Onychomadesis in Children: What You Should Know

Written and verified by the dermatologist Maria del Carmen Hernandez
Although onychomadesis in children isn’t one of the most common nail injuries in little ones, it’s important to be aware of it in order to know how to handle it. Especially because the appearance it produces in the hands of infants attracts a lot of attention.
Here, we’ll tell you everything you should know about this transitory and benign condition. Are you interested? Keep reading!
What is onychomadesis in children?
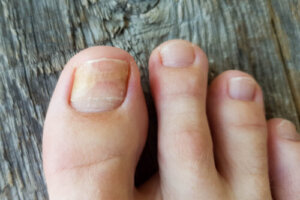
Onychomadesis is the complete and spontaneous detachment of the nail plate from its proximal fold, with no signs of inflammation or pain.
This detachment has no clear cause, but it’s assumed that it could be caused by a temporary halt in the activity of the nail matrix. In general, this phenomenon is related to some acute viral conditions suffered by children.
Unlike fungal infections, nail detachment occurs in the proximal area and can affect both fingers and toes.
The causes of onychomadesis in children
The most frequent causes include mechanical trauma, autoimmune diseases, drugs, or infections. There’s also a group of undetermined causes, which is the most common of all.
Many times, onychomadesis in children can occur as a side effect of the following systemic diseases:
- Kawasaki disease
- Blistering dermatoses
- Paronychia
- Radiation therapy
- Stress
Hand, foot, and mouth disease

Among the infectious causes, hand, foot, and mouth disease is the most common. This viral infectious illness is quite frequent in childhood, during the summer or autumn months. It’s caused by coxsackievirus A and enterovirus 71.
The most characteristic skin lesions are small, oval, reddish vesicles appearing on the hands, feet, and mouth. In general, the condition appears in the form of outbreaks in preschools and daycare centers.
The natural evolution of the infection follows a certain sequence. It starts with an incubation period of approximately 3 to 6 days, and then, vesicles appear in the oral cavity. After a short time, these erode and leave ulcers with a characteristic red rim. Finally, the outbreak appears on other areas of the body, mainly on the palms of the hands and soles of the feet.
This disease resolves spontaneously within a week and doesn’t require curative medical treatment.
Read also: 10 Childhood Diseases that Can Be Avoided with Handwashing
Inadequate footwear, a common cause of onychomadesis in children
In addition to infectious causes, nail detachment can develop due to improperly sized footwear. This phenomenon is also observed in athletes who don’t wear wide shoes.
Even when children wear closed shoes and have very long toenails, constant trauma to the nail bed is generated and this favors the detachment of the plate.
Clinical manifestations of onychomadesis in children
In children with onychomadesis, a proximal separation of the nail bed is evident and sometimes there are also shallow transverse grooves.
There’s usually no subungual hyperkeratosis or periungual lesions, and, in most cases, the cuticle remains intact.
The following are some characteristic signs that accompany nail detachment.
Beau’s lines
Onychomadesis is considered a severe form of Beau’s lines, which are transverse ridges or grooves that run from one lateral nail fold to the other. They result from a momentary disruption of the growth of the proximal nail matrix.
Some of the causes of Beau’s lines include local trauma and some systemic triggers such as the following:
- Severe malnutrition
- Febrile illness
- Pemphigus
- Kawasaki disease.
- Raynaud’s disease.
Like onychomadesis, there’s no specific therapy for Beau’s lines, as they resolve spontaneously when the underlying condition disappears.
After detachment of the nail from the nail bed, whatever the cause, the nail doesn’t reattach. In fact, a new nail grows underneath slowly until it completely replaces it.
Fingernails take about 6 months to grow out, while toenails can take up to 18 months.
Diagnosis and treatment
The diagnosis of onychomadesis is based on clinical manifestations and a thorough questioning regarding personal history.
In the beginning, the nail plate shows a transverse depression line (called Beau’s line). If the nail matrix remains injured for a long time, this line deepens until the nail plate is completely separated from the nail.
Onychomadesis doesn’t require any particular treatment. That is, just keeping the area clean and preventing further trauma is sufficient. However, home management may include keeping the area dry to prevent infection.
After about 6 to 12 weeks, the problem resolves spontaneously.
You may be interested in: Ingrown Nails in Babies: Prevention and Treatment
Tips for nail care

During the process of replacing the detached plate, it’s a good idea to practice certain care measures to keep the nails clean and germ-free:
- Trim the nail or file the sharp edges that may appear to prevent it from catching and detaching even more.
- Don’t attempt to trim the part of the nail that’s detached, just leave it as it is. When the new nail begins to grow, the old nail will fall off on its own.
- A thin layer of petroleum jelly can be applied and the area covered with a bandage.
A benign and transient condition
Although partial or total nail growth arrest isn’t a common condition in children, when it occurs, it can cause some concern in parents.
The prognosis of onychomadesis, in most cases, is very good, as it’s a temporary condition. At the end of the process, the new nail will grow under the injured one.
Although onychomadesis in children isn’t one of the most common nail injuries in little ones, it’s important to be aware of it in order to know how to handle it. Especially because the appearance it produces in the hands of infants attracts a lot of attention.
Here, we’ll tell you everything you should know about this transitory and benign condition. Are you interested? Keep reading!
What is onychomadesis in children?
Onychomadesis is the complete and spontaneous detachment of the nail plate from its proximal fold, with no signs of inflammation or pain.
This detachment has no clear cause, but it’s assumed that it could be caused by a temporary halt in the activity of the nail matrix. In general, this phenomenon is related to some acute viral conditions suffered by children.
Unlike fungal infections, nail detachment occurs in the proximal area and can affect both fingers and toes.
The causes of onychomadesis in children
The most frequent causes include mechanical trauma, autoimmune diseases, drugs, or infections. There’s also a group of undetermined causes, which is the most common of all.
Many times, onychomadesis in children can occur as a side effect of the following systemic diseases:
- Kawasaki disease
- Blistering dermatoses
- Paronychia
- Radiation therapy
- Stress
Hand, foot, and mouth disease

Among the infectious causes, hand, foot, and mouth disease is the most common. This viral infectious illness is quite frequent in childhood, during the summer or autumn months. It’s caused by coxsackievirus A and enterovirus 71.
The most characteristic skin lesions are small, oval, reddish vesicles appearing on the hands, feet, and mouth. In general, the condition appears in the form of outbreaks in preschools and daycare centers.
The natural evolution of the infection follows a certain sequence. It starts with an incubation period of approximately 3 to 6 days, and then, vesicles appear in the oral cavity. After a short time, these erode and leave ulcers with a characteristic red rim. Finally, the outbreak appears on other areas of the body, mainly on the palms of the hands and soles of the feet.
This disease resolves spontaneously within a week and doesn’t require curative medical treatment.
Read also: 10 Childhood Diseases that Can Be Avoided with Handwashing
Inadequate footwear, a common cause of onychomadesis in children
In addition to infectious causes, nail detachment can develop due to improperly sized footwear. This phenomenon is also observed in athletes who don’t wear wide shoes.
Even when children wear closed shoes and have very long toenails, constant trauma to the nail bed is generated and this favors the detachment of the plate.
Clinical manifestations of onychomadesis in children
In children with onychomadesis, a proximal separation of the nail bed is evident and sometimes there are also shallow transverse grooves.
There’s usually no subungual hyperkeratosis or periungual lesions, and, in most cases, the cuticle remains intact.
The following are some characteristic signs that accompany nail detachment.
Beau’s lines
Onychomadesis is considered a severe form of Beau’s lines, which are transverse ridges or grooves that run from one lateral nail fold to the other. They result from a momentary disruption of the growth of the proximal nail matrix.
Some of the causes of Beau’s lines include local trauma and some systemic triggers such as the following:
- Severe malnutrition
- Febrile illness
- Pemphigus
- Kawasaki disease.
- Raynaud’s disease.
Like onychomadesis, there’s no specific therapy for Beau’s lines, as they resolve spontaneously when the underlying condition disappears.
After detachment of the nail from the nail bed, whatever the cause, the nail doesn’t reattach. In fact, a new nail grows underneath slowly until it completely replaces it.
Fingernails take about 6 months to grow out, while toenails can take up to 18 months.
Diagnosis and treatment
The diagnosis of onychomadesis is based on clinical manifestations and a thorough questioning regarding personal history.
In the beginning, the nail plate shows a transverse depression line (called Beau’s line). If the nail matrix remains injured for a long time, this line deepens until the nail plate is completely separated from the nail.
Onychomadesis doesn’t require any particular treatment. That is, just keeping the area clean and preventing further trauma is sufficient. However, home management may include keeping the area dry to prevent infection.
After about 6 to 12 weeks, the problem resolves spontaneously.
You may be interested in: Ingrown Nails in Babies: Prevention and Treatment
Tips for nail care

During the process of replacing the detached plate, it’s a good idea to practice certain care measures to keep the nails clean and germ-free:
- Trim the nail or file the sharp edges that may appear to prevent it from catching and detaching even more.
- Don’t attempt to trim the part of the nail that’s detached, just leave it as it is. When the new nail begins to grow, the old nail will fall off on its own.
- A thin layer of petroleum jelly can be applied and the area covered with a bandage.
A benign and transient condition
Although partial or total nail growth arrest isn’t a common condition in children, when it occurs, it can cause some concern in parents.
The prognosis of onychomadesis, in most cases, is very good, as it’s a temporary condition. At the end of the process, the new nail will grow under the injured one.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Chiu HH, Wu CS, Lan CE. Onychomadesis: A Late Complication of Hand, Foot, and Mouth Disease. J Emerg Med. 2017 Feb;52(2):243-245. doi: 10.1016/j.jemermed.2016.01.034. Epub 2016 Oct 4. PMID: 27717588.
- Jandial A, Mishra K, Prakash G, Malhotra P. Beau’s lines. BMJ Case Rep. 2018 Mar 28;2018:bcr2018224978. doi: 10.1136/bcr-2018-224978. PMID: 29593008; PMCID: PMC5878284.
- Salgado F, Handler MZ, Schwartz RA. Shedding light on onychomadesis. Cutis. 2017 Jan;99(1):33-36. PMID: 28207011.
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








