Achondroplasia in Children: Causes and Characteristics

Achondroplasia in children is one of the most commonly seen forms of dwarfism. In every 25,000 children born, one has this genetic bone condition.
According to studies, we know that 75% of cases of achondroplasia in children are due to new genetic mutations during fetal development, while the other 25% are related to inherited genes. This genetic mutation is responsible for 70% of cases of dwarfism.
Achondroplasia in children is classified as a form of disproportionate dwarfism. The condition affects the development of the long bones while the development of the spine is normal. This leads to disproportionate growth.
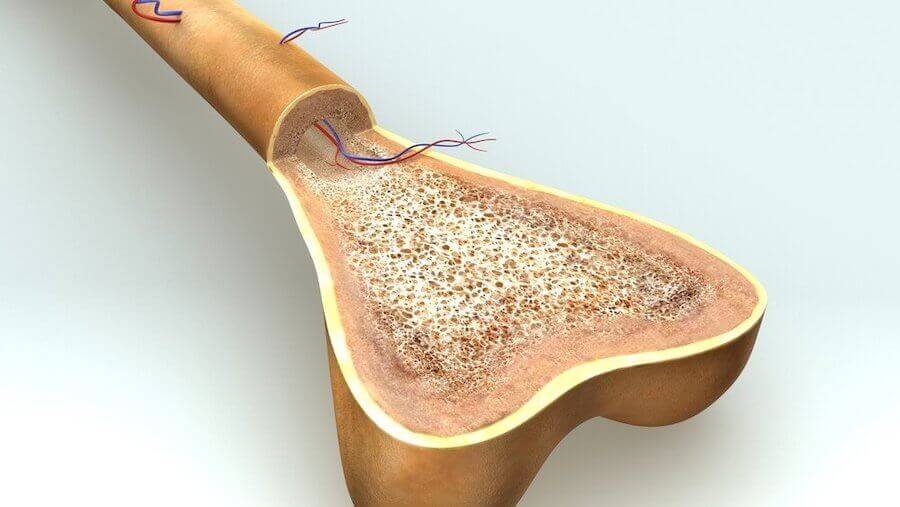
Achondroplasia in children occurs due to an alteration in cellular DNA. The change affects receptors of growth factor 3 which are present in fibroblasts. This leads to an anomaly in cartilage formation and later blocks normal bone growth.
There is an increased risk of death during childhood because compression of the medulla and respiratory system obstruction can occur.
Probability of Achondroplasia
The probability that a child whose parents don’t have the condition will have achondroplasia is 1/25,000. That rate rises to 50% if one parent has the condition, and 75% if both parents do.
Additionally, there is a 2.5% probability that a child will have homozygous achondroplasia if both parents have the condition.
Signs of Achondroplasia in Children
Signs of achondroplasia can be evaluated based on a diagnosis during fetal development. It can be inferred from bone measurements, but after birth it can be diagnosed with certainty.
Treatment for Achondroplasia in Children
There is no pharmacological treatment for achondroplasia. Despite this fact, they’ve been able to identify the gene that acts as a carrier on chromosome 4.P and 16.3, known as the short branch of chromosome 4.
Intellectual Capacity and Physical Characteristics
Children with achondroplasia have normal intellectual capacity. However, the physical characteristics are readily identifiable. The average adult height for a person with this condition is 47.2 inches, or 1.20 meters.
The long bones such as the femur and humerus are shorter compared to the forearm (radius and ulna) and the lower leg. The head is larger compared to body size, with a large forehead and flattened nasal septum. Some people have bone curvature, which can be very painful.
In some cases there are dental problems, involving crowded or twisted teeth. In general, feet can be wider, with narrow toes and flat soles. Muscle tone is weak, leading babies to develop more slowly at first.
They may also have what is known as trident hand, in which the space between the middle and ring finger is larger.

Associated Disorders
In addition to the physical characteristics, children with achondroplasia can present certain associated illnesses as they develop. But as long as these are monitored, a child can lead a normal life and develop to adulthood.
- Apnea: when babies stop breathing for a few seconds.
- Otitis: children with achondroplasia often suffer repeated ear infections, which can lead to greater harm if not treated.
- Spinal cord compression: this is a condition that occurs when the channel connecting the skull to the spinal column is very small, compressing the spinal cord and causing breathing problems.
- Hydrocephalus: when liquid accumulates in the baby’s skull it may result in a rapid abnormal growth of the head. Head size should be closely monitored.
- Kyphosis: this is a small hump that forms in the upper part of the back. In general it appears before the child begins walking, and later disappears.
- Spinal Curvature: inward curvature at the lower part of the back. This often appears after the child starts walking. It can be treated with special exercises.
Achondroplasia in children is one of the most commonly seen forms of dwarfism. In every 25,000 children born, one has this genetic bone condition.
According to studies, we know that 75% of cases of achondroplasia in children are due to new genetic mutations during fetal development, while the other 25% are related to inherited genes. This genetic mutation is responsible for 70% of cases of dwarfism.
Achondroplasia in children is classified as a form of disproportionate dwarfism. The condition affects the development of the long bones while the development of the spine is normal. This leads to disproportionate growth.

Achondroplasia in children occurs due to an alteration in cellular DNA. The change affects receptors of growth factor 3 which are present in fibroblasts. This leads to an anomaly in cartilage formation and later blocks normal bone growth.
There is an increased risk of death during childhood because compression of the medulla and respiratory system obstruction can occur.
Probability of Achondroplasia
The probability that a child whose parents don’t have the condition will have achondroplasia is 1/25,000. That rate rises to 50% if one parent has the condition, and 75% if both parents do.
Additionally, there is a 2.5% probability that a child will have homozygous achondroplasia if both parents have the condition.
Signs of Achondroplasia in Children
Signs of achondroplasia can be evaluated based on a diagnosis during fetal development. It can be inferred from bone measurements, but after birth it can be diagnosed with certainty.
Treatment for Achondroplasia in Children
There is no pharmacological treatment for achondroplasia. Despite this fact, they’ve been able to identify the gene that acts as a carrier on chromosome 4.P and 16.3, known as the short branch of chromosome 4.
Intellectual Capacity and Physical Characteristics
Children with achondroplasia have normal intellectual capacity. However, the physical characteristics are readily identifiable. The average adult height for a person with this condition is 47.2 inches, or 1.20 meters.
The long bones such as the femur and humerus are shorter compared to the forearm (radius and ulna) and the lower leg. The head is larger compared to body size, with a large forehead and flattened nasal septum. Some people have bone curvature, which can be very painful.
In some cases there are dental problems, involving crowded or twisted teeth. In general, feet can be wider, with narrow toes and flat soles. Muscle tone is weak, leading babies to develop more slowly at first.
They may also have what is known as trident hand, in which the space between the middle and ring finger is larger.

Associated Disorders
In addition to the physical characteristics, children with achondroplasia can present certain associated illnesses as they develop. But as long as these are monitored, a child can lead a normal life and develop to adulthood.
- Apnea: when babies stop breathing for a few seconds.
- Otitis: children with achondroplasia often suffer repeated ear infections, which can lead to greater harm if not treated.
- Spinal cord compression: this is a condition that occurs when the channel connecting the skull to the spinal column is very small, compressing the spinal cord and causing breathing problems.
- Hydrocephalus: when liquid accumulates in the baby’s skull it may result in a rapid abnormal growth of the head. Head size should be closely monitored.
- Kyphosis: this is a small hump that forms in the upper part of the back. In general it appears before the child begins walking, and later disappears.
- Spinal Curvature: inward curvature at the lower part of the back. This often appears after the child starts walking. It can be treated with special exercises.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Cialzeta domingo. (2009). Acondroplasia: una mirada desde la clínica pediátrica. Hospital Niños BAires.
- Fano V e Lejarraga H. (2000). Hallazgos frecuentes en la atención clínica de 96 ninõs con acondro- plasia. Arch Argent. Pediatr. 98(6). Pp. 368-375.
- Yolanda Sánchez Fernández, Isabel Ruiz Fernández, L. I. C. y M. L. P. R. (2009). LA IMPORTANCIA DE LA ATENCIÓN TEMPRANA EN NIÑOS CON ACONDROPLASIA; INTERVENCIÓN EN LA FAMILIA. International Journal of Developmental and Educational Psychology. https://www.redalyc.org/pdf/3498/349832331047.pdf
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








