How Do I Know if My Child Has a Tongue Fungus?

Written and verified by the dermatologist Maria del Carmen Hernandez
The immune system of children and infants isn’t fully developed, which facilitates the growth of fungi on the tongue and in other regions of the body. Therefore, this type of infection is quite common in minors, as well as being uncomfortable and unpleasant. Keep reading to learn more about it.
Causes of tongue fungus
Tongue fungus, also called thrush, is caused by the same fungus that causes vaginal infections or diaper rash. Oral candidiasis is an opportunistic infection, quite common in newborn babies. In general, the body maintains a balance of microorganisms that inhabit it, but sometimes, this is altered, so they begin to multiply exponentially. The following are the main causes:
- The use of certain antibiotics or corticosteroids to treat other infections.
- At the time of delivery, if the mother has a vaginal infection, the newborn can easily become infected by contact with the fungus.
- Impaired salivary gland function.
- It can be transmitted through the bottle nipple, so it’s best to disinfect it meticulously with a sterilizer or boiling water for 3 minutes.
- Due to extreme life situations and a diet high in carbohydrates.
The incidence varies according to certain predisposing factors and by the age of the person who develops it.

Are they contagious?
When oral candidiasis occurs, it’s likely to transmit the fungus to another person by kissing them. Then, on some occasions, they may develop characteristic lesions in the oral cavity. However, Candida doesn’t only develop in the mouth, but can also cause infections in other regions of the body, so it can also be transmitted to other parts of another person’s body. The most frequent examples are the following:
- Pregnant women who have vaginal candidiasis can pass the infection to the baby during delivery.
- If the candidiasis infection is present on the breasts or nipples, the fungus can be transmitted during breastfeeding.
- If the baby has thrush, the fungus may be transmitted during breastfeeding.
Read also: Cutaneous Mycoses in Children
Symptoms of tongue fungus
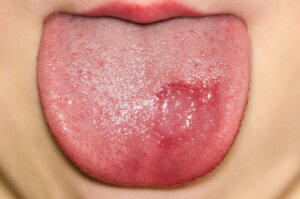
Candida growth occurs in the oral region, especially on the roof of the mouth and on the tongue. It may even spread to the pharynx or the internal mucosa of the cheeks. The clinical manifestations are characterized by whitish plaques with a granular and raised appearance. In addition, they may be accompanied by the following symptoms:
- Sore throat
- Halitosis or loss of appetite and taste
- Painful swallowing
- Active bleeding when rubbing against velvety plaques
However, certain clinical pictures have painless lesions and no other symptomatology. In addition, children may also present with a Candida rash on other areas of the body. For example, diaper rash in infants or spread to the esophagus in adults.
How to diagnose them?
In some cases, when the characteristic Candida albicans lesions grow excessively, they may be called thrush. According to a study conducted in 2010, fungi on the tongue are classified according to their location or evolution:
- Angular cheilitis: Lesions in the labial commissure.
- Chronic candidiasis: This includes variants such as erythematous, hyperplastic, nodular, or pseudomembranous.
- Acute candidiasis: Erythematous and pseudomembranous forms.
This diagnosis is made by the specialist physician during a consultation, who will perform a thorough anamnesis, taking into account the child’s health history and predisposing factors. Therefore, these data together with the clinical findings will help the doctor to arrive at a clear diagnosis. However, if there’s any doubt about it, the lesion can be scraped and studied under a microscope.
You may be interested in: 10 Home Remedies for Skin Fungus
Therapeutic options for oral candidiasis in children
In most cases, oral Candida infection usually resolves spontaneously. However, it’s essential to consult a specialist to analyze the severity of the clinical picture and indicate the correct treatment. The priority in the management of oral candidiasis is to try to alleviate any predisposing factors that can be identified. However, some of them are impossible to eradicate, such as underlying illnesses.
As a therapeutic option, drugs for topical application or oral administration (nystatin, clotrimazole, or fluconazole) are usually prescribed. In turn, it’s essential to use the correct mouthwash, as a good state of health contributes to an easier recovery. In addition, another one of the most important recommendations includes extreme hygiene measures. For example, keeping your child from putting their fingers in their mouth, washing their hands regularly, and changing their diaper frequently.
The important thing is to prevent the disease
Although thrush is a non-contagious infection caused by harmless fungi, it’s advisable to take prevention methods into account. Therefore, putting the recommendations into practice can contribute to preventing the development of candidiasis in children’s tongues. If in doubt, it’s best to consult a physician.
The immune system of children and infants isn’t fully developed, which facilitates the growth of fungi on the tongue and in other regions of the body. Therefore, this type of infection is quite common in minors, as well as being uncomfortable and unpleasant. Keep reading to learn more about it.
Causes of tongue fungus
Tongue fungus, also called thrush, is caused by the same fungus that causes vaginal infections or diaper rash. Oral candidiasis is an opportunistic infection, quite common in newborn babies. In general, the body maintains a balance of microorganisms that inhabit it, but sometimes, this is altered, so they begin to multiply exponentially. The following are the main causes:
- The use of certain antibiotics or corticosteroids to treat other infections.
- At the time of delivery, if the mother has a vaginal infection, the newborn can easily become infected by contact with the fungus.
- Impaired salivary gland function.
- It can be transmitted through the bottle nipple, so it’s best to disinfect it meticulously with a sterilizer or boiling water for 3 minutes.
- Due to extreme life situations and a diet high in carbohydrates.
The incidence varies according to certain predisposing factors and by the age of the person who develops it.

Are they contagious?
When oral candidiasis occurs, it’s likely to transmit the fungus to another person by kissing them. Then, on some occasions, they may develop characteristic lesions in the oral cavity. However, Candida doesn’t only develop in the mouth, but can also cause infections in other regions of the body, so it can also be transmitted to other parts of another person’s body. The most frequent examples are the following:
- Pregnant women who have vaginal candidiasis can pass the infection to the baby during delivery.
- If the candidiasis infection is present on the breasts or nipples, the fungus can be transmitted during breastfeeding.
- If the baby has thrush, the fungus may be transmitted during breastfeeding.
Read also: Cutaneous Mycoses in Children
Symptoms of tongue fungus
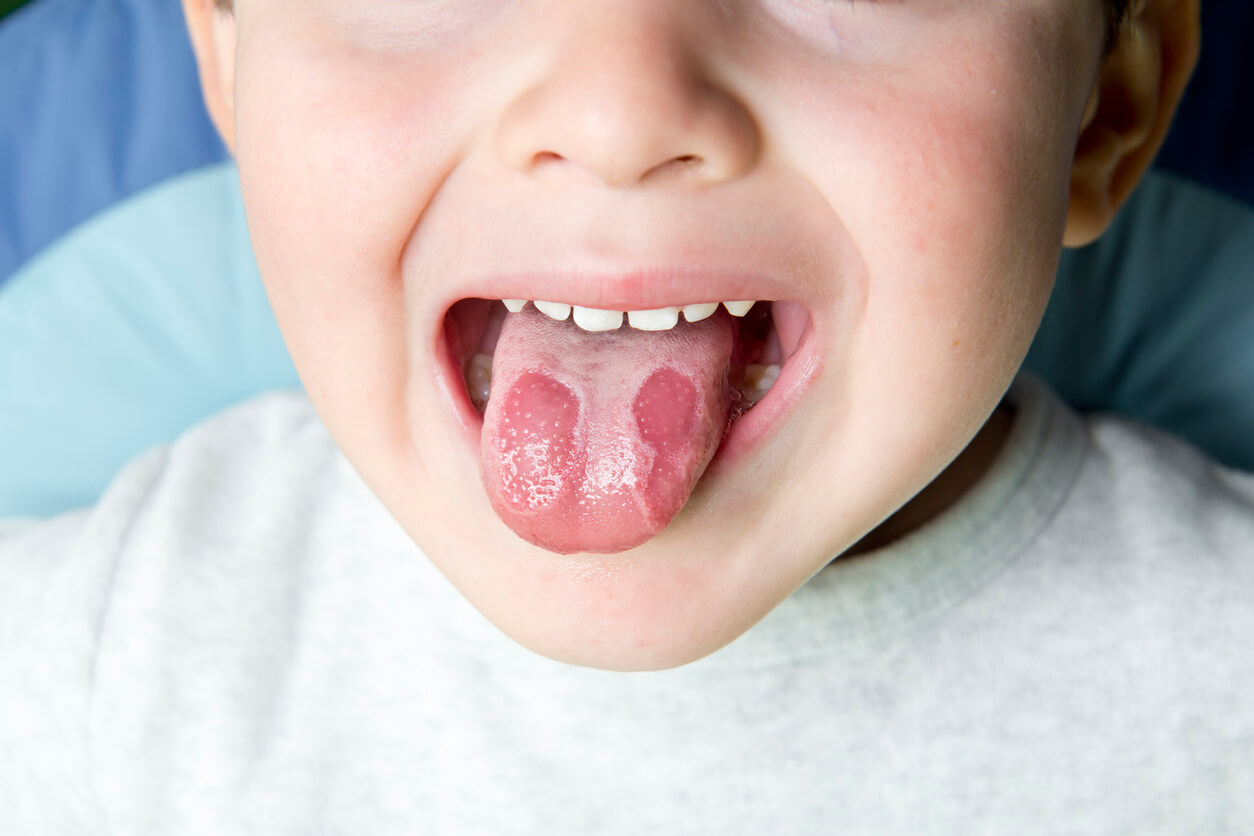
Candida growth occurs in the oral region, especially on the roof of the mouth and on the tongue. It may even spread to the pharynx or the internal mucosa of the cheeks. The clinical manifestations are characterized by whitish plaques with a granular and raised appearance. In addition, they may be accompanied by the following symptoms:
- Sore throat
- Halitosis or loss of appetite and taste
- Painful swallowing
- Active bleeding when rubbing against velvety plaques
However, certain clinical pictures have painless lesions and no other symptomatology. In addition, children may also present with a Candida rash on other areas of the body. For example, diaper rash in infants or spread to the esophagus in adults.
How to diagnose them?
In some cases, when the characteristic Candida albicans lesions grow excessively, they may be called thrush. According to a study conducted in 2010, fungi on the tongue are classified according to their location or evolution:
- Angular cheilitis: Lesions in the labial commissure.
- Chronic candidiasis: This includes variants such as erythematous, hyperplastic, nodular, or pseudomembranous.
- Acute candidiasis: Erythematous and pseudomembranous forms.
This diagnosis is made by the specialist physician during a consultation, who will perform a thorough anamnesis, taking into account the child’s health history and predisposing factors. Therefore, these data together with the clinical findings will help the doctor to arrive at a clear diagnosis. However, if there’s any doubt about it, the lesion can be scraped and studied under a microscope.
You may be interested in: 10 Home Remedies for Skin Fungus

Therapeutic options for oral candidiasis in children
In most cases, oral Candida infection usually resolves spontaneously. However, it’s essential to consult a specialist to analyze the severity of the clinical picture and indicate the correct treatment. The priority in the management of oral candidiasis is to try to alleviate any predisposing factors that can be identified. However, some of them are impossible to eradicate, such as underlying illnesses.
As a therapeutic option, drugs for topical application or oral administration (nystatin, clotrimazole, or fluconazole) are usually prescribed. In turn, it’s essential to use the correct mouthwash, as a good state of health contributes to an easier recovery. In addition, another one of the most important recommendations includes extreme hygiene measures. For example, keeping your child from putting their fingers in their mouth, washing their hands regularly, and changing their diaper frequently.
The important thing is to prevent the disease
Although thrush is a non-contagious infection caused by harmless fungi, it’s advisable to take prevention methods into account. Therefore, putting the recommendations into practice can contribute to preventing the development of candidiasis in children’s tongues. If in doubt, it’s best to consult a physician.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Sharon V, Fazel N. Oral candidiasis and angular cheilitis. Dermatol Ther. 2010 May-Jun;23(3):230-42. doi: 10.1111/j.1529-8019.2010.01320.x. PMID: 20597942.
- Fang J, Huang B, Ding Z. Efficacy of antifungal drugs in the treatment of oral candidiasis: A Bayesian network meta-analysis. J Prosthet Dent. 2021 Feb;125(2):257-265. doi: 10.1016/j.prosdent.2019.12.025. Epub 2020 Mar 10. PMID: 32165010.
- Vila T, Sultan AS, Montelongo-Jauregui D, Jabra-Rizk MA. Oral Candidiasis: A Disease of Opportunity. J Fungi (Basel). 2020 Jan 16;6(1):15. doi: 10.3390/jof6010015. PMID: 31963180; PMCID: PMC7151112.
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








