Milia in Babies: What You Should Know

Written and verified by the dermatologist Maria del Carmen Hernandez
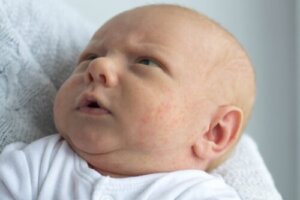
Milia in babies, also known as milk spots, are a fairly common dermatologic condition. Although they’re benign and resolve on their own, it’s best to be aware of their manifestations in order to know how to identify them. Here’s everything you need to know to manage them correctly.
What are milia in babies?
Milia are benign, temporary cysts of the dermis, composed of keratin, which appear as tiny, firm, white papules located on the face, genital area, extremities, and upper trunk. Keratin, on the other hand, is a protein which, in most cases, is found in the tissues of the hair, skin, and nails. It can therefore occur in people of all ages and ethnicities. However, they’re most common in newborns.
Milia classification
The classification of milia can be primary and secondary. In most cases, primary milia account for those that occur spontaneously and are present at birth, especially on the nose, eyelids, scalp, and cheeks.
Primary congenital milia occur in up to 40% to 50% of healthy term newborns. However, when secondary milia are acquired, they usually affect older children with a history of blistering skin conditions or trauma.
In general, primary milia develop from the lower infundibular sebaceous collar of the vellus hair follicles; whereas secondary milia arise from the eccrine ducts, sebaceous ducts, or epidermis.
You may be interested in: Miliaria or Sweat Rash in Infants: What Is It?
Causes of milia in infants
The etiology of milia in newborns differs significantly from that of adults or older children. Consequently, the cause in newborns isn’t known, although it’s often confused with infant acne that’s caused by maternal hormones. Unlike in infants, in older children and adults, it’s related to certain skin conditions, which may include the following:
- Burns
- Blisters (epidermolysis bullosa, cicatricial pemphigoid, or porphyria cutanea tarda)
- Prolonged use of corticosteroid creams
Milia may even develop when the epidermis loses its natural ability to exfoliate, which happens due to aging.
Clinical manifestations
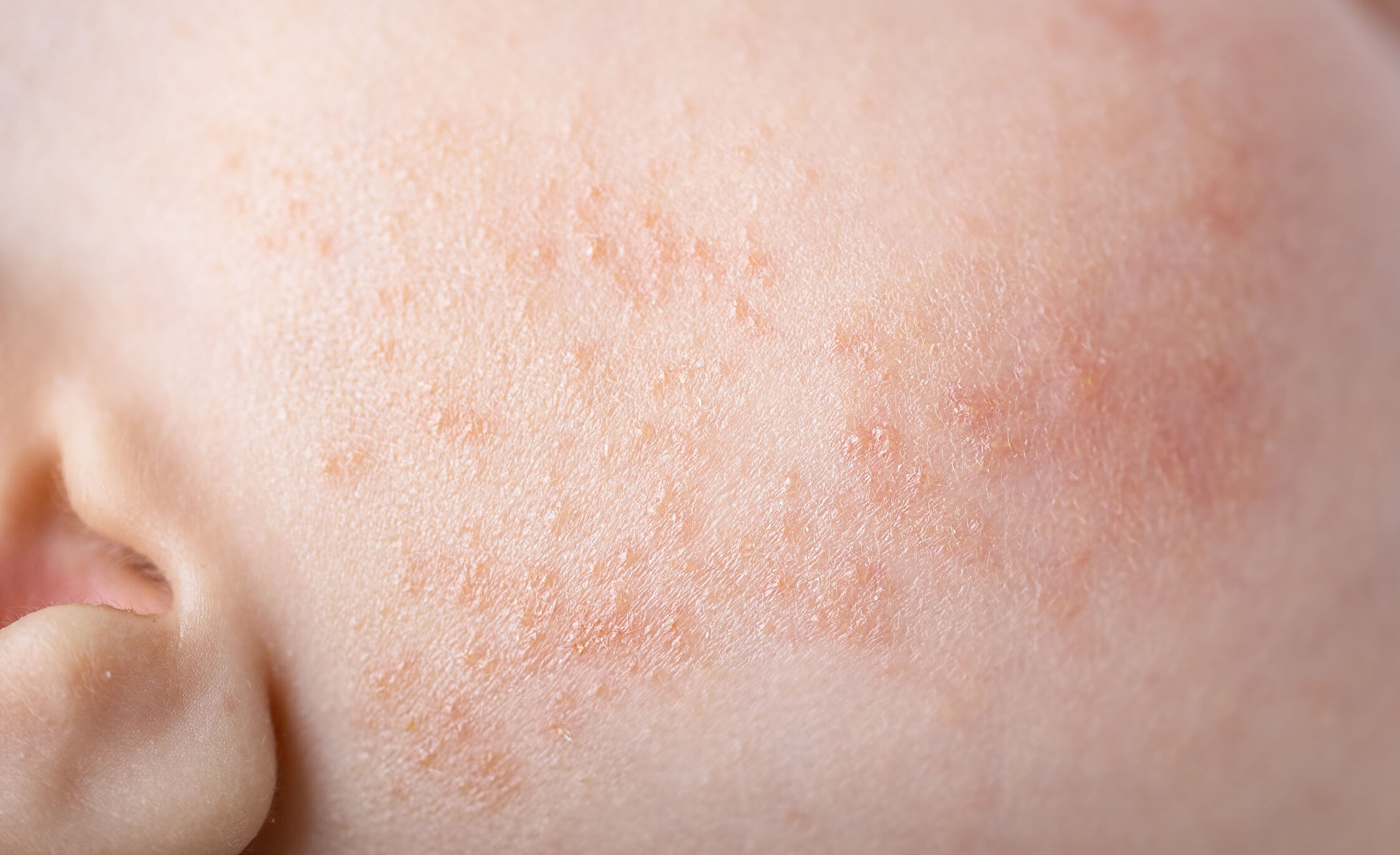
Milia lesions in infants are usually asymptomatic and resolve spontaneously within the first few months of life. In addition, they appear in the form of small yellow or white papules, measuring less than 3 millimeters, on the nose.
They may present in the form of plaque as a reddened area covered by multiple milia cysts. They’re usually not itchy or painful, but rough clothing or bed sheets may cause the skin to appear red and irritated. For this very reason, it’s often incorrectly referred to as “infant acne.”
Types of milia presentations
The types of milia can be divided according to the age at presentation or what causes the cysts. Namely:
- Neonatal milia: These are considered primary milia that develop in newborns and disappear in a few weeks. In turn, they occur most frequently on the scalp, face, and upper torso.
- Milia juvenile may be caused by some rare genetic disorders involving the skin. For example, nevoid basal cell carcinoma syndrome, Gardner syndrome, pachyonychia congenita, and Bazex-Dupré-Christol syndrome.
- Multiple eruptive milia: Appears in the form of itchy areas on the face, torso, or upper arms.
Read also: What Are Those Little Red Spots on My Baby’s Skin?

The management of milia in infants
Milia in infants are diagnosed on the basis of the clinical manifestations of the lesions. Moreover, they don’t require incision and drainage of the keratin content to certify the diagnosis. Therefore, no specific treatment is needed, as the papules tend to go away on their own. However, secondary milia may not heal spontaneously and, in this case, the contents will need to be removed.
Some of the therapeutic options that may be effective in secondary cases include the following:
- Cryotherapy is one of the most commonly used methods. In it, liquid nitrogen freezes the lesion.
- Topical retinoids: Contain vitamin A, which helps to exfoliate the skin surface.
- Chemical peeling: Acids peel off the first layer of skin.
- Manual removal: The contents of the milia cyst are removed with a sterile needle.
Milia in babies and their evolution
Milia in infants resolve spontaneously, without scarring or injury, over the course of weeks. Although the resolution process takes longer in older children or adults, this condition isn’t considered harmful. However, whenever the condition doesn’t improve or resolve, a doctor should be consulted to verify that it’s not another dermatological condition.
Milia in babies, also known as milk spots, are a fairly common dermatologic condition. Although they’re benign and resolve on their own, it’s best to be aware of their manifestations in order to know how to identify them. Here’s everything you need to know to manage them correctly.
What are milia in babies?
Milia are benign, temporary cysts of the dermis, composed of keratin, which appear as tiny, firm, white papules located on the face, genital area, extremities, and upper trunk. Keratin, on the other hand, is a protein which, in most cases, is found in the tissues of the hair, skin, and nails. It can therefore occur in people of all ages and ethnicities. However, they’re most common in newborns.
Milia classification
The classification of milia can be primary and secondary. In most cases, primary milia account for those that occur spontaneously and are present at birth, especially on the nose, eyelids, scalp, and cheeks.
Primary congenital milia occur in up to 40% to 50% of healthy term newborns. However, when secondary milia are acquired, they usually affect older children with a history of blistering skin conditions or trauma.
In general, primary milia develop from the lower infundibular sebaceous collar of the vellus hair follicles; whereas secondary milia arise from the eccrine ducts, sebaceous ducts, or epidermis.
You may be interested in: Miliaria or Sweat Rash in Infants: What Is It?

Causes of milia in infants
The etiology of milia in newborns differs significantly from that of adults or older children. Consequently, the cause in newborns isn’t known, although it’s often confused with infant acne that’s caused by maternal hormones. Unlike in infants, in older children and adults, it’s related to certain skin conditions, which may include the following:
- Burns
- Blisters (epidermolysis bullosa, cicatricial pemphigoid, or porphyria cutanea tarda)
- Prolonged use of corticosteroid creams
Milia may even develop when the epidermis loses its natural ability to exfoliate, which happens due to aging.
Clinical manifestations
Milia lesions in infants are usually asymptomatic and resolve spontaneously within the first few months of life. In addition, they appear in the form of small yellow or white papules, measuring less than 3 millimeters, on the nose.
They may present in the form of plaque as a reddened area covered by multiple milia cysts. They’re usually not itchy or painful, but rough clothing or bed sheets may cause the skin to appear red and irritated. For this very reason, it’s often incorrectly referred to as “infant acne.”
Types of milia presentations
The types of milia can be divided according to the age at presentation or what causes the cysts. Namely:
- Neonatal milia: These are considered primary milia that develop in newborns and disappear in a few weeks. In turn, they occur most frequently on the scalp, face, and upper torso.
- Milia juvenile may be caused by some rare genetic disorders involving the skin. For example, nevoid basal cell carcinoma syndrome, Gardner syndrome, pachyonychia congenita, and Bazex-Dupré-Christol syndrome.
- Multiple eruptive milia: Appears in the form of itchy areas on the face, torso, or upper arms.
Read also: What Are Those Little Red Spots on My Baby’s Skin?

The management of milia in infants
Milia in infants are diagnosed on the basis of the clinical manifestations of the lesions. Moreover, they don’t require incision and drainage of the keratin content to certify the diagnosis. Therefore, no specific treatment is needed, as the papules tend to go away on their own. However, secondary milia may not heal spontaneously and, in this case, the contents will need to be removed.
Some of the therapeutic options that may be effective in secondary cases include the following:
- Cryotherapy is one of the most commonly used methods. In it, liquid nitrogen freezes the lesion.
- Topical retinoids: Contain vitamin A, which helps to exfoliate the skin surface.
- Chemical peeling: Acids peel off the first layer of skin.
- Manual removal: The contents of the milia cyst are removed with a sterile needle.
Milia in babies and their evolution
Milia in infants resolve spontaneously, without scarring or injury, over the course of weeks. Although the resolution process takes longer in older children or adults, this condition isn’t considered harmful. However, whenever the condition doesn’t improve or resolve, a doctor should be consulted to verify that it’s not another dermatological condition.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Kutlubay Z, Tanakol A, Engýn B, Onel C, Sýmsek E, Serdaroglu S, Tuzun Y, Yilmaz E, Eren B. Newborn Skin: Common Skin Problems. Maedica (Bucur). 2017 Jan;12(1):42-47. PMID: 28878836; PMCID: PMC5574071.
- Batra P, Tsou HC, Warycha M, Votava HJ, Stein J. Multiple eruptive milia. Dermatol Online J. 2009 Aug 15;15(8):20. PMID: 19891928.
- Kansal NK, Agarwal S. Neonatal milia. Indian Pediatr. 2015 Aug;52(8):723-4. PMID: 26388648.
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








