Keratosis Pilaris in Children: Symptoms, Causes and Treatment

Written and verified by the dermatologist Maria del Carmen Hernandez
Keratosis Pilaris in children is one of the most common skin conditions and some even consider it to be a normal skin condition. In fact, it’s the most common follicular keratosis.
It’s a benign dermatological condition that usually concerns parents and leads them to consult a doctor.
What is keratosis pilaris in children?
According to research in The British Journal of Dermatology, keratosis pilaris appears for the first time in childhood, and evolves and becomes more extensive during the second part of life.
This condition is also known as “chicken skin,” and it’s often related to other syndromes, like Noonan Syndrome and Down Syndrome. In addition, it’s associated with other illnesses, such as atopic dermatitis mellitus, vulgar ichthyosis, diabetes mellitus, obesity and malnutrition.
Why does keratosis pilaris occur?
This skin condition has an autosomal dominant inheritance which causes a mutation to occur in the filaggrin, just like with atopic dermatitis.
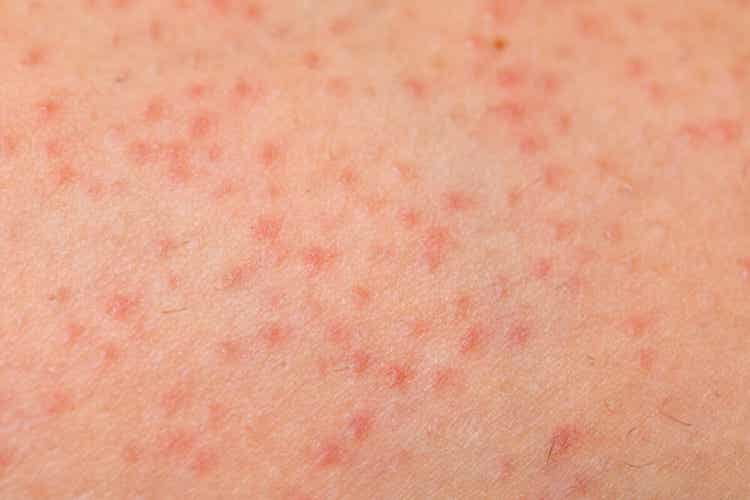
Both skin conditions cause a loss of epithelial barrier function. Therefore, its cause lies in the abnormal keratinization of the follicle opening, which leads to the blockage in the infundibulum.
The formation of these keratin blockages causes erythema on the skin’s surface and a slight peeling around each follicle.
Symptoms and signs of keratosis pilaris
This skin condition presents itself as keratin lugs in the follicular openings together with different degrees of peripollicular erythema. In addition, it can show up anywhere on the skin that has hair follicles. Therefore, you’ll never see this condition on the palms of your hands or the soles of your feet.
This asymptomatic condition occurs on the extensor surfaces of the proximal upper and lower extremities. Also, it can occur on the buttocks. You may notice coiled hairs inside the lesions, which are responsible for inflammation and keratinization.
The affected area of the skin will feel rough and dry, like sandpaper. Also, people who have dry skin, eczema, hay fever or ichthyosis are more likely to develop this condition.
Keep reading: 10 Effective Skincare Tips for Teenagers
Treatment options
The diagnosis of this condition is clinical and will be based on the dermatological findings at the time of the physical examination. Although keratosis pilaris in children is an asymptomatic condition that tends to improve over time, there are also therapeutic options that can help you manage it and improve it.
Proper hygiene
We recommend using hypoallergenic soaps and vegetable sponges when bathing. Also, try not to generate too much friction when washing. Instead, you should gently exfoliate to remove the dead cells.
In addition, you should limit the amount of time you spend bathing because prolonged times tend to eliminate your skin’s fatty acids. These fatty acids help your skin’s barrier function correctly.
Also, you shouldn’t touch the papules on the surface of your skin. Doing so increases the probability of creating other lesions.
Constantly moisturize
After each shower, when the skin can absorb moisture the most, you should apply a moisturizing cream to your body. When choosing a lotion, be sure to look at its components and appearance.
Lotions with vitamin A, lactic acid, vitamin E or allantoin are ideal for moisturizing dry skin and helping your skin’s surface renew itself. While applying lotion can help prevent keratosis pilaris in children, it’s also helpful for those who already suffer from it. Using lotion can keep the lesions from becoming inflamed when the skin is dry.
Specific products
To improve your skin’s texture, you should use lotions with salicylic acid or urea-based creams. When using these creams, keratosis pilaris in children tends to fade after a few weeks. Both ingredients help loosen and remove dead cells from the skin’s surface, which helps to smooth the skin.

There are other types of more invasive aesthetic treatments for this condition. For example, other options to improve your skin’s appearance include chemical peels, retinol creams and diamond-tipped microdermabrasion.
Keratosis pilaris, more than a skin issue
Keratosis pilaris in children usually develops during childhood and improves over time. In addition, it’s a condition that doesn’t cause any major symptoms, only aesthetic discomfort. Also, it tends to not be contagious and it worsens in the winter months since that’s when skin is likely to dry out.
Even though it’s a harmless genetic skin condition, patients’ distress over their appearance can cause them concern and make them want to improve it.
Keratosis Pilaris in children is one of the most common skin conditions and some even consider it to be a normal skin condition. In fact, it’s the most common follicular keratosis.
It’s a benign dermatological condition that usually concerns parents and leads them to consult a doctor.
What is keratosis pilaris in children?
According to research in The British Journal of Dermatology, keratosis pilaris appears for the first time in childhood, and evolves and becomes more extensive during the second part of life.
This condition is also known as “chicken skin,” and it’s often related to other syndromes, like Noonan Syndrome and Down Syndrome. In addition, it’s associated with other illnesses, such as atopic dermatitis mellitus, vulgar ichthyosis, diabetes mellitus, obesity and malnutrition.
Why does keratosis pilaris occur?
This skin condition has an autosomal dominant inheritance which causes a mutation to occur in the filaggrin, just like with atopic dermatitis.

Both skin conditions cause a loss of epithelial barrier function. Therefore, its cause lies in the abnormal keratinization of the follicle opening, which leads to the blockage in the infundibulum.
The formation of these keratin blockages causes erythema on the skin’s surface and a slight peeling around each follicle.
Symptoms and signs of keratosis pilaris
This skin condition presents itself as keratin lugs in the follicular openings together with different degrees of peripollicular erythema. In addition, it can show up anywhere on the skin that has hair follicles. Therefore, you’ll never see this condition on the palms of your hands or the soles of your feet.
This asymptomatic condition occurs on the extensor surfaces of the proximal upper and lower extremities. Also, it can occur on the buttocks. You may notice coiled hairs inside the lesions, which are responsible for inflammation and keratinization.
The affected area of the skin will feel rough and dry, like sandpaper. Also, people who have dry skin, eczema, hay fever or ichthyosis are more likely to develop this condition.
Keep reading: 10 Effective Skincare Tips for Teenagers
Treatment options
The diagnosis of this condition is clinical and will be based on the dermatological findings at the time of the physical examination. Although keratosis pilaris in children is an asymptomatic condition that tends to improve over time, there are also therapeutic options that can help you manage it and improve it.
Proper hygiene
We recommend using hypoallergenic soaps and vegetable sponges when bathing. Also, try not to generate too much friction when washing. Instead, you should gently exfoliate to remove the dead cells.
In addition, you should limit the amount of time you spend bathing because prolonged times tend to eliminate your skin’s fatty acids. These fatty acids help your skin’s barrier function correctly.
Also, you shouldn’t touch the papules on the surface of your skin. Doing so increases the probability of creating other lesions.
Constantly moisturize
After each shower, when the skin can absorb moisture the most, you should apply a moisturizing cream to your body. When choosing a lotion, be sure to look at its components and appearance.
Lotions with vitamin A, lactic acid, vitamin E or allantoin are ideal for moisturizing dry skin and helping your skin’s surface renew itself. While applying lotion can help prevent keratosis pilaris in children, it’s also helpful for those who already suffer from it. Using lotion can keep the lesions from becoming inflamed when the skin is dry.
Specific products
To improve your skin’s texture, you should use lotions with salicylic acid or urea-based creams. When using these creams, keratosis pilaris in children tends to fade after a few weeks. Both ingredients help loosen and remove dead cells from the skin’s surface, which helps to smooth the skin.

There are other types of more invasive aesthetic treatments for this condition. For example, other options to improve your skin’s appearance include chemical peels, retinol creams and diamond-tipped microdermabrasion.
Keratosis pilaris, more than a skin issue
Keratosis pilaris in children usually develops during childhood and improves over time. In addition, it’s a condition that doesn’t cause any major symptoms, only aesthetic discomfort. Also, it tends to not be contagious and it worsens in the winter months since that’s when skin is likely to dry out.
Even though it’s a harmless genetic skin condition, patients’ distress over their appearance can cause them concern and make them want to improve it.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Clinica Mayo. Queratosis pilaris. Julio 2021.
- Fenner J, Silverberg NB. Skin diseases associated with atopic dermatitis. Clin Dermatol. 2018 Sep-Oct;36(5):631-640. doi: 10.1016/j.clindermatol.2018.05.004. Epub 2018 Jun 1. PMID: 30217275.
- Gerbig AW. Treating keratosis pilaris. J Am Acad Dermatol. 2002 Sep;47(3):457. doi: 10.1067/mjd.2002.122733. PMID: 12196765.
- Hwang S, Schwartz RA. Keratosis pilaris: a common follicular hyperkeratosis. Cutis. 2008 Sep;82(3):177-80. PMID: 18856156.
- Poskitt L, Wilkinson JD. Natural history of keratosis pilaris. Br J Dermatol. 1994 Jun;130(6):711-3. doi: 10.1111/j.1365-2133.1994.tb03406.x. PMID: 8011494.
- Society for Pediatric Dermatology. ¿Qué es la queratosis pilaris? 2019.
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








