Cutaneous Mycoses in Children

Written and verified by the dermatologist Maria del Carmen Hernandez
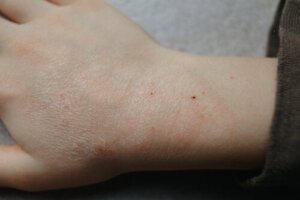
Cutaneous mycoses in children are frequent skin and adnexal conditions. These manifestations are caused by fungi that are characterized by growing on keratin (skin, nails, and hair).
These mycoses are superficial and make up about 10% of the consultations with dermatologists. Under the indicated treatment, they go away effectively and quickly.
Cutaneous mycoses in children

Tinea or dermatophytosis
In this condition, the type of fungus involved isn’t part of the normal skin flora. In turn, transmission can occur by direct contact with infected humans or animals, or indirectly with contaminated fomites.
Dermatophytosis is a superficial fungal infection caused by keratinophilic fungi:
- Trichophyton Erythrasma: Infects the skin, nails, and hair.
- Microsporum Erythrasma: Alters the skin surface and hair.
- Epidermophyton Erythrasma: Causes alteration of the skin and nails.
Clinical manifestations
Clinical manifestations vary depending on the causative agent and the immune response of the child; they may last for months or years. They may even be asymptomatic or only expressed by itching. Certain clinical signs predominate depending on the region of the body affected. These manifestations may include the following:
- Scalp lesions (tinea capitis).
- Generalized involvement (tinea corporis).
- Lesions in the interdigital spaces and plantar regions of the foot (tinea pedis).
- Lesions on the nail (tinea unguium).
In very special cases, a complication of tinea capitis called Kerion (or inflammatory tinea capitis of the head) may occur. According to an article in Medigraphic, this condition is primarily associated with Microsporum canis infection and is considered difficult to manage.
Diagnosis and treatment of tinea capitis
Diagnosis is established by observation of the manifestations of the disease and by the particular distribution of lesions on the body. In cases where there’s some doubt in determining the diagnosis of certainty, direct examination is used to confirm the diagnosis.
During clinical examination, several differential diagnoses may be raised depending on the site of the lesions. These include seborrheic dermatitis, cutaneous manifestations of lupus, and psoriasis.
According to the Journal Dermatology Online Journal, the first-line therapeutic option is topical antifungal agents, mostly imidazole antifungals. When topical treatment is ineffective, oral antifungal agents are used:
- Terbinafine
- Itraconazole
- Ketoconazole
- Fluconazole
Read also: 10 Home Remedies for Skin Fungus
Mucocutaneous candidiasis
Mucocutaneous candidiasis are infections located on the mucous membranes and skin surface generated by the yeast of the genus Candida. In turn, it can affect the nails and, in a lesser number of cases, the hair follicle.
There are several clinical presentations that occur in a localized manner. Some of them are the following:
- Thrush (oral candidiasis)
- Candidiasis (candidiasis)
- Miliaria variants
- Paronychia-onychomycosis
- Interdigital variant
- Perioral dermatitis
Oral Candidiasis
Candida can give rise to thrush or oral candidiasis in children who have a weakened immune system due to some cause. It usually appears in infants and newborns. Consequently, the diagnosis is made on the basis of the clinical manifestations in children.
Oral candidiasis is characterized by white pseudomembranous plaques. It may even affect the hard and soft palate, tongue, and oral mucosa.
In turn, loss of taste and angular cheilitis (cracking of the skin at the corners of the mouth in children) may also occur.
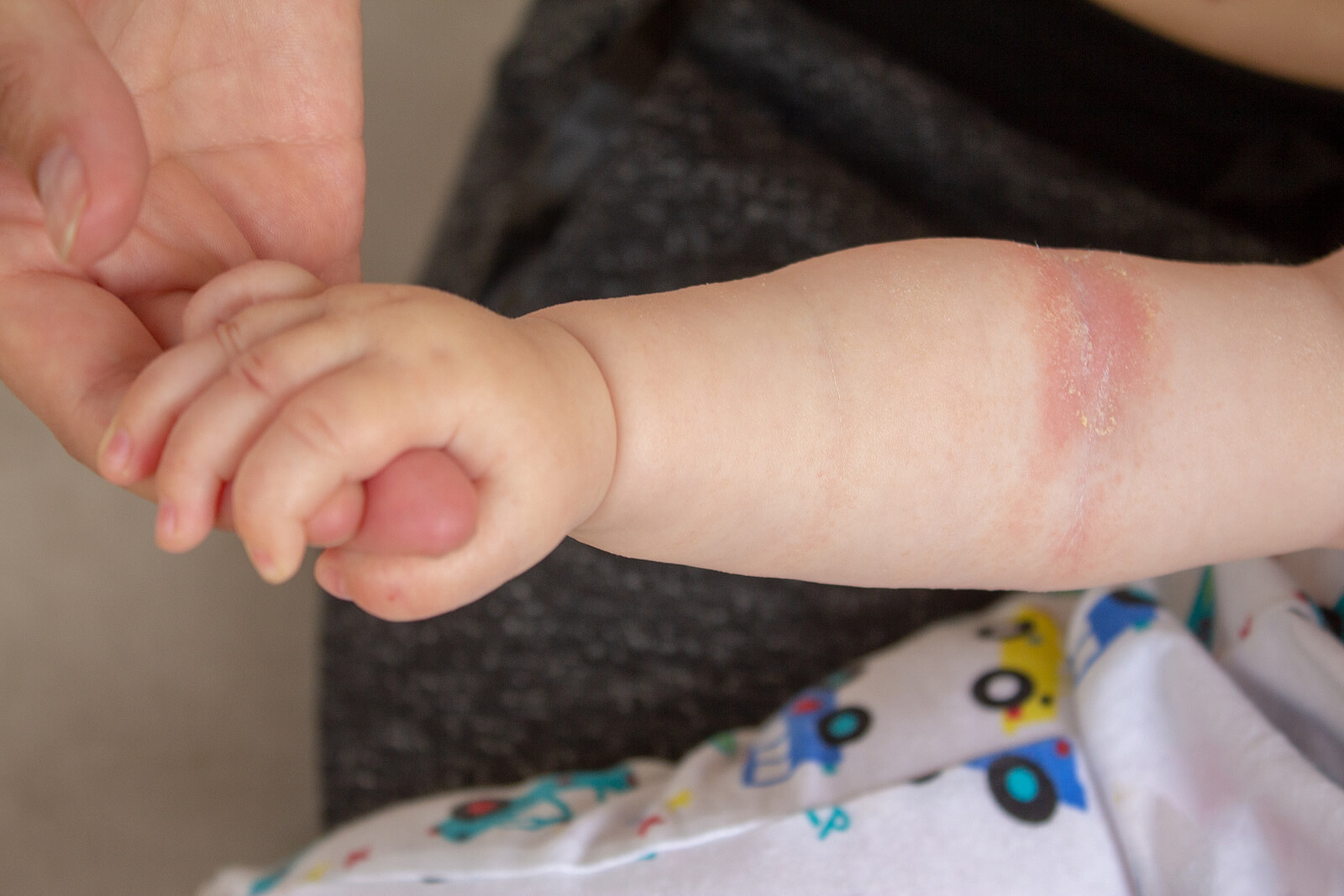
Cutaneous candidiasis
Candida infection in fold regions is a common condition in children. It may even be one of the main causes of diaper rash in infants.
Dermatitis caused by this fungal species is characterized by erythema and scaly plaques, accompanied by eczema. In addition, in the most severe cases, erosions or ulcerations may occur.
The differential diagnoses that may be considered at the time of medical consultation are the following:
- Seborrheic dermatitis
- Psoriasis
- Erythrasma
You may be interested in: Oral candidiasis in children: symptoms, causes and treatment
Pityriasis Versicolor
Pityriasis Versicolor is a common and benign superficial fungal infection of the skin. In turn, it’s characterized by hypopigmented or hyperpigmented fine scaly macules.
It’s an infection that develops chronically and usually recurs at different times. However, it should be treated equally upon diagnosis.
The most prevalent location is on the seborrheic areas of the body, i.e. trunk, neck, and proximal extremities. Multiple well-demarcated, oval-shaped patches are seen in these areas.
As for differential diagnoses, pityriasis Versicolor lesions can be confused with pityriasis rosea, vitiligo, and leukoderma.
Treatment of Pityriasis Versicolor
Skin lesions are usually asymptomatic or mildly pruritic (itchy). Therefore, they can be effectively treated with topical and systemic agents. Thus, according to the journal Fungi, topical antifungal treatments are considered the first line of defense against Pityriasis Versicolor.
Parents should be informed that the triggering agent for Pityriasis Versicolor is a commensal fungus that inhabits the normal skin flora and therefore the condition isn’t considered contagious.
Regarding cutaneous mycoses in children
Cutaneous mycoses are common in children. In turn, these skin manifestations can negatively affect the quality of life of young children. Therefore, even if these diseases aren’t serious for the child who suffers from them, a specialist should be consulted at the first sign of symptoms.
Cutaneous mycoses in children are frequent skin and adnexal conditions. These manifestations are caused by fungi that are characterized by growing on keratin (skin, nails, and hair).
These mycoses are superficial and make up about 10% of the consultations with dermatologists. Under the indicated treatment, they go away effectively and quickly.
Cutaneous mycoses in children

Tinea or dermatophytosis
In this condition, the type of fungus involved isn’t part of the normal skin flora. In turn, transmission can occur by direct contact with infected humans or animals, or indirectly with contaminated fomites.
Dermatophytosis is a superficial fungal infection caused by keratinophilic fungi:
- Trichophyton Erythrasma: Infects the skin, nails, and hair.
- Microsporum Erythrasma: Alters the skin surface and hair.
- Epidermophyton Erythrasma: Causes alteration of the skin and nails.
Clinical manifestations
Clinical manifestations vary depending on the causative agent and the immune response of the child; they may last for months or years. They may even be asymptomatic or only expressed by itching. Certain clinical signs predominate depending on the region of the body affected. These manifestations may include the following:
- Scalp lesions (tinea capitis).
- Generalized involvement (tinea corporis).
- Lesions in the interdigital spaces and plantar regions of the foot (tinea pedis).
- Lesions on the nail (tinea unguium).
In very special cases, a complication of tinea capitis called Kerion (or inflammatory tinea capitis of the head) may occur. According to an article in Medigraphic, this condition is primarily associated with Microsporum canis infection and is considered difficult to manage.
Diagnosis and treatment of tinea capitis
Diagnosis is established by observation of the manifestations of the disease and by the particular distribution of lesions on the body. In cases where there’s some doubt in determining the diagnosis of certainty, direct examination is used to confirm the diagnosis.
During clinical examination, several differential diagnoses may be raised depending on the site of the lesions. These include seborrheic dermatitis, cutaneous manifestations of lupus, and psoriasis.
According to the Journal Dermatology Online Journal, the first-line therapeutic option is topical antifungal agents, mostly imidazole antifungals. When topical treatment is ineffective, oral antifungal agents are used:
- Terbinafine
- Itraconazole
- Ketoconazole
- Fluconazole
Read also: 10 Home Remedies for Skin Fungus
Mucocutaneous candidiasis
Mucocutaneous candidiasis are infections located on the mucous membranes and skin surface generated by the yeast of the genus Candida. In turn, it can affect the nails and, in a lesser number of cases, the hair follicle.
There are several clinical presentations that occur in a localized manner. Some of them are the following:
- Thrush (oral candidiasis)
- Candidiasis (candidiasis)
- Miliaria variants
- Paronychia-onychomycosis
- Interdigital variant
- Perioral dermatitis
Oral Candidiasis
Candida can give rise to thrush or oral candidiasis in children who have a weakened immune system due to some cause. It usually appears in infants and newborns. Consequently, the diagnosis is made on the basis of the clinical manifestations in children.
Oral candidiasis is characterized by white pseudomembranous plaques. It may even affect the hard and soft palate, tongue, and oral mucosa.
In turn, loss of taste and angular cheilitis (cracking of the skin at the corners of the mouth in children) may also occur.
Cutaneous candidiasis
Candida infection in fold regions is a common condition in children. It may even be one of the main causes of diaper rash in infants.
Dermatitis caused by this fungal species is characterized by erythema and scaly plaques, accompanied by eczema. In addition, in the most severe cases, erosions or ulcerations may occur.
The differential diagnoses that may be considered at the time of medical consultation are the following:
- Seborrheic dermatitis
- Psoriasis
- Erythrasma

You may be interested in: Oral candidiasis in children: symptoms, causes and treatment
Pityriasis Versicolor
Pityriasis Versicolor is a common and benign superficial fungal infection of the skin. In turn, it’s characterized by hypopigmented or hyperpigmented fine scaly macules.
It’s an infection that develops chronically and usually recurs at different times. However, it should be treated equally upon diagnosis.
The most prevalent location is on the seborrheic areas of the body, i.e. trunk, neck, and proximal extremities. Multiple well-demarcated, oval-shaped patches are seen in these areas.
As for differential diagnoses, pityriasis Versicolor lesions can be confused with pityriasis rosea, vitiligo, and leukoderma.
Treatment of Pityriasis Versicolor
Skin lesions are usually asymptomatic or mildly pruritic (itchy). Therefore, they can be effectively treated with topical and systemic agents. Thus, according to the journal Fungi, topical antifungal treatments are considered the first line of defense against Pityriasis Versicolor.
Parents should be informed that the triggering agent for Pityriasis Versicolor is a commensal fungus that inhabits the normal skin flora and therefore the condition isn’t considered contagious.
Regarding cutaneous mycoses in children
Cutaneous mycoses are common in children. In turn, these skin manifestations can negatively affect the quality of life of young children. Therefore, even if these diseases aren’t serious for the child who suffers from them, a specialist should be consulted at the first sign of symptoms.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Gupta AK, Summerbell RC. Tinea capitis. Med Mycol. 2000 Aug;38(4):255-87. doi: 10.1080/mmy.38.4.255.287. PMID: 10975696.
- Sahoo, A. K., & Mahajan, R. (2016). Management of tinea corporis, tinea cruris, and tinea pedis: A comprehensive review. Indian dermatology online journal, 7(2), 77–86. https://doi.org/10.4103/2229-5178.178099
- Millsop JW, Fazel N. Oral candidiasis. Clin Dermatol. 2016 Jul-Aug;34(4):487-94. doi: 10.1016/j.clindermatol.2016.02.022. Epub 2016 Mar 2. PMID: 27343964.
- Hellstein JW, Marek CL. Candidiasis: Red and White Manifestations in the Oral Cavity. Head Neck Pathol. 2019 Mar;13(1):25-32. doi: 10.1007/s12105-019-01004-6. Epub 2019 Jan 29. PMID: 30693459; PMCID: PMC6405794.
- Bonifaz A, Rojas R, Tirado-Sánchez A, Chávez-López D, Mena C, Calderón L, María PO. Superficial Mycoses Associated with Diaper Dermatitis. Mycopathologia. 2016 Oct;181(9-10):671-9. doi: 10.1007/s11046-016-0020-9. Epub 2016 May 19. PMID: 27193417; PMCID: PMC5014885.
- Gupta AK, Foley KA. Antifungal Treatment for Pityriasis Versicolor. J Fungi (Basel). 2015 Mar 12;1(1):13-29. doi: 10.3390/jof1010013. PMID: 29376896; PMCID: PMC5770013.
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








