How to Prevent and Treat Melasma During Pregnancy


Written and verified by the dermatologist Maria del Carmen Hernandez
Melasma is a very common condition in pregnant women. It generally affects women in their 20s and older and is characterized by the appearance of hyperpigmented spots on exposed areas of the skin, such as the face.
It’s caused by several factors that can be avoided to prevent this problem. Here, we’ll tell you more about it. Are you interested? Keep reading the article below!
Melasma during pregnancy: Dark spots on the face
Melasma is an acquired condition that develops during pregnancy. It’s characterized by the appearance of symmetrical spots on the face. Most women get it in the following areas:
- The chin
- The cheeks
- The forehead
- The bridge of the nose
- Above the upper lip
In addition, it’s more common in dark phototypes than in light phototypes; and it’s rare for it to occur before puberty and more frequent in the reproductive years.
Pregnant women have increased values of progesterone and estrogen hormones, so they’re believed to contribute to the development of hyperpigmentations.

Types of melasma
There are three types of melasma that are classified according to the depth of the pigment. In order to differentiate between them, a Wood’s lamp is used which emits black light and determines how deep the pigment is located.
- Epidermal: The coloration is darker, with a well-defined border. This type of melasma responds quite well to treatment.
- Dermal: Hyperpigmented spots have a light brown or bluish color and the border isn’t well-defined. It doesn’t respond well to the proposed treatments.
- Mixed melasma: This is the most frequently occurring variant in which patches of brown and blue coloration are observed. Response to depigmenting treatments is relative.
When does melasma during pregnancy start and how long does it last?
The causes of melasma can be multiple, including hormonal influences, exposure to sunlight, and family history. However, studies conducted by the Indian Journal of Dermatology have shown that ultraviolet light triggers and exacerbates the condition.
From the second trimester of pregnancy, when hormonal changes become more evident, hyperpigmented spots appear on the face.
For some women, melasma disappears on its own after childbirth or breastfeeding. In general, this occurs when it’s generated by pregnancy or birth control pills.
At the same time, procedures to eliminate it don’t guarantee that melasma won’t return. In fact, some cases can’t even be completely attenuated.
Can melasma during pregnancy be prevented or treated?
According to the American Academy of Dermatology Association, 90% of people who develop melasma are women. Although family history or hormonal alterations can’t be modified, there are some useful measures to put into practice and contribute to prevention.
Preventive methods
One of the most effective methods to prevent the exacerbation and outbreaks of melasma is to avoid ultraviolet rays and visible light.
It’s also recommended to use sunscreen every day with SPF 50 one hour before sun exposure and reapply it within two hours. The ideal filters are those composed of titanium or zinc minerals, as they’re not absorbed into the skin.
Even the choice of protective clothing is especially important if you’re exposed to the sun’s rays for a prolonged period of time. In fact, a wide-brimmed hat protects and shades the face.
Another essential recommendation to prevent the appearance of melasma in pregnancy is to avoid the middle hours of the day when ultraviolet rays are most damaging.
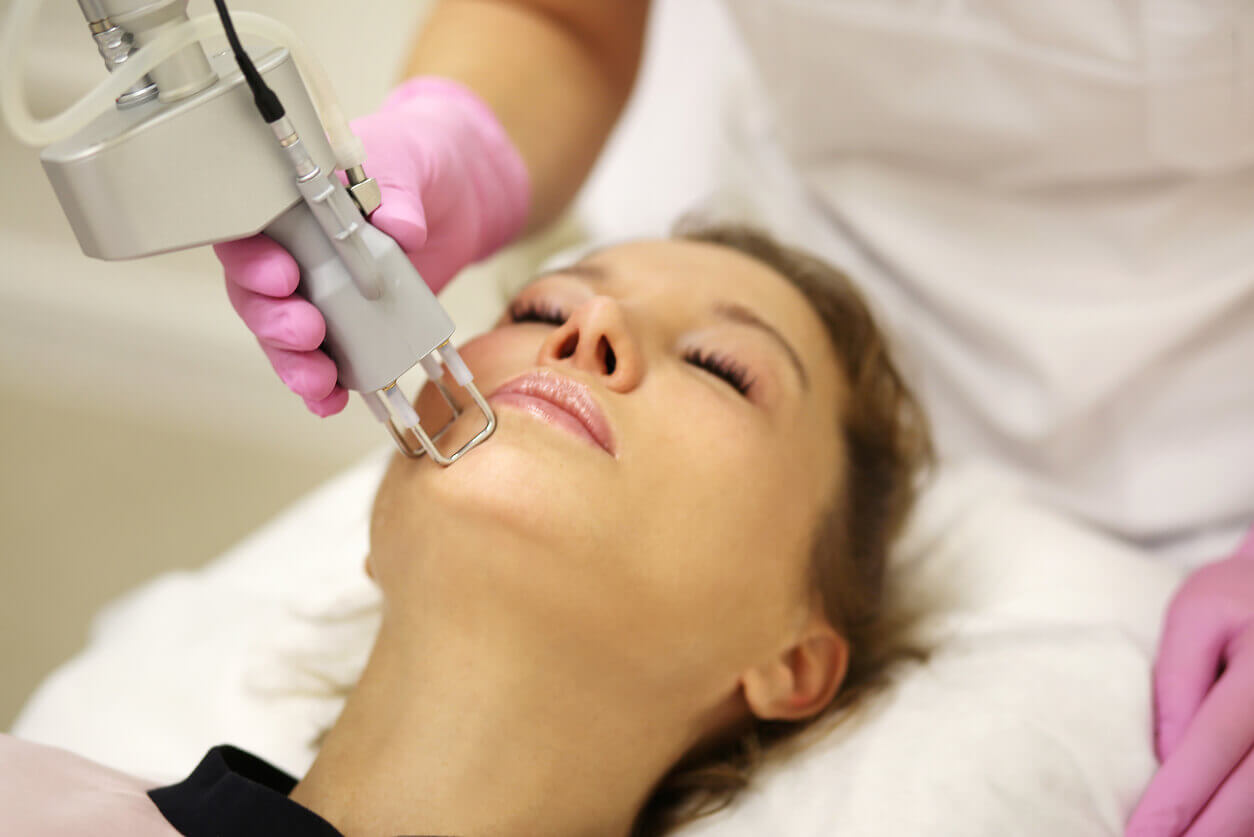
Therapeutic options
There are several topical, procedural, and oral therapies to manage melasma during pregnancy. Some of the topical options include hydroquinone, corticosteroids, and tretinoin. In turn, the addition of vitamin C serum to skincare routines helps fight free radical damage, brightens the skin, and improves skin tone.
While oral drugs such as tranexamic acid are quite promising in the treatment of blemishes.
Even, aesthetic procedures performed by qualified personnel can be the following: Microneedling, chemical peels, laser, and radiofrequency.
In conclusion, while there are several treatments that help improve the appearance of melasma, it’s a skin condition that can come and go at different times.
You may be interested in: Natural Cosmetics for Pregnant Women
Will melasma improve after delivery?
Melasma during pregnancy can also occur on the forearms and neck. Also, while it doesn’t cause any physical harm, it may cause embarrassment.
In some cases, spots on the face usually fade after delivery spontaneously without medical intervention. Otherwise, depigmenting therapies with creams, chemical peels, or appliances can be used.
Melasma during pregnancy isn’t just an aesthetic issue
Melasma developed during pregnancy is a frustrating condition to deal with and has major psychosocial implications.
However, there’s no associated mortality or morbidity. Moreover, fortunately, melasma in pregnant women resolves on its own in some cases.
Melasma is a very common condition in pregnant women. It generally affects women in their 20s and older and is characterized by the appearance of hyperpigmented spots on exposed areas of the skin, such as the face.
It’s caused by several factors that can be avoided to prevent this problem. Here, we’ll tell you more about it. Are you interested? Keep reading the article below!
Melasma during pregnancy: Dark spots on the face
Melasma is an acquired condition that develops during pregnancy. It’s characterized by the appearance of symmetrical spots on the face. Most women get it in the following areas:
- The chin
- The cheeks
- The forehead
- The bridge of the nose
- Above the upper lip
In addition, it’s more common in dark phototypes than in light phototypes; and it’s rare for it to occur before puberty and more frequent in the reproductive years.
Pregnant women have increased values of progesterone and estrogen hormones, so they’re believed to contribute to the development of hyperpigmentations.

Types of melasma
There are three types of melasma that are classified according to the depth of the pigment. In order to differentiate between them, a Wood’s lamp is used which emits black light and determines how deep the pigment is located.
- Epidermal: The coloration is darker, with a well-defined border. This type of melasma responds quite well to treatment.
- Dermal: Hyperpigmented spots have a light brown or bluish color and the border isn’t well-defined. It doesn’t respond well to the proposed treatments.
- Mixed melasma: This is the most frequently occurring variant in which patches of brown and blue coloration are observed. Response to depigmenting treatments is relative.
When does melasma during pregnancy start and how long does it last?
The causes of melasma can be multiple, including hormonal influences, exposure to sunlight, and family history. However, studies conducted by the Indian Journal of Dermatology have shown that ultraviolet light triggers and exacerbates the condition.
From the second trimester of pregnancy, when hormonal changes become more evident, hyperpigmented spots appear on the face.
For some women, melasma disappears on its own after childbirth or breastfeeding. In general, this occurs when it’s generated by pregnancy or birth control pills.
At the same time, procedures to eliminate it don’t guarantee that melasma won’t return. In fact, some cases can’t even be completely attenuated.
Can melasma during pregnancy be prevented or treated?
According to the American Academy of Dermatology Association, 90% of people who develop melasma are women. Although family history or hormonal alterations can’t be modified, there are some useful measures to put into practice and contribute to prevention.
Preventive methods
One of the most effective methods to prevent the exacerbation and outbreaks of melasma is to avoid ultraviolet rays and visible light.
It’s also recommended to use sunscreen every day with SPF 50 one hour before sun exposure and reapply it within two hours. The ideal filters are those composed of titanium or zinc minerals, as they’re not absorbed into the skin.
Even the choice of protective clothing is especially important if you’re exposed to the sun’s rays for a prolonged period of time. In fact, a wide-brimmed hat protects and shades the face.
Another essential recommendation to prevent the appearance of melasma in pregnancy is to avoid the middle hours of the day when ultraviolet rays are most damaging.

Therapeutic options
There are several topical, procedural, and oral therapies to manage melasma during pregnancy. Some of the topical options include hydroquinone, corticosteroids, and tretinoin. In turn, the addition of vitamin C serum to skincare routines helps fight free radical damage, brightens the skin, and improves skin tone.
While oral drugs such as tranexamic acid are quite promising in the treatment of blemishes.
Even, aesthetic procedures performed by qualified personnel can be the following: Microneedling, chemical peels, laser, and radiofrequency.
In conclusion, while there are several treatments that help improve the appearance of melasma, it’s a skin condition that can come and go at different times.
You may be interested in: Natural Cosmetics for Pregnant Women
Will melasma improve after delivery?
Melasma during pregnancy can also occur on the forearms and neck. Also, while it doesn’t cause any physical harm, it may cause embarrassment.
In some cases, spots on the face usually fade after delivery spontaneously without medical intervention. Otherwise, depigmenting therapies with creams, chemical peels, or appliances can be used.
Melasma during pregnancy isn’t just an aesthetic issue
Melasma developed during pregnancy is a frustrating condition to deal with and has major psychosocial implications.
However, there’s no associated mortality or morbidity. Moreover, fortunately, melasma in pregnant women resolves on its own in some cases.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Achar A, Rathi SK. Melasma: a clinico-epidemiological study of 312 cases. Indian J Dermatol. 2011 Jul;56(4):380-2. doi: 10.4103/0019-5154.84722. PMID: 21965843; PMCID: PMC3178998.
- Boukari F, Jourdan E, Fontas E, Montaudié H, Castela E, Lacour JP, Passeron T. Prevention of melasma relapses with sunscreen combining protection against UV and short wavelengths of visible light: a prospective randomized comparative trial. J Am Acad Dermatol. 2015 Jan;72(1):189-90.e1. doi: 10.1016/j.jaad.2014.08.023. Epub 2014 Oct 22. PMID: 25443629.
- Melasma: Diagnosis and Treatment. [Internet ] Disponible en: https://www.aad.org/public/diseases/a-z/melasma-treatment#causes
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








