Eczema in Babies: Characteristics and Treatment

Written and verified by the dermatologist Maria del Carmen Hernandez
Eczema in babies is one of the most common inflammatory skin diseases during childhood. It affects between 5 and 20% of children. Atopic eczema usually appears during the first year of life. In addition, most children who suffer from eczema are allergic to house dust mites. And, this is one of the main causes of aggravation of this condition.
What are the causes of eczema in babies?
Genetic factors, like the ones involved in encoding skin barrier proteins, like filaggrin, are important. However, they don’t explain the prevalence of this condition in all cases.
Babies who suffer from eczema have a higher risk of getting secondary skin infection. Besides, according to The Journal of Allergy and Clinical Immunology, this condition is usually linked to other immunoglobulin E (IgE) diseases, such as asthma, food allergies or allergic rhinitis.
Specific environmental exposure that would explain the risk of getting eczema is still unknown. However, exposure to microbes during early childhood and exposure to urban environments may be related to this disease.
What are the symptoms of eczema?
Eczema is an inflammatory skin disease, which makes your skin red and itchy. In addition, there are some related characteristics, such as:
- Peeling.
- Thickened skin (lichenification).
- Excoriation.
- Papules.
- Blisters.
- Suppuration.
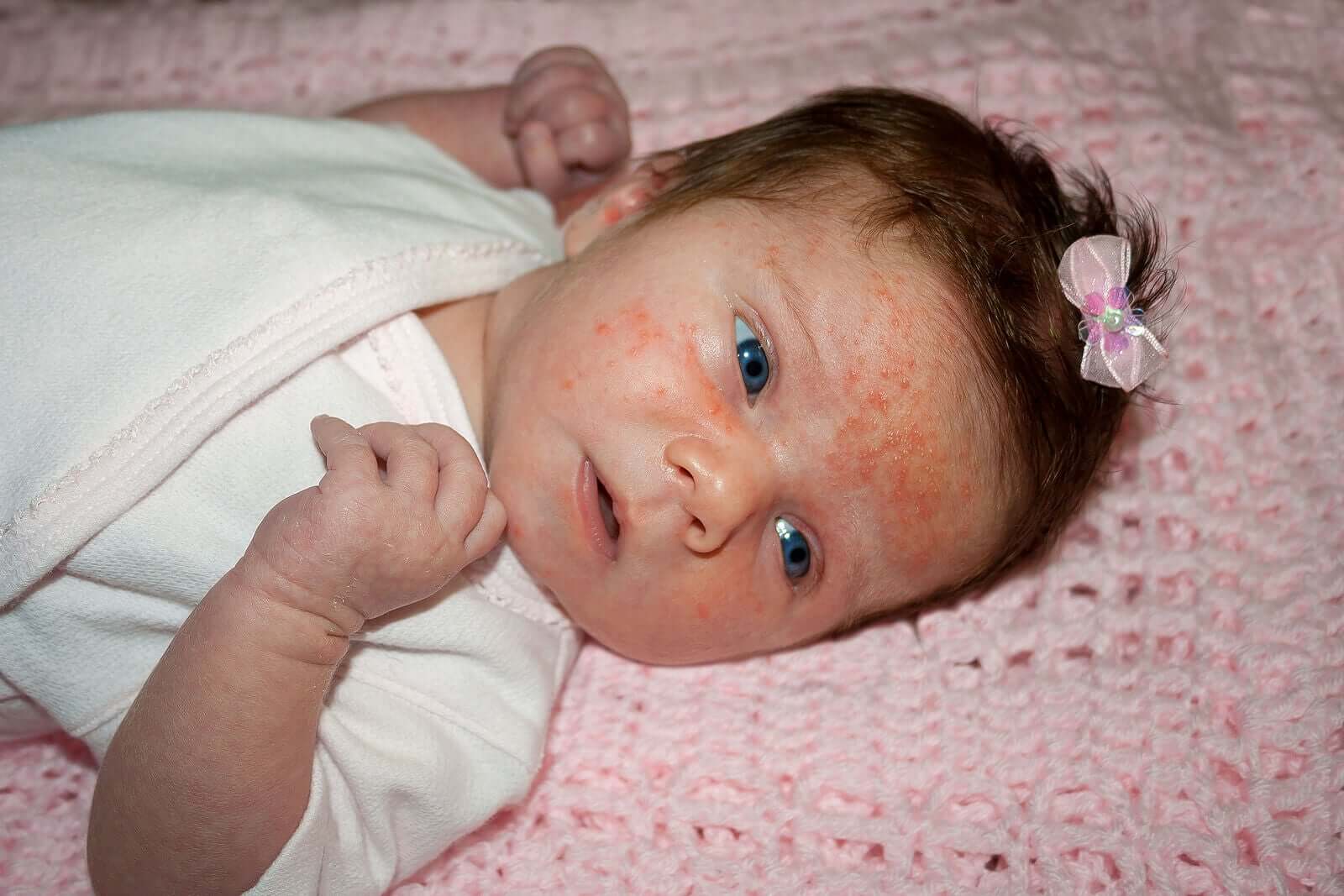
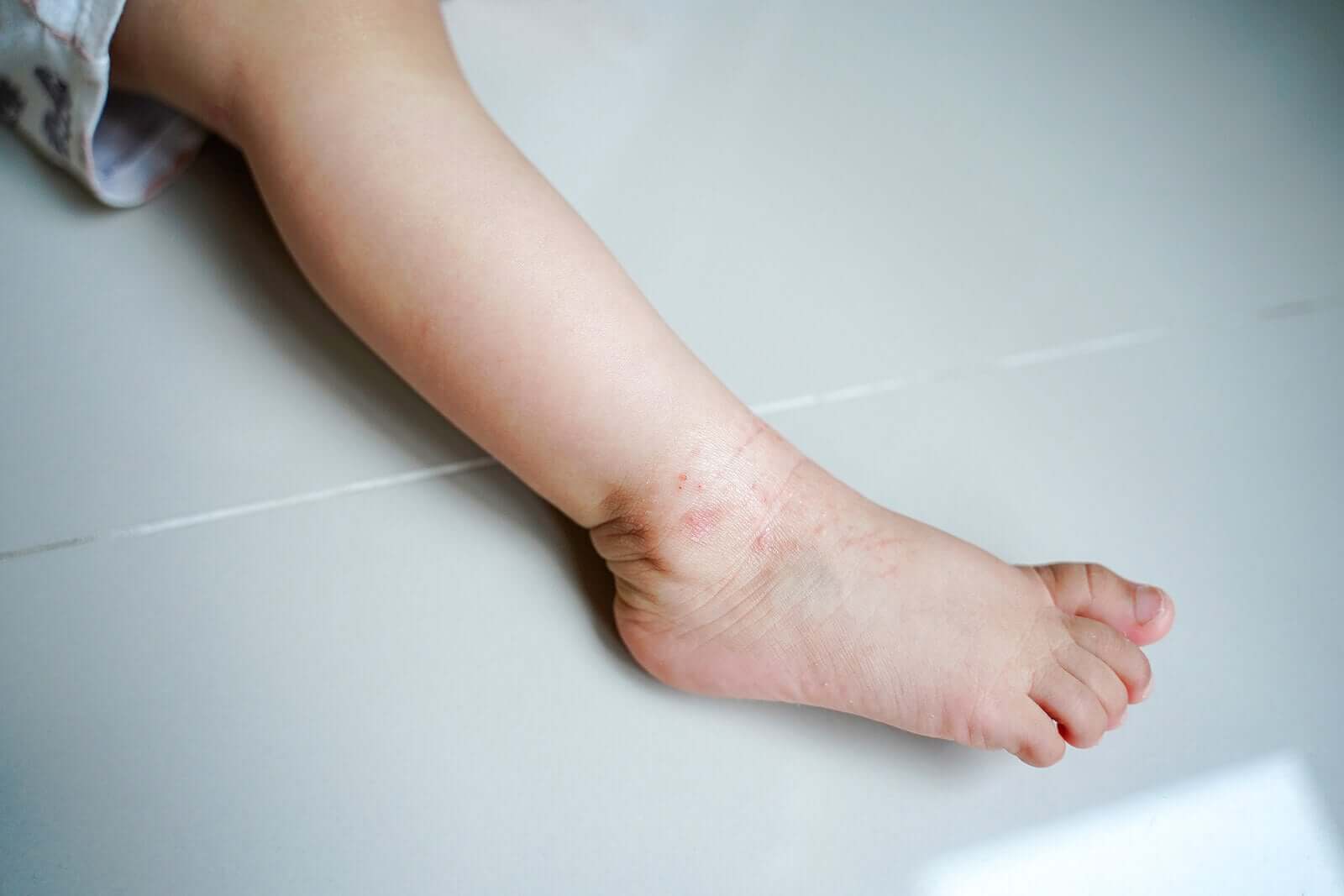
There’s a wide variety of atopic eczema, from minimal flexural eczema to erythroderma. Even though it can affect any part of the body, in babies it usually occurs on their cheeks, neck and skin folds of knees and elbows.
The importance of the skin barrier
The outer surface of the skin works as a physical and chemical barrier against external factors.
Babies with eczema suffer from a loss of the permeability barrier. Furthermore, their antimicrobial barrier is also compromised, which leads to a higher risk of skin infections. In more serious or advanced cases, there can be acute bacterial infections, which require another type of treatment.
Eczema treatment
Since eczema disrupts the skin barrier’s function, babies suffer from transepidermal water loss and from the ability to retain it. Besides, there’s a small amount of ceramides and intraepidermal lipids. So, how can you avoid eczema in babies?
Hygiene and bathing
Bathing oils and products with oatmeal are useful to prevent skin dryness, caused by taking baths. To avoid dehydration, baths should be short and warm.
Itching is the predominant symptom, which leads to scratching, and then more itching, forming a vicious circle. Perspiration or rough clothing, like wool may trigger this symptom.
Moisturizing
Babies with eczema tend to have dry skin. Also, humidity, cold weather and soaps usually aggravate this symptom. This is why it’s important to find the right moisturizer and apply it twice a day (with or without eczema).
Moisturizing helps improve skin dryness and itching. The ones that contain ceramides, essential oils and lipids are the best.
Avoiding allergens
House dust mites are the most important ones. Hence, you need to avoid them by covering your mattress and pillows, and washing your sheets using hot water (140 Fahrenheit degrees or higher).
If you think your baby may have food allergy, visit their pediatrician for proper treatment. Usually, babies with severe atopic eczema are allergic or intolerant to certain food.
Probiotics
Currently, there’s no evidence of the role that intestinal flora plays in this disease. And, there’s no evidence of the preventive effect of probiotics.
However, some studies suggest that they may prevent eczema, especially in babies who receive probiotics during their perinatal period.
What do you need to know about eczema in babies?
In conclusion, it’s a disease that may appear and disappear for years. Nowadays, there’s no treatment that can make it disappear forever. So, the best you can do is prevent it.
Furthermore, it’s important to handle predisposing factors. To do this, you have to use the proper moisturizer and maintain good hygiene.
Eczema in babies is one of the most common inflammatory skin diseases during childhood. It affects between 5 and 20% of children. Atopic eczema usually appears during the first year of life. In addition, most children who suffer from eczema are allergic to house dust mites. And, this is one of the main causes of aggravation of this condition.
What are the causes of eczema in babies?
Genetic factors, like the ones involved in encoding skin barrier proteins, like filaggrin, are important. However, they don’t explain the prevalence of this condition in all cases.
Babies who suffer from eczema have a higher risk of getting secondary skin infection. Besides, according to The Journal of Allergy and Clinical Immunology, this condition is usually linked to other immunoglobulin E (IgE) diseases, such as asthma, food allergies or allergic rhinitis.

Specific environmental exposure that would explain the risk of getting eczema is still unknown. However, exposure to microbes during early childhood and exposure to urban environments may be related to this disease.
What are the symptoms of eczema?
Eczema is an inflammatory skin disease, which makes your skin red and itchy. In addition, there are some related characteristics, such as:
- Peeling.
- Thickened skin (lichenification).
- Excoriation.
- Papules.
- Blisters.
- Suppuration.
There’s a wide variety of atopic eczema, from minimal flexural eczema to erythroderma. Even though it can affect any part of the body, in babies it usually occurs on their cheeks, neck and skin folds of knees and elbows.
The importance of the skin barrier
The outer surface of the skin works as a physical and chemical barrier against external factors.
Babies with eczema suffer from a loss of the permeability barrier. Furthermore, their antimicrobial barrier is also compromised, which leads to a higher risk of skin infections. In more serious or advanced cases, there can be acute bacterial infections, which require another type of treatment.
Eczema treatment
Since eczema disrupts the skin barrier’s function, babies suffer from transepidermal water loss and from the ability to retain it. Besides, there’s a small amount of ceramides and intraepidermal lipids. So, how can you avoid eczema in babies?
Hygiene and bathing
Bathing oils and products with oatmeal are useful to prevent skin dryness, caused by taking baths. To avoid dehydration, baths should be short and warm.
Itching is the predominant symptom, which leads to scratching, and then more itching, forming a vicious circle. Perspiration or rough clothing, like wool may trigger this symptom.
Moisturizing
Babies with eczema tend to have dry skin. Also, humidity, cold weather and soaps usually aggravate this symptom. This is why it’s important to find the right moisturizer and apply it twice a day (with or without eczema).

Moisturizing helps improve skin dryness and itching. The ones that contain ceramides, essential oils and lipids are the best.
Avoiding allergens
House dust mites are the most important ones. Hence, you need to avoid them by covering your mattress and pillows, and washing your sheets using hot water (140 Fahrenheit degrees or higher).
If you think your baby may have food allergy, visit their pediatrician for proper treatment. Usually, babies with severe atopic eczema are allergic or intolerant to certain food.
Probiotics
Currently, there’s no evidence of the role that intestinal flora plays in this disease. And, there’s no evidence of the preventive effect of probiotics.
However, some studies suggest that they may prevent eczema, especially in babies who receive probiotics during their perinatal period.
What do you need to know about eczema in babies?
In conclusion, it’s a disease that may appear and disappear for years. Nowadays, there’s no treatment that can make it disappear forever. So, the best you can do is prevent it.
Furthermore, it’s important to handle predisposing factors. To do this, you have to use the proper moisturizer and maintain good hygiene.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Shelov SP, Hannemann R, editors. The Complete and Authoritative Guide. 4. New York: NY Bantam Books; 2004. Caring for your baby and young child:brith to age
- Biagini Myers JM, Khurana Hershey GK. Eczema in early life: genetics, the skin barrier, and lessons learned from birth cohort studies. J Pediatr. 2010;157(5):704-714. doi:10.1016/j.jpeds.2010.07.009
- Bieber T. Atopic dermatitis. N Engl J Med. 2008 Apr 3;358(14):1483-94. doi: 10.1056/NEJMra074081. PMID: 18385500.
- Sugarman JL. The epidermal barrier in atopic dermatitis. Semin Cutan Med Surg. 2008 Jun;27(2):108-14. doi: 10.1016/j.sder.2008.04.005. PMID: 18620132.
- Beck LA, Leung DY. Allergen sensitization through the skin induces systemic allergic responses. J Allergy Clin Immunol. 2000 Nov;106(5 Suppl):S258-63. https://pubmed.ncbi.nlm.nih.gov/11080741/
- Björkstén B, Sepp E, Julge K, Voor T, Mikelsaar M. Allergy development and the intestinal microflora during the first year of life. J Allergy Clin Immunol. 2001 Oct;108(4):516-20. https://pubmed.ncbi.nlm.nih.gov/11590374/
- Kalliomäki M, Salminen S, Arvilommi H, Kero P, Koskinen P, Isolauri E. Probiotics in primary prevention of atopic disease: a randomised placebo-controlled trial. Lancet. 2001 Apr 7;357(9262):1076-9. https://pubmed.ncbi.nlm.nih.gov/11297958/
- Palmer, C. N., Irvine, A. D., Terron-Kwiatkowski, A., Zhao, Y., Liao, H., Lee, S. P., … & O’Regan, G. M. (2006). Common loss-of-function variants of the epidermal barrier protein filaggrin are a major predisposing factor for atopic dermatitis. Nature genetics, 38(4), 441-446. https://pubmed.ncbi.nlm.nih.gov/16550169/
- Lodén, M. (2003). Role of topical emollients and moisturizers in the treatment of dry skin barrier disorders. American journal of clinical dermatology, 4(11), 771-788. https://pubmed.ncbi.nlm.nih.gov/14572299/
- Edwards, C., & Marks, R. (2004). 2 A Hydration and Atopic Dermatitis. Bioengineering of the skin: water and the stratum corneum, 323. https://www.researchgate.net/publication/329487011_Hydration_and_atopic_dermatitis
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








