Ringworm in Babies and Children: Symptoms, Causes, and Treatment

Written and verified by the dermatologist Maria del Carmen Hernandez
Ringworm in babies and children is a condition that occurs quite frequently on the skin, nails, and hair. In turn, it’s caused by microscopic fungi that, according to the area of the body they affect, are called by different names. This skin infection has several therapeutic options you can put into practice. In this article, we’ll tell you more about it.
Ringworm in babies and children
Ringworm is an infection of the skin surface, hair, or nails caused by dermatophytes, which are agents with the ability to adhere to the keratinized tissue of the skin. In fact, it’s explicitly defined by the location of the lesions it can produce.
Ringworm of the body
Ringworm of the body is very common worldwide. Excessive heat, relative humidity, and tight clothing have correlations with frequent and more serious cases. The infection manifests as pink or blushing spots that are circular in shape and have raised, scaly borders, and a fair tendency to lighten toward the center.
Localized tinea corporis responds to topical therapy applied once or twice daily over the course of two to three weeks. Topical options include clotrimazole, ketoconazole, miconazole, terbinafine, and naftifine. In addition, oral medication is necessary in more generalized infections or in cases where treatment has failed. In fact, itraconazole and oral terbinafine are the preferred first-line treatments.
Read also: What to Do If Your Child Has Foot Fungus
Tinea pedis

Ringworm of the foot, also known as athlete’s foot, is an infection that affects the interdigital spaces, nails, and soles of the feet. Common risk factors include the following:
- Excessive sweating
- Prolonged use of occlusive footwear
- A hot and humid environment
- Prolonged exposure to water
Imidazoles such as econazole, clotrimazole, ketoconazole, miconazole, isoconazole, thioconazole, and sulconazole, are effective drugs in tinea capitis with a very low incidence of adverse reactions.
Tinea capitis
Tinea capitis and tinea corporis are the most common dermatophyte infections in prepubertal children. It’s caused by the dermatophyte species Microsporum and Trichophyton. It’s a fungal infection of the scalp hairs. According to the clinical appearance, it can be divided into inflammatory and non-inflammatory types. The first type may result in the following:
- Kerion: Its appearance involves inflammation and may progress to cicatricial alopecia.
- Painful pus nodule: Inflammatory infection with the presence of abscesses, crusts, or nodules.
- Alopecia cicatricial.
In most cases, the systemic antifungal drug of choice is griseofulvin. Therefore, the topical alternative isn’t recommended as it’s ineffective.
Nail ringworm
Onychomycosis is an infection caused by fungi. When these are dermatophytes, it’s called tinea unguium. Toenails are the most frequently infected. The most effective treatments for onychomycosis are systemic antifungals, although newer topical therapies have improved cure rates.
According to the American Academy of Dermatology Association, nails that are infected by dermatophytes are characterized by darker or yellowish coloration, brittleness, and flaking. These systemic drugs usually take 4 months before completely replacing the infected nail with a new one.
You may be interested in: Color Changes in Children’s Nails: What Do They Mean?
Ringworm of the groin
This is an infection caused by dermatophytes that find favorable environments in which there’s sweating, maceration, and alkaline pH. It affects the skin of the pubic, genital, perineal, and perianal regions. Therefore, there are several risk factors that predispose a person to jock itch, such as excessive sweating, inadequate hygiene, occlusive clothing, diabetes mellitus, immunosuppression, and low socioeconomic status.
In these cases, topical therapies are effective and preferred. In fact, allylamines and azoles are the mainstay of topical treatment regimens and are indicated once to twice daily for two to four weeks.
Ringworm in babies and children
The prognosis for ringworm in infants and children is good as long as preventive measures are taken. Experts warn against implementing home remedies or measures but recommend going to the doctor for the most appropriate indication. Although these aren’t serious conditions, their management and care shouldn’t be postponed due to their great capacity to spread and to be a gateway for various bacterial infections.
Ringworm in babies and children is a condition that occurs quite frequently on the skin, nails, and hair. In turn, it’s caused by microscopic fungi that, according to the area of the body they affect, are called by different names. This skin infection has several therapeutic options you can put into practice. In this article, we’ll tell you more about it.
Ringworm in babies and children
Ringworm is an infection of the skin surface, hair, or nails caused by dermatophytes, which are agents with the ability to adhere to the keratinized tissue of the skin. In fact, it’s explicitly defined by the location of the lesions it can produce.
Ringworm of the body
Ringworm of the body is very common worldwide. Excessive heat, relative humidity, and tight clothing have correlations with frequent and more serious cases. The infection manifests as pink or blushing spots that are circular in shape and have raised, scaly borders, and a fair tendency to lighten toward the center.
Localized tinea corporis responds to topical therapy applied once or twice daily over the course of two to three weeks. Topical options include clotrimazole, ketoconazole, miconazole, terbinafine, and naftifine. In addition, oral medication is necessary in more generalized infections or in cases where treatment has failed. In fact, itraconazole and oral terbinafine are the preferred first-line treatments.
Read also: What to Do If Your Child Has Foot Fungus
Tinea pedis

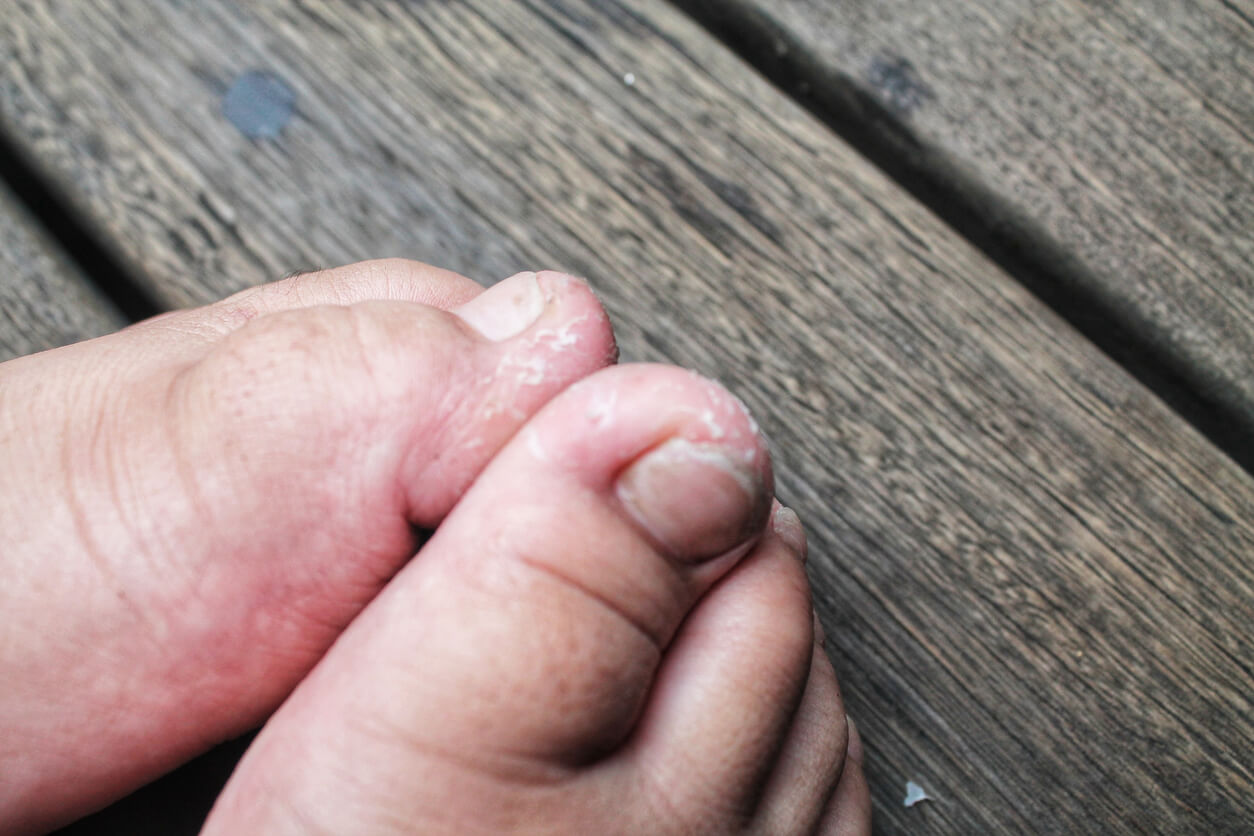
Ringworm of the foot, also known as athlete’s foot, is an infection that affects the interdigital spaces, nails, and soles of the feet. Common risk factors include the following:
- Excessive sweating
- Prolonged use of occlusive footwear
- A hot and humid environment
- Prolonged exposure to water
Imidazoles such as econazole, clotrimazole, ketoconazole, miconazole, isoconazole, thioconazole, and sulconazole, are effective drugs in tinea capitis with a very low incidence of adverse reactions.
Tinea capitis
Tinea capitis and tinea corporis are the most common dermatophyte infections in prepubertal children. It’s caused by the dermatophyte species Microsporum and Trichophyton. It’s a fungal infection of the scalp hairs. According to the clinical appearance, it can be divided into inflammatory and non-inflammatory types. The first type may result in the following:
- Kerion: Its appearance involves inflammation and may progress to cicatricial alopecia.
- Painful pus nodule: Inflammatory infection with the presence of abscesses, crusts, or nodules.
- Alopecia cicatricial.
In most cases, the systemic antifungal drug of choice is griseofulvin. Therefore, the topical alternative isn’t recommended as it’s ineffective.
Nail ringworm
Onychomycosis is an infection caused by fungi. When these are dermatophytes, it’s called tinea unguium. Toenails are the most frequently infected. The most effective treatments for onychomycosis are systemic antifungals, although newer topical therapies have improved cure rates.
According to the American Academy of Dermatology Association, nails that are infected by dermatophytes are characterized by darker or yellowish coloration, brittleness, and flaking. These systemic drugs usually take 4 months before completely replacing the infected nail with a new one.
You may be interested in: Color Changes in Children’s Nails: What Do They Mean?

Ringworm of the groin
This is an infection caused by dermatophytes that find favorable environments in which there’s sweating, maceration, and alkaline pH. It affects the skin of the pubic, genital, perineal, and perianal regions. Therefore, there are several risk factors that predispose a person to jock itch, such as excessive sweating, inadequate hygiene, occlusive clothing, diabetes mellitus, immunosuppression, and low socioeconomic status.
In these cases, topical therapies are effective and preferred. In fact, allylamines and azoles are the mainstay of topical treatment regimens and are indicated once to twice daily for two to four weeks.
Ringworm in babies and children
The prognosis for ringworm in infants and children is good as long as preventive measures are taken. Experts warn against implementing home remedies or measures but recommend going to the doctor for the most appropriate indication. Although these aren’t serious conditions, their management and care shouldn’t be postponed due to their great capacity to spread and to be a gateway for various bacterial infections.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Ely JW, Rosenfeld S, Seabury Stone M. Diagnosis and management of tinea infections. Am Fam Physician. 2014 Nov 15;90(10):702-10. PMID: 25403034.
- Noble SL, Forbes RC, Stamm PL. Diagnosis and management of common tinea infections. Am Fam Physician. 1998 Jul;58(1):163-74, 177-8. PMID: 9672436.
- Sahoo AK, Mahajan R. Management of tinea corporis, tinea cruris, and tinea pedis: A comprehensive review. Indian Dermatol Online J. 2016 Mar-Apr;7(2):77-86. doi: 10.4103/2229-5178.178099. PMID: 27057486; PMCID: PMC4804599.
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








