Mouth Sores in Children: Causes and Treatment
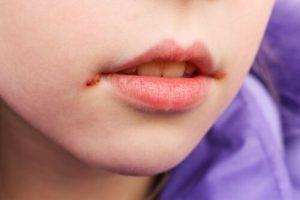
Mouth sores in children are very common. This infection is caused by a fungus or bacteria and causes pain and discomfort in children, especially when they open their mouths to eat. Because of this, you should treat them quickly to avoid unnecessary suffering.
How to know if your children have mouth sores
You’ll know if your children are suffering from mouth sores if you notice inflammation and redness at the corner of their lips, scabs or small fissures. There will be a noticeable smell when they open their mouths.
In babies, crying is always the first sign. In the case of older children, they’ll be able to express the pain they’re feeling, and explain what’s happening.
Mouth sores tend to be very painful and irritating, and children often rub them and get them wet. This, unfortunately, worsens the situation.
The causes of children’s mouth sores
We should first determine the causes of cheilitis, or mouth sores, in children. That way you’ll be able to give the correct treatment. The most frequent are:
Saliva
The accumulation of saliva in the lip area allows the spread of bacteria, especially streptococcus and staphylococcus. It can also produce a fungus known as candida. This fungus is contagious, and can easily be spread to other people by physical contact.
If the baby is teething then he or she will be prone to getting these mouth sores. This is due to the excessive salivation and constant drooling.
Vitamin deficiency
Some children have deficiencies of vitamins A, B and D, folic acid, iron and zinc or have anemic symptoms due to poor diet. Because of this, they too will be more susceptible to suffering from these types of mouth sores. Another common cause are allergic reactions to food or cosmetic products.
“If there is inflammation and redness in the corner of the lips, scabs or small fissures, then they’re suffering from angular cheilitis mouth sores”
Use of pacifiers
In the case of babies, the use of pacifiers and baby bottles can cause the accumulation of saliva in the corners of their mouths.

Other causes
- Use of teethers or sucking their thumbs/fingers
- Exposure to extreme temperatures, either very cold conditions, or exposure to the sun for long periods
- Use of dentures that don’t fit well
- Nervous disorders
- Dehydration
- Digestive problems
In addition to this, stress at school because of exams and other factors can also causes mouth sores. Other causes include viruses such as the flu, or fever.
How to treat angular cheilitis in children
The most important thing is to know what is causing the mouth sores in your child. Your doctor will prescribe the medication that your child will need, such as anti-inflammatories, antibiotics and bactericidal or fungicidal creams.
If the outbreak isn’t too serious then you can treat it at home with the following recommendations and home remedies.
- Follow a diet rich in vitamins and minerals.
- Keep the child well hydrated, especially with water.
- Keep a high level of hygiene at home.
- Dry the child’s mouth frequently with a clean, soft cloth.
- Apply the medicated creams.
- Avoid any food or product that causes allergies.
- Don’t give hot or very acidic foods.
- Prevent the child from kissing his siblings or other people, as mouth sores are contagious.
- Avoid touching or scratching the affected area if possible.

5 plant-based treatments to cure mouth sores
Some plant-based remedies can also be very effective. Keep in mind that this condition normally lasts around 6 or 7 days. If they persist, you should consult a specialist.
- Aloe Vera: Aloe Vera has moisturizing, antibacterial and healing properties. It’s a very effective healer. You should extract the gel from the Aloe Vera plant (or buy it directly from health shops). Rub the gel about 3 times a day directly onto the mouth sores.
- Parietaria: This can cure cheilitis naturally. Use a poultice made from the plant and apply it at night time.
- Rosehip oil: This is a magnificent moisturizer and healer. Apply a few drops 3 times a day. It’s advisable to use it when the mouth sores have just broken out.
- Honey: It must be natural honey to be effective. Honey is very effective in fighting the infection and is a good healer. Before bedtime apply a few drops of honey.
- Calendula flowers: These contain emollients, which are antiseptic and healing. Simply wash the affected area several times a day and apply creams made from this plant.
If your child has mouth sores, you shouldn’t be alarmed. With proper hygiene and the right treatment, they will soon heal and disappear.
Mouth sores in children are very common. This infection is caused by a fungus or bacteria and causes pain and discomfort in children, especially when they open their mouths to eat. Because of this, you should treat them quickly to avoid unnecessary suffering.
How to know if your children have mouth sores
You’ll know if your children are suffering from mouth sores if you notice inflammation and redness at the corner of their lips, scabs or small fissures. There will be a noticeable smell when they open their mouths.
In babies, crying is always the first sign. In the case of older children, they’ll be able to express the pain they’re feeling, and explain what’s happening.
Mouth sores tend to be very painful and irritating, and children often rub them and get them wet. This, unfortunately, worsens the situation.
The causes of children’s mouth sores
We should first determine the causes of cheilitis, or mouth sores, in children. That way you’ll be able to give the correct treatment. The most frequent are:
Saliva
The accumulation of saliva in the lip area allows the spread of bacteria, especially streptococcus and staphylococcus. It can also produce a fungus known as candida. This fungus is contagious, and can easily be spread to other people by physical contact.
If the baby is teething then he or she will be prone to getting these mouth sores. This is due to the excessive salivation and constant drooling.
Vitamin deficiency
Some children have deficiencies of vitamins A, B and D, folic acid, iron and zinc or have anemic symptoms due to poor diet. Because of this, they too will be more susceptible to suffering from these types of mouth sores. Another common cause are allergic reactions to food or cosmetic products.
“If there is inflammation and redness in the corner of the lips, scabs or small fissures, then they’re suffering from angular cheilitis mouth sores”
Use of pacifiers
In the case of babies, the use of pacifiers and baby bottles can cause the accumulation of saliva in the corners of their mouths.

Other causes
- Use of teethers or sucking their thumbs/fingers
- Exposure to extreme temperatures, either very cold conditions, or exposure to the sun for long periods
- Use of dentures that don’t fit well
- Nervous disorders
- Dehydration
- Digestive problems
In addition to this, stress at school because of exams and other factors can also causes mouth sores. Other causes include viruses such as the flu, or fever.
How to treat angular cheilitis in children
The most important thing is to know what is causing the mouth sores in your child. Your doctor will prescribe the medication that your child will need, such as anti-inflammatories, antibiotics and bactericidal or fungicidal creams.
If the outbreak isn’t too serious then you can treat it at home with the following recommendations and home remedies.
- Follow a diet rich in vitamins and minerals.
- Keep the child well hydrated, especially with water.
- Keep a high level of hygiene at home.
- Dry the child’s mouth frequently with a clean, soft cloth.
- Apply the medicated creams.
- Avoid any food or product that causes allergies.
- Don’t give hot or very acidic foods.
- Prevent the child from kissing his siblings or other people, as mouth sores are contagious.
- Avoid touching or scratching the affected area if possible.

5 plant-based treatments to cure mouth sores
Some plant-based remedies can also be very effective. Keep in mind that this condition normally lasts around 6 or 7 days. If they persist, you should consult a specialist.
- Aloe Vera: Aloe Vera has moisturizing, antibacterial and healing properties. It’s a very effective healer. You should extract the gel from the Aloe Vera plant (or buy it directly from health shops). Rub the gel about 3 times a day directly onto the mouth sores.
- Parietaria: This can cure cheilitis naturally. Use a poultice made from the plant and apply it at night time.
- Rosehip oil: This is a magnificent moisturizer and healer. Apply a few drops 3 times a day. It’s advisable to use it when the mouth sores have just broken out.
- Honey: It must be natural honey to be effective. Honey is very effective in fighting the infection and is a good healer. Before bedtime apply a few drops of honey.
- Calendula flowers: These contain emollients, which are antiseptic and healing. Simply wash the affected area several times a day and apply creams made from this plant.
If your child has mouth sores, you shouldn’t be alarmed. With proper hygiene and the right treatment, they will soon heal and disappear.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Akhtar, N., Zaman, S. U., Khan, B. A., Amir, M. N., & Ebrahimzadeh, M. A. (2011). Calendula extract: effects on mechanical parameters of human skin. Acta Poloniae Pharmaceutica, 68(5), 693–701. https://pubmed.ncbi.nlm.nih.gov/21928714/
- Bermúdez Bermúdez, M., Cuadro Montero, K. M., Parra Sanabria, E. A., Rueda Jiménez, A., & Peña Vega, C. P. (2021). Manifestaciones en la cavidad bucal y en la cara asociadas a la COVID-19. Universitas Médica, 62(3), 115–131. https://doi.org/10.11144/javeriana.umed62-3.mcbc
- Cazzolla, A. P., Cosola, M. D., Ballini, A., Santacroce, L., Lovero, R., Testa, N. F., Lacarbonara, V., De Franco, A., Troiano, G., Cantore, S., Di Comite, M., Nocini, R., Muzio, L. L., Crincoli, V., & Dioguardi, M. (2021). The association between nutritional alterations and oral lesions in a pediatric population: An epidemiological study. BioMed Research International, 2021, 9992451. https://doi.org/10.1155/2021/9992451
- Clínica Dental Los Valles. (2018). Causas, tratamiento y contagio de las Boqueras. Clínica Dental Los Valles. https://www.clinicalosvalles.es/boqueras-causas-tratamiento-y-contagio/
- García López, E., Blanco Ruiz, A. O., Rodríguez García, L. O., Reyes Fundora, D., & Sotres Vázquez, J. (2004). Queilitis: Revisión bibliográfica. Revista Cubana de Estomatologia, 41(2), 0–0. http://scielo.sld.cu/scielo.php?script=sci_arttext&pid=S0034-75072004000200009
- Langlais, R. P., Miller, C. S., & Nield-Gehrig, J. S. (2011). Atlas a color de enfermedades bucales. Editorial El Manual Moderno. https://books.google.es/books?id=RXfLCQAAQBAJ&dq=las+boqueras+o+queilitis+se+clasifican+en+unilaterales+o+bilaterales&lr=&hl=es&source=gbs_navlinks_s
- Lei, Z., Cao, Z., Yang, Z., Ao, M., Jin, W., & Yu, L. (2019). Rosehip oil promotes excisional wound healing by accelerating the phenotypic transition of macrophages. Planta Medica, 85(7), 563–569. https://doi.org/10.1055/a-0725-8456
- Lugović-Mihić, L., Pilipović, K., Crnarić, I., Šitum, M., & Duvančić, T. (2018). Differential diagnosis of cheilitis – how to classify cheilitis? Acta Clinica Croatica, 57(2), 342–351. https://doi.org/10.20471/acc.2018.57.02.16
- Patil, S., Rao, R. S., Majumdar, B., & Anil, S. (2015). Clinical appearance of oral candida infection and therapeutic strategies. Frontiers in Microbiology, 6, 1391. https://doi.org/10.3389/fmicb.2015.01391
- Pelta, R., & Vivas, E. (1997). Piel y Alergia. I.B.D. https://books.google.es/books?id=AQDAiWLj8_YC&dq=Parietaria:+permite+aliviar+la+queilitis+de+forma+natural%3B&lr=&hl=es&source=gbs_navlinks_s
- Ras Monleón, R. M., & Riera Ras, P. (1998). Manejo de las queilitis de contacto en atención primaria. Atencion primaria, 22(1), 53–58. https://www.elsevier.es/es-revista-atencion-primaria-27-articulo-manejo-queilitis-contacto-atencion-primaria-14851
- Sánchez, M., González-Burgos, E., Iglesias, I., & Gómez-Serranillos, M. P. (2020). Pharmacological update properties of aloe Vera and its major active constituents. Molecules (Basel, Switzerland), 25(6), 1324. https://doi.org/10.3390/molecules25061324
- Siedentopp, U. (2010). La miel: producto alimenticio y medicinal eficaz contra la inflamación, la tos y la ronquera. Revista internacional de acupuntura, 4(1), 48–51. https://doi.org/10.1016/s1887-8369(10)70013-2
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








