequate anesthesia and analgesia can favor the desired outcome.
Types of anesthesia for childbirth

The main objective of anesthesia is to reduce the sensation of pain before an invasive or traumatic procedure, such as surgery or the delivery itself. For this, drugs are administered that cancel the sensitivity of a certain region of the body temporarily and reversibly. This is known as analgesia.
In some cases, it’s also necessary to relax the muscles or put a woman under in order to perform more complex procedures. These effects are myorelaxation and sedation, respectively.
In the case of delivery (either vaginal or by cesarean section), there are several types of anesthesia possible and the choice of one or the other is subject to individual circumstances. In this sense, not only are maternal preferences considered but medical staff also seek to provide the best care conditions for the pregnant woman and her baby.
As a practical matter, we’re going to classify the types of anesthesia for childbirth as follows:
- Local: This is the administration of the anesthetic in a specific area of the body, through an injection that’s placed in the subcutaneous cellular tissue (the one that’s below the dermal layer of the skin).
- Regional: In this case, the drug seeks to numb a certain region of the body. For example, the lower half of the body. In this case, the anesthetic is administered into the medullary canal.
- General: This type of anesthesia involves complete sedation of the patient (putting the woman into a stage of unconsciousness), muscle relaxation, and of course, analgesia. Medications are administered through the veins and require external ventilation and other advanced life support measures.
Some anatomical concepts
To understand each procedure, you need to know some basic notions regarding human anatomy. For example, it’s essential that you know where the painful stimulus circulates to understand why anesthetic drugs are administered in such a way.
Inside the skull is the brain, and this connects with the rest of the body’s organs through nerves. The latter are like wires that send sensitive information (such as pain or touch) from the viscera, muscles, or skin to the brain and in turn, return the “brain orders” to these tissues. The messages from the brain can be motor stimuli (such as removing your hand from a heat source) or behavioral (such as the urge to run away in fear), among others.
Nerves, in general, don’t leave directly from the brain, but from its attached structures: The brain stem and the spinal cord. The latter extends from the base of the head to almost the waist through a hole that remains within the vertebrae, called the canal or medullary canal.
Within the medullary canal, there are different cavities, as the medulla passes through it wrapped in membranes and liquid. One of the main medullary envelopes is called the dura mater, and according to this, the following spaces are defined:
- Epidural or epidural: This is the one that’s included between the bone of the vertebrae and the dura mater.
- Subdural or intradural: This is the space between the dura mater and the medulla, which is occupied by the cerebrospinal fluid.
Depending on the site where the drugs are administered and their characteristics, the different types of anesthesia may be carried out.
1. Local anesthesia
As we’ve mentioned, this type of anesthesia is used to block the sensitivity of a limited and determined area. For example, the perineal area where an episiotomy will be sutured in a mother who didn’t receive another type of anesthesia during childbirth.
This type of anesthesia is called infiltration and is done by injecting the drug through the skin of the vaginal frenulum. In this act, the thin fibers of the pudendal nerve are blocked and the woman loses sensitivity in this part of her vagina.
Due to the thinness of the tissue, it begins to act quickly and for a short period of time. Therefore, it’s ideal for performing the episiotomy and for its closure.
On the other hand, due to its short time of action and its localized effect, it’s not an adequate alternative to alleviate the pain of labor contractions.
2. Loco-regional anesthesia
This type of anesthesia is the most used for obstetric procedures, as it allows the blocking of intense pain in the lower half of the body. This way, the mother can go through the delivery in a more bearable way and avoid the adverse effects of the intolerable painful sensation.
Depending on the route of delivery (vaginal or cesarean section), one of the following techniques will be chosen:
- Epidural anesthesia: This is the most appropriate for vaginal delivery, as it allows the administration of medications in a sustained way over time. This is thanks to the placement of a thin catheter in the epidural space.
- Spinal anesthesia: This type of anesthesia favors the administration of higher doses of drugs, which allows a gradual numbing of the area for surgery. First, it blocks the pain, then the touch, and finally, the mobility of the muscles. In this case, the drug is injected into the subdural space only once before the surgical act.
To perform both procedures, a professional must perform a puncture on the mother’s back. But despite the fears, this’s done at a height where there’s no spinal cord, but rather thin filaments of it. Therefore, the risk of injuring it is quite low.
Like any invasive procedure, it has associated adverse effects, but in general, it’s a safe technique for both mother and baby.
3. General anesthesia
This type of anesthesia is reserved for emergency situations, such as massive bleeding or advanced fetal distress. Likewise, for those cases in which loco-regional anesthesia is contraindicated, such as a severe bleeding disorder, a generalized infection, or diseases of the spine.
In this case, the drugs are administered intravenously and inhaled. The patient remains completely asleep and requires respiratory assistance and advanced life support throughout the procedure.

About the types of anesthesia in childbirth, we can say…
Labor anesthesia is a safe practice that has evolved a lot over the years.
At present, serious complications for mother and baby are low (maternal mortality is estimated at 5 per 1,000,000 births). On the other hand, the benefits obtained through it are considerable and very important to guarantee the well-being of both.
For this reason, if you’re about to give birth and want to know your options, talk to your obstetrician about it. Information is key to being able to make a conscious and correct decision.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Analgesia obstétrica y anestesia. In: Cunningham F, Leveno KJ, Bloom SL, Dashe JS, Hoffman BL, Casey BM, Spong CY. eds. Williams Obstetricia. 25° edición. McGraw Hill; 2019.
- Chestnut D, Wong C, Tsen L, Ngan Kee W, Beilin Y, Mhyre J, Bateman B, Nathan N. Chestnut. Anestesia obstétrica. Principios y práctica. 6° edición. Elsevier España; 2020.
- Hawkins JL: Epidural analgesia for labor and delivery. N Engl J Med 362:1503, 2010. Disponible en: https://www.jvsmedicscorner.com/Anaesth-Obstetrics_files/Epidural%20Analgesia%20for%20Labor%20and%20Delivery.pdf
- Vijaya P. Borkar Patil, Jayshree J Upadhye. Anesthetic complications in cesarean section. International Journal of Research in Medical Sciences. 2018 Oct;6(10). Disponible en: http://dx.doi.org/10.18203/2320-6012.ijrms20183849.
- American Society of Anesthesiologists Task Force on Obstetric Anesthesia: Practice guidelines for obstetric anesthesia: an updated report by the American Society of Anesthesiologists Task Force on Obstetric Anesthesia. Anesthesiology February 2016, Vol. 124, 270–300. Disponible en: https://doi.org/10.1097/ALN.0000000000000935
- Practice Bulletin No. 177: Obstetric Analgesia and Anesthesia, Obstetrics & Gynecology: April 2017 – Volume 129 – Issue 4 – p e73-e89 Disponible en: https://doi: 10.1097/AOG.0000000000002018
- Pérez Fuentes J. Versión actualizada de la definición de dolor de la IASP: un paso adelante o un paso atrás. Rev. Soc. Esp. Dolor [Internet]. 2020 Ago [citado 2021 Dic 02] ; 27( 4 ): 232-233. Disponible en: http://scielo.isciii.es/scielo.php?script=sci_arttext&pid=S1134-80462020000400003&lng=es. Epub 13-Oct-2020. https://dx.doi.org/10.20986/resed.2020.3839/2020.
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








