Hypothyroidism in Children: What You Need to Know


Written and verified by the nurse Leidy Mora Molina
Hypothyroidism in children is a disease that results from an alteration at the level of the thyroid gland that generates a lower production of its respective hormones. These substances are essential for the correct functioning of the body and for metabolism.
In children, the cause of this disease can vary, as well as the impact on the development of their body. Therefore, early diagnosis and treatment can improve their prognosis.
Do you want to know more about hypothyroidism in children? Keep reading.
Hypothyroidism in children
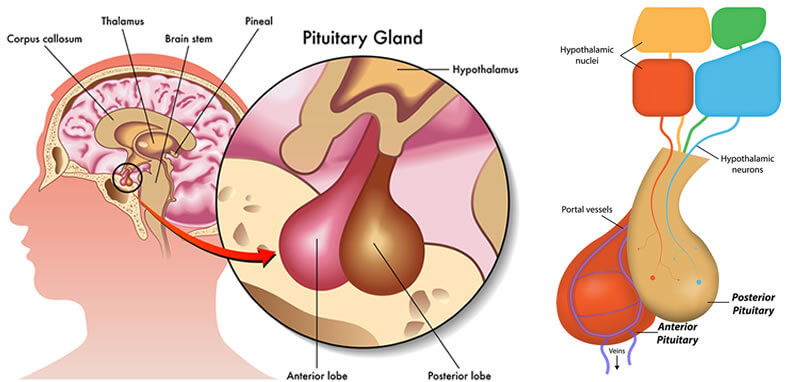
The thyroid gland is located in the middle of the neck and produces key hormones for health: Triiodothyronine (T3) and thyroxine (T4). This organ is controlled by the hypophysis or pituitary gland, located at the base of the brain, by means of thyroid stimulating hormone (TSH).
Thyroid hormones have very important functions for the organism, among which the following stand out:
- Promoting brain development
- Regulating metabolism
- Ensuring body growth
- Contributing to the maintenance of the internal temperature
When we talk about hypothyroidism, we’re referring to a condition that results from a decrease in the biological activity of thyroid hormones on body tissues. And this can be produced by a low production by the gland or by a high resistance to the hormonal action by the cells of the rest of the body.
In children, most cases of hypothyroidism occur due to a low production of thyroid hormones and it manifests itself from the early stages of life. Therefore, it can cause brain alterations, problems in body growth as well as in the development of different organs.
This condition is quite frequent in childhood and its prevalence varies according to the geographical area (1 in every 800 to 10,000 children).
In some cases, hypothyroidism is transitory, but in others, it becomes a chronic and incurable condition. But fortunately, with proper hormone replacement therapy and regular follow-up with a pediatric endocrinologist, affected children can lead a normal life.

Types of hypothyroidism in children
There are different criteria for classifying the disease, either based on the location of the problem or the cause of the problem.
Regarding the first criterion, the objective is to define which is the affected organ that produces a low level of thyroid hormones in the blood. The most common hypothyroidism in childhood is the primary type, which implies a malfunction of the thyroid gland. Secondary hypothyroidism refers to a malfunction of the pituitary gland.
Depending on the cause of the damage to the thyroid gland, hypothyroidism is classified into two types: Congenital (birth) or acquired (postnatal). Let’s look at each of them in detail.
Congenital hypothyroidism
When we talk about congenital hypothyroidism, we mean that the baby is born with a problem in its thyroid gland, either an abnormal development or a complete absence of the thyroid gland. Although more rarely, it can occur due to damage to the pituitary gland, it’s very rarely associated with the mother’s dietary habits (e.g. intake of iodine-deficient diets).
It’s estimated that this type of disease occurs in 1 in 3000 – 3500 births and constitutes one of the main preventable causes of intellectual disability.
Acquired hypothyroidism
If the disease appears after birth (more specifically, after 6 months of age), we speak of acquired hypothyroidism. In this case, the thyroid gland produces little or no thyroid hormone and the causes of this phenomenon are diverse:
- Hashimoto’s thyroiditis: This is an autoimmune disease, where the immune system itself attacks the thyroid gland and prevents it from performing its functions. It’s the main cause of hypothyroidism in children and women.
- Viral infections.
- Alterations caused by medication (due to lithium, amiodarone, and oxcarbazepine consumption).
- Family history of hypothyroidism.
- Surgical removal of the thyroid gland for other causes.
- Inadequate iodine intake, either more or less.
- Diseases of the pituitary gland (such as panhypopituitarism).
What are the symptoms of hypothyroidism in children?
Children usually present variable clinical pictures, both in terms of symptoms and intensity. In general, the disease has a slow onset, meaning that it may take several years to manifest itself and many signs may go unnoticed. Among the most prominent signs of hypothyroidism in children are described as follows:
- Chronic fatigue and tiredness.
- Increased sensitivity to cold.
- Weight gain. Hypothyroidism slows metabolism, resulting in moderate weight gain, between 4.5 and 10 pounds.
- Poor height gain. This is a characteristic sign of hypothyroidism in children.
- Delayed puberty (in adolescents).
- Dry and fragile skin and hair.
- Constipation.
- Goiter.
Infants with hypothyroidism may also have symptoms such as jaundice, a hoarse cry, a large and prominent tongue, respiratory distress, and umbilical hernia.
If you detect that your child has several of these symptoms, you need to discuss it with your pediatrician so they can order studies to confirm or rule out this diagnosis.
The diagnosis of hypothyroidism
The diagnosis of hypothyroidism in children is simple. First, your pediatrician will conduct a detailed physical examination, where height and weight are assessed to determine any alteration in the percentiles. In addition, they’ll palpate the thyroid to see if it is enlarged.
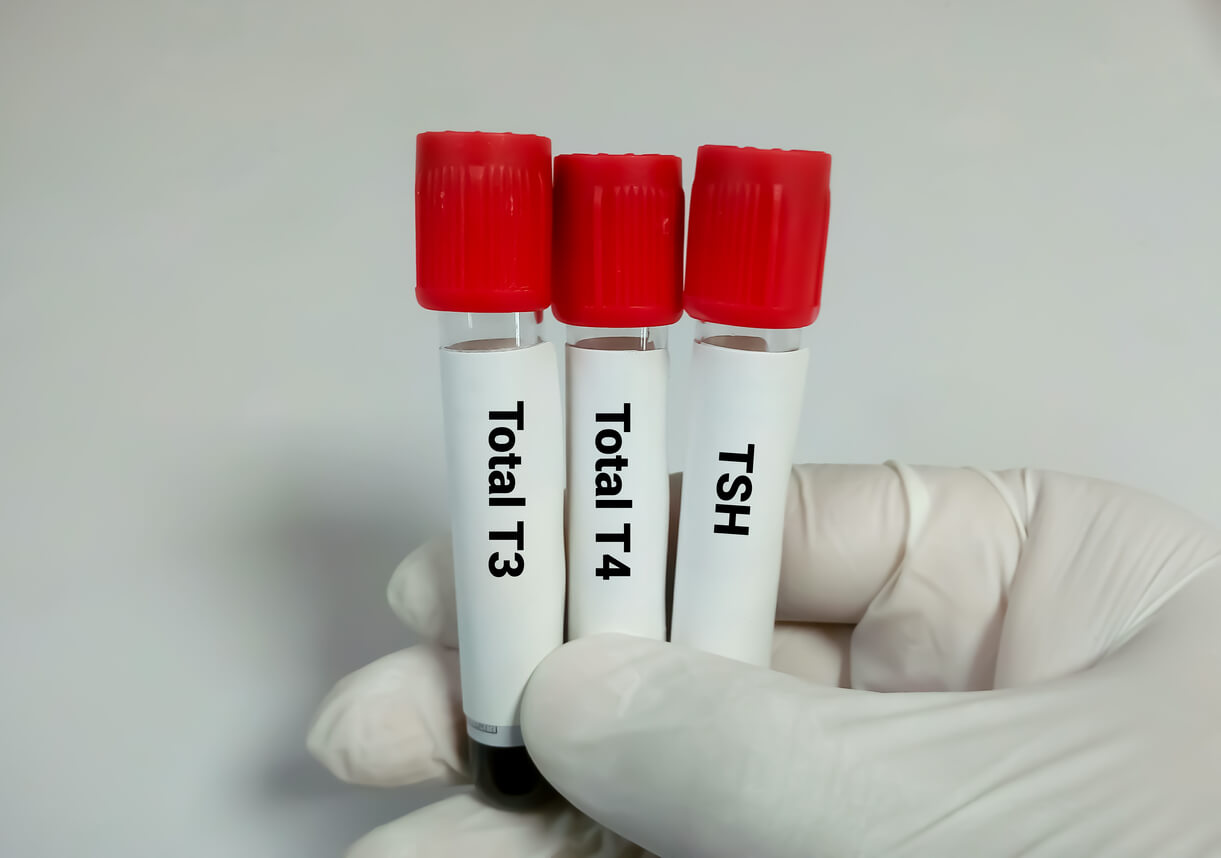
Then, they’ll order some blood tests to assess the levels of hormones produced by the pituitary and thyroid glands:
- Free T4: Free thyroxine levels are measured in blood, which is thyroxine that is not bound to proteins and can enter body tissues.
- TSH (thyroid stimulating hormone): This is a sensitive test to detect hypothyroidism. When the thyroid gland isn’t doing its job, the pituitary gland produces more TSH than usual to try to stimulate it.
- Antithyroid antibodies: This measurement is used to diagnose possible Hashimoto’s thyroiditis.
Hypothyroidism is diagnosed when TSH levels are high and the level of free T4 produced by the thyroid is low.
If the alteration of the blood tests is confirmed, other complementary tests will be ordered, such as a thyroid scan or thyroid ultrasound in order to determine the exact location of the gland and its size.
In addition, the endocrinologist is likely to request a brain MRI, to evaluate the pituitary gland and rule out central alterations.
Treatment of hypothyroidism in children
The treatment of hypothyroidism in children is based on hormone replacement through the administration of synthetic thyroid hormones, such as levothyroxine sodium or LT4.
This drug is administered once a day and the dose varies according to the age and weight of the child. Ideally, it should be administered after waking up and 30 minutes before eating. In addition, it should be taken away from other supplements, such as calcium, iron, or vitamins, to avoid diminishing its effect.
It should be noted that it’s vitally important to be consistent with the daily administration of this hormone to the child.
Often, the specialist also indicates biotin (vitamin B8) to improve the health of the child’s skin and hair. In addition, it’s important that the child has an adequate diet to avoid excessive weight gain.
This treatment has very few side effects, and if any occur, the dosage of the medication can be regulated. For this reason, a constant review by the endocrinologist is necessary.
Although there’s no cure for hypothyroidism in children, this hormonal treatment can control the symptoms and slow down the evolution of the disease. Therefore, it’s possible to lead a normal and otherwise healthy life.
The prevention of hypothyroidism in children
There’s no certain way to prevent hypothyroidism in children, but it’s important to detect it early when the child begins to show any suggestive symptoms. Therefore, treatment can be initiated before negative and irreversible consequences to their health are unleashed.
Hypothyroidism in children is a disease that results from an alteration at the level of the thyroid gland that generates a lower production of its respective hormones. These substances are essential for the correct functioning of the body and for metabolism.
In children, the cause of this disease can vary, as well as the impact on the development of their body. Therefore, early diagnosis and treatment can improve their prognosis.
Do you want to know more about hypothyroidism in children? Keep reading.
Hypothyroidism in children
The thyroid gland is located in the middle of the neck and produces key hormones for health: Triiodothyronine (T3) and thyroxine (T4). This organ is controlled by the hypophysis or pituitary gland, located at the base of the brain, by means of thyroid stimulating hormone (TSH).
Thyroid hormones have very important functions for the organism, among which the following stand out:
- Promoting brain development
- Regulating metabolism
- Ensuring body growth
- Contributing to the maintenance of the internal temperature
When we talk about hypothyroidism, we’re referring to a condition that results from a decrease in the biological activity of thyroid hormones on body tissues. And this can be produced by a low production by the gland or by a high resistance to the hormonal action by the cells of the rest of the body.
In children, most cases of hypothyroidism occur due to a low production of thyroid hormones and it manifests itself from the early stages of life. Therefore, it can cause brain alterations, problems in body growth as well as in the development of different organs.
This condition is quite frequent in childhood and its prevalence varies according to the geographical area (1 in every 800 to 10,000 children).
In some cases, hypothyroidism is transitory, but in others, it becomes a chronic and incurable condition. But fortunately, with proper hormone replacement therapy and regular follow-up with a pediatric endocrinologist, affected children can lead a normal life.

Types of hypothyroidism in children
There are different criteria for classifying the disease, either based on the location of the problem or the cause of the problem.
Regarding the first criterion, the objective is to define which is the affected organ that produces a low level of thyroid hormones in the blood. The most common hypothyroidism in childhood is the primary type, which implies a malfunction of the thyroid gland. Secondary hypothyroidism refers to a malfunction of the pituitary gland.
Depending on the cause of the damage to the thyroid gland, hypothyroidism is classified into two types: Congenital (birth) or acquired (postnatal). Let’s look at each of them in detail.
Congenital hypothyroidism
When we talk about congenital hypothyroidism, we mean that the baby is born with a problem in its thyroid gland, either an abnormal development or a complete absence of the thyroid gland. Although more rarely, it can occur due to damage to the pituitary gland, it’s very rarely associated with the mother’s dietary habits (e.g. intake of iodine-deficient diets).
It’s estimated that this type of disease occurs in 1 in 3000 – 3500 births and constitutes one of the main preventable causes of intellectual disability.
Acquired hypothyroidism
If the disease appears after birth (more specifically, after 6 months of age), we speak of acquired hypothyroidism. In this case, the thyroid gland produces little or no thyroid hormone and the causes of this phenomenon are diverse:
- Hashimoto’s thyroiditis: This is an autoimmune disease, where the immune system itself attacks the thyroid gland and prevents it from performing its functions. It’s the main cause of hypothyroidism in children and women.
- Viral infections.
- Alterations caused by medication (due to lithium, amiodarone, and oxcarbazepine consumption).
- Family history of hypothyroidism.
- Surgical removal of the thyroid gland for other causes.
- Inadequate iodine intake, either more or less.
- Diseases of the pituitary gland (such as panhypopituitarism).

What are the symptoms of hypothyroidism in children?
Children usually present variable clinical pictures, both in terms of symptoms and intensity. In general, the disease has a slow onset, meaning that it may take several years to manifest itself and many signs may go unnoticed. Among the most prominent signs of hypothyroidism in children are described as follows:
- Chronic fatigue and tiredness.
- Increased sensitivity to cold.
- Weight gain. Hypothyroidism slows metabolism, resulting in moderate weight gain, between 4.5 and 10 pounds.
- Poor height gain. This is a characteristic sign of hypothyroidism in children.
- Delayed puberty (in adolescents).
- Dry and fragile skin and hair.
- Constipation.
- Goiter.
Infants with hypothyroidism may also have symptoms such as jaundice, a hoarse cry, a large and prominent tongue, respiratory distress, and umbilical hernia.
If you detect that your child has several of these symptoms, you need to discuss it with your pediatrician so they can order studies to confirm or rule out this diagnosis.
The diagnosis of hypothyroidism
The diagnosis of hypothyroidism in children is simple. First, your pediatrician will conduct a detailed physical examination, where height and weight are assessed to determine any alteration in the percentiles. In addition, they’ll palpate the thyroid to see if it is enlarged.
Then, they’ll order some blood tests to assess the levels of hormones produced by the pituitary and thyroid glands:
- Free T4: Free thyroxine levels are measured in blood, which is thyroxine that is not bound to proteins and can enter body tissues.
- TSH (thyroid stimulating hormone): This is a sensitive test to detect hypothyroidism. When the thyroid gland isn’t doing its job, the pituitary gland produces more TSH than usual to try to stimulate it.
- Antithyroid antibodies: This measurement is used to diagnose possible Hashimoto’s thyroiditis.
Hypothyroidism is diagnosed when TSH levels are high and the level of free T4 produced by the thyroid is low.
If the alteration of the blood tests is confirmed, other complementary tests will be ordered, such as a thyroid scan or thyroid ultrasound in order to determine the exact location of the gland and its size.
In addition, the endocrinologist is likely to request a brain MRI, to evaluate the pituitary gland and rule out central alterations.

Treatment of hypothyroidism in children
The treatment of hypothyroidism in children is based on hormone replacement through the administration of synthetic thyroid hormones, such as levothyroxine sodium or LT4.
This drug is administered once a day and the dose varies according to the age and weight of the child. Ideally, it should be administered after waking up and 30 minutes before eating. In addition, it should be taken away from other supplements, such as calcium, iron, or vitamins, to avoid diminishing its effect.
It should be noted that it’s vitally important to be consistent with the daily administration of this hormone to the child.
Often, the specialist also indicates biotin (vitamin B8) to improve the health of the child’s skin and hair. In addition, it’s important that the child has an adequate diet to avoid excessive weight gain.
This treatment has very few side effects, and if any occur, the dosage of the medication can be regulated. For this reason, a constant review by the endocrinologist is necessary.
Although there’s no cure for hypothyroidism in children, this hormonal treatment can control the symptoms and slow down the evolution of the disease. Therefore, it’s possible to lead a normal and otherwise healthy life.
The prevention of hypothyroidism in children
There’s no certain way to prevent hypothyroidism in children, but it’s important to detect it early when the child begins to show any suggestive symptoms. Therefore, treatment can be initiated before negative and irreversible consequences to their health are unleashed.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- American thyroid association (2021). Hipotiroidismo en Niños y Adolescentes. Recuperado de: https://www.thyroid.org/hipotiroidismo-ninos-adolescentes/
- Ares, S. et al (2009). Enfermedades frecuentes del tiroides en la infancia. Revista Pediatría en Atención Primaria Vol.11 Supl.16. Recuperado de: https://scielo.isciii.es/scielo.php?script=sci_arttext&pid=S1139-76322009000600005
- Asociacion española de pediatria (2022). Levotiroxina sódica. Recuperado de: https://www.aeped.es/comite-medicamentos/pediamecum/levotiroxina-sodica
- Castilla, M (2015). Hipotiroidismo congénito. Boletín Médico del Hospital Infantil de México. Vol. 72 N°2. Recuperado de: https://www.elsevier.es/es-revista-boletin-medico-del-hospital-infantil-401-articulo-hipotiroidismo-congenito-S166511461500060X
- Manual Merck (2020). Hipotiroidismo en lactantes y niños. Recuperado de: https://www.merckmanuals.com/es-us/hogar/salud-infantil/trastornos-hormonales-en-ni%C3%B1os/hipotiroidismo-en-lactantes-y-ni%C3%B1os
- Sanz, M. et al (2015). Patología tiroidea en el niño y en el adolescente. Revista de pediatría Integral 2015; XIX (7): 467-476. Recuperado de: https://www.pediatriaintegral.es/publicacion-2015-09/patologia-tiroidea-en-el-nino-y-en-el-adolescente/
- Toro, M. et al. (2012). Hipotiroidismo adquirido en niños. Medicina y laboratorio. Vol 18, N° 9-10. Recuperado de: https://www.medigraphic.com/pdfs/medlab/myl-2012/myl129-10c.pdf
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








