Color Changes in Children's Nails: What Do They Mean?

Written and verified by the pediatrician Marcela Alejandra Caffulli
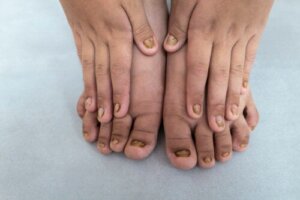
Nails protect the most outer tips of our bodies–our fingertips and toes. Their presence facilitates manual skills, improves the perception of touch, and fulfills an aesthetic function. Therefore, color changes in children’s nails can be a cause for great concern in parents.
In many cases, these modifications are due to trivial causes, while in others, they can alert us to the presence of more serious diseases.
Do you want to know why this color change occurs? Coming up next, we’ll tell you everything you need to know.
The normal development of children’s nails
The first traces of nails appear in the ninth week of gestation and, by week 20, all are fully formed. Growth continues throughout life and varies depending on the presence of certain factors, such as age, sex, nutrition, and disease.
Nails have several components, among which the following stand out:
- Nail plate: This is a rigid and translucent structure with a rectangular shape and a smooth surface and edges. It’s the most superficial and visible part.
- Nail bed: This is the layer that’s immediately under the plate. It’s pale pink in color, as blood vessels, nerves, and lymphatic vessels circulate through it.
- Nail matrix: This is a vital structure that manufactures the nail plate. It’s found under the skin and appears as a white crescent at the base of the nail (the lunula).
- Nail folds and cuticles: These are layers of skin that fold over on three edges of the plate in order to seal the nails and prevent germs from entering the matrix. They’re the same tone as the rest of the skin.
Pathological color changes in children’s nails
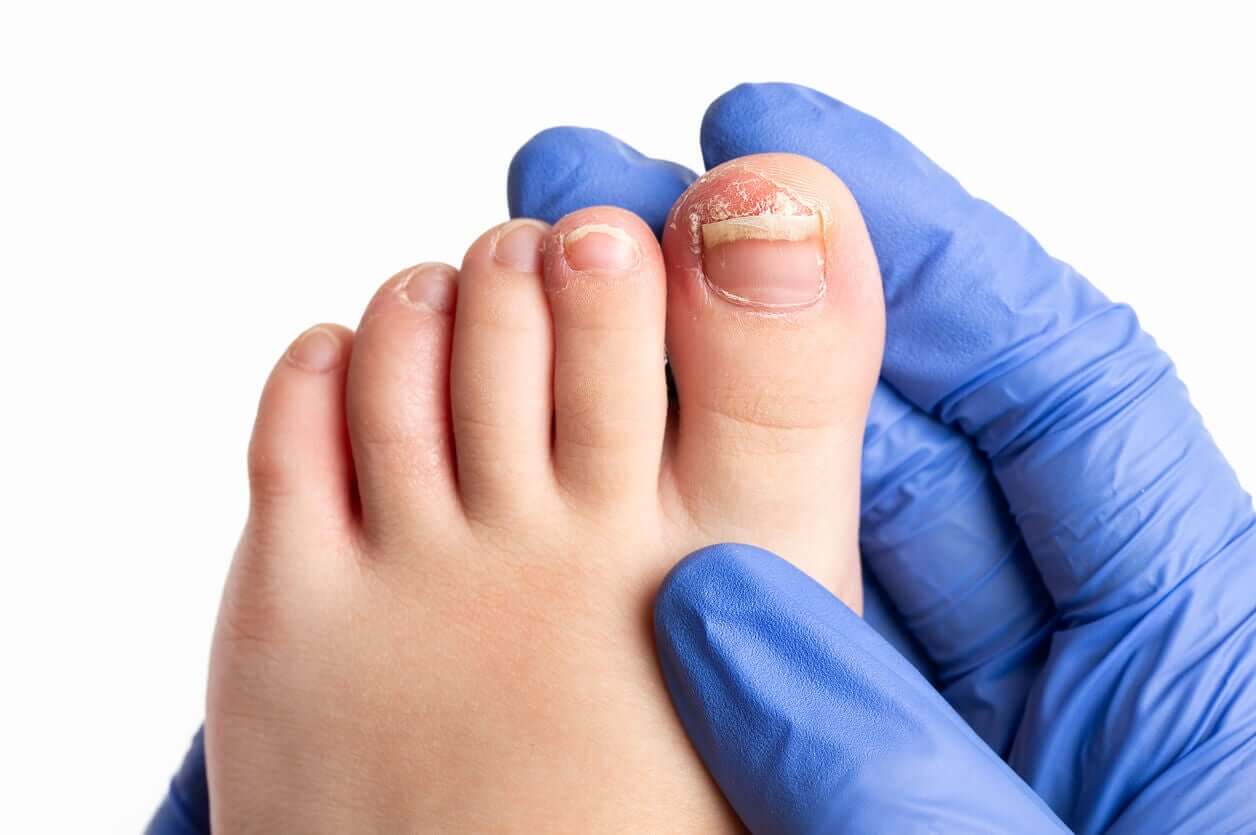
Any modification in the usual appearance of the nails warrants a consultation with a doctor.
Some of these changes can be present from birth and are part of some congenital diseases. But others can be acquired in later stages and indicate the presence of local illnesses (in the proximity of the nail) or at a distance.
Among the alterations in the appearance of the nails, are color changes. These range from small spots to a complete change from the usual hue.
Next, we’ll describe the illnesses that are associated with each color of children’s nails.
White
- Minor trauma
- Congenital candidiasis (yeast infection)
- Stevens-Johnson syndrome (acute and severe skin disease)
- Chemotherapy drugs (cancer drugs)
- Acrodermatitis enteropathica (innate metabolic disease)
- Heart failure (heart pump failure)
- Vitiligo (absence of skin pigments)
- Taking certain antibiotics, such as sulfonamides
- Noonan syndrome (genetic disease)
- Severe anemia
- Low levels of protein in the blood
Black
- Melanocytic nevus (moles)
- Melanoma (skin tumor)
- Taking certain drugs, such as cyclophosphamide (immunosuppressant)
- Severe trauma (for example, being slammed in a door)
- Paronychia (infections in nail folds)
Red
- Vascular tumors
- Paronychia or infections
- Petechiae dot-like skin bleeds)
- Autoimmune diseases such as lupus or rheumatoid arthritis
- Porphyrias (blood disease)
- Lichen planus (inflammatory skin disease)
- Bruising or bleeding below the nail bed
Blue or gray
- Ink stains
- The use of nail polish
- Cyanide, carbon monoxide, silver, or copper poisoning
- The use of some antibiotics, such as minocycline
- Chemotherapeutic agents
- A low level of oxygen in the blood, as occurs in severe respiratory distress
Yellow
- Tobacco use
- Taking certain antibiotics, such as tetracyclines
- Use of nail polishes
- Carotenoderma (from the excessive intake of orange vegetables)
- Yeast infections
- Psoriasis (autoimmune disease)
- Yellow nail syndrome
Green
- Adrenal gland diseases
- Yeast infections, such as Aspergillus
- Bacterial infections, such as pseudomonas
Brown
- Anthralin treatment (for psoriasis)
- Potassium permanganate (antiseptic and antioxidant drug)
- Peutz Jeghers disease (polyposis of the intestine)
What to do in the case of color changes in your child’s nails
First of all, you must sanitize your feet or hands well with soap and water, in order to rule out reversible causes such as dirt.
If the color changes in the nails persist, then you should consult your pediatrician. Regardless of the color or the extension along the nail, it’s important to assess the general condition of the child and look for other signs. In general, the doctor requests certain studies to determine and resolve the cause.
In the case of a specific nail disease, treatment can be localized or directed to this specific reason. For example, when the child has a fungal infection, an antifungal drug is prescribed for several weeks, as the tissue takes this long to regain its normal appearance.
When it comes to generalized diseases, changes in the color of the child’s nails are one more sign. So, the treatment is aimed at solving the basic problem and not at improving the appearance of these structures.
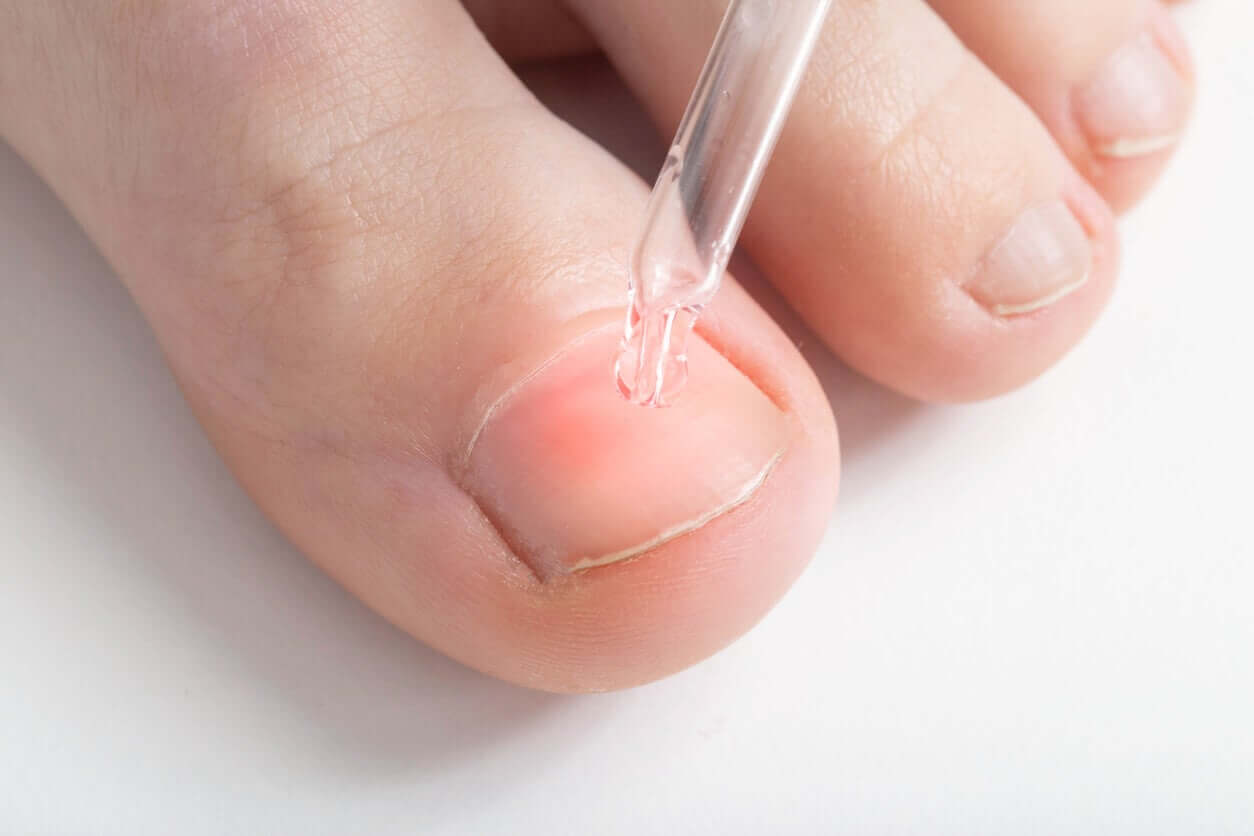
Can color changes in the nails of children be prevented?
In some cases yes, such as trauma or infection. Among the general skincare measures, the following stand out:
- Maintain proper hand and nail hygiene, even underneath
- Avoid cracks or injuries to the skin
- Drink enough water daily
- Moisturize the skin with moisturizing creams
- Avoid contact with irritating substances, such as solvents or alcohols
- Wear loose-fitting shoes and keep your feet ventilated
- Don’t walk barefoot in swimming pools and changing rooms
- Use only personal hygiene items and don’t share them
About color changes in children’s nails
Nails are part of our body and, like other areas of the skin, they can be warning signs of disease.
Sometimes we can prevent their damage through good hygiene and care practices but, other times, this isn’t possible. In this sense, timely consultation with your family doctor is essential in order to guide the diagnosis and carry out the appropriate treatments.
Nails protect the most outer tips of our bodies–our fingertips and toes. Their presence facilitates manual skills, improves the perception of touch, and fulfills an aesthetic function. Therefore, color changes in children’s nails can be a cause for great concern in parents.
In many cases, these modifications are due to trivial causes, while in others, they can alert us to the presence of more serious diseases.
Do you want to know why this color change occurs? Coming up next, we’ll tell you everything you need to know.
The normal development of children’s nails
The first traces of nails appear in the ninth week of gestation and, by week 20, all are fully formed. Growth continues throughout life and varies depending on the presence of certain factors, such as age, sex, nutrition, and disease.
Nails have several components, among which the following stand out:
- Nail plate: This is a rigid and translucent structure with a rectangular shape and a smooth surface and edges. It’s the most superficial and visible part.
- Nail bed: This is the layer that’s immediately under the plate. It’s pale pink in color, as blood vessels, nerves, and lymphatic vessels circulate through it.
- Nail matrix: This is a vital structure that manufactures the nail plate. It’s found under the skin and appears as a white crescent at the base of the nail (the lunula).
- Nail folds and cuticles: These are layers of skin that fold over on three edges of the plate in order to seal the nails and prevent germs from entering the matrix. They’re the same tone as the rest of the skin.
Pathological color changes in children’s nails

Any modification in the usual appearance of the nails warrants a consultation with a doctor.
Some of these changes can be present from birth and are part of some congenital diseases. But others can be acquired in later stages and indicate the presence of local illnesses (in the proximity of the nail) or at a distance.
Among the alterations in the appearance of the nails, are color changes. These range from small spots to a complete change from the usual hue.
Next, we’ll describe the illnesses that are associated with each color of children’s nails.
White
- Minor trauma
- Congenital candidiasis (yeast infection)
- Stevens-Johnson syndrome (acute and severe skin disease)
- Chemotherapy drugs (cancer drugs)
- Acrodermatitis enteropathica (innate metabolic disease)
- Heart failure (heart pump failure)
- Vitiligo (absence of skin pigments)
- Taking certain antibiotics, such as sulfonamides
- Noonan syndrome (genetic disease)
- Severe anemia
- Low levels of protein in the blood
Black
- Melanocytic nevus (moles)
- Melanoma (skin tumor)
- Taking certain drugs, such as cyclophosphamide (immunosuppressant)
- Severe trauma (for example, being slammed in a door)
- Paronychia (infections in nail folds)
Red
- Vascular tumors
- Paronychia or infections
- Petechiae dot-like skin bleeds)
- Autoimmune diseases such as lupus or rheumatoid arthritis
- Porphyrias (blood disease)
- Lichen planus (inflammatory skin disease)
- Bruising or bleeding below the nail bed
Blue or gray
- Ink stains
- The use of nail polish
- Cyanide, carbon monoxide, silver, or copper poisoning
- The use of some antibiotics, such as minocycline
- Chemotherapeutic agents
- A low level of oxygen in the blood, as occurs in severe respiratory distress
Yellow
- Tobacco use
- Taking certain antibiotics, such as tetracyclines
- Use of nail polishes
- Carotenoderma (from the excessive intake of orange vegetables)
- Yeast infections
- Psoriasis (autoimmune disease)
- Yellow nail syndrome
Green
- Adrenal gland diseases
- Yeast infections, such as Aspergillus
- Bacterial infections, such as pseudomonas
Brown
- Anthralin treatment (for psoriasis)
- Potassium permanganate (antiseptic and antioxidant drug)
- Peutz Jeghers disease (polyposis of the intestine)
What to do in the case of color changes in your child’s nails
First of all, you must sanitize your feet or hands well with soap and water, in order to rule out reversible causes such as dirt.
If the color changes in the nails persist, then you should consult your pediatrician. Regardless of the color or the extension along the nail, it’s important to assess the general condition of the child and look for other signs. In general, the doctor requests certain studies to determine and resolve the cause.
In the case of a specific nail disease, treatment can be localized or directed to this specific reason. For example, when the child has a fungal infection, an antifungal drug is prescribed for several weeks, as the tissue takes this long to regain its normal appearance.
When it comes to generalized diseases, changes in the color of the child’s nails are one more sign. So, the treatment is aimed at solving the basic problem and not at improving the appearance of these structures.

Can color changes in the nails of children be prevented?
In some cases yes, such as trauma or infection. Among the general skincare measures, the following stand out:
- Maintain proper hand and nail hygiene, even underneath
- Avoid cracks or injuries to the skin
- Drink enough water daily
- Moisturize the skin with moisturizing creams
- Avoid contact with irritating substances, such as solvents or alcohols
- Wear loose-fitting shoes and keep your feet ventilated
- Don’t walk barefoot in swimming pools and changing rooms
- Use only personal hygiene items and don’t share them
About color changes in children’s nails
Nails are part of our body and, like other areas of the skin, they can be warning signs of disease.
Sometimes we can prevent their damage through good hygiene and care practices but, other times, this isn’t possible. In this sense, timely consultation with your family doctor is essential in order to guide the diagnosis and carry out the appropriate treatments.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Correa N. Patologia de la Uña. Capítulo 9.2. En: Larralde M et al. Dermatología Pediátrica. Tercera Edición. Editorial Journal. Buenos Aires. Año 2021.
- Gioseffi A. Dermatosis de las uñas. Sección 17. En: Gioseffi A. Dermatología en Pediatría Ambulatoria. Editorial Panamericana. Buenos Aires. Año 2017.
- Zornosa Moreno M, Pertusa Guillén M. Cambios de color en las uñas, ¿me preocupo o no?. Familia y Salud, Asociación Española de Pediatría. Año 2015. Disponible en: https://www.familiaysalud.es/sintomas-y-enfermedades/la-piel/otros-problemas-de-piel/cambios-de-color-en-las-unas-me-preocupo-o. Downleaded May 2021.
- Larrañaga A, Capafons S, Vilá M. Todo sobre las uñas. Academia Española de Dermatología y Venerología. Año 2013. Disponible en: https://aedv.es/comunicacion/notas-de-prensa/todo-sobre-las-unas/. Downloaded May 2021.
- Amerian Academy of Dermatology Association. 12 Nail changes a Dermatologist should examine. Disponible en: https://www.aad.org/public/everyday-care/nail-care-secrets/basics/nail-changes-dermatologist-should-examine. Downloaded May 2021.
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








