The 6 Most Common Mouth Infections in Children

Bacteria, viruses, and fungi can cause diseases that manifest within the oral cavity. Knowing about them will help you to be prepared to prevent them and in case they appear, to know what to expect and how to best accompany your little one. That’s why today we’re going to tell you which are the most common mouth infections in children. Don’t stop reading!
The 6 most common mouth infections in children
1. Tooth decay
Tooth decay is one of the most common and frequent mouth infections in children. It’s the destruction of the hard tissues of the teeth by the action of acids that are obtained by metabolizing sugars in the diet.
According to the World Health Organization (WHO):
“According to the Global Burden of Disease Study, in 2017 more than 530 million children worldwide had dental caries in baby teeth.“
It’s considered an infection because one of the necessary factors for its development is the accumulation of bacteria in the mouth. Streptococcus mutans is the most significant microbial agent in this process of dental destruction.
When a cavity first starts, it’s observed as white spots on the teeth, which later turn yellow, brown, and even black. If the child doesn’t receive dental care in a timely manner, the process continues and advances in extension and depth until the complete loss of the tooth. This causes problems with esthetics, eating, speaking, and occluding the mouth properly.
You may be interested in: 5 Dietary Recommendations to Prevent Cavities in Children
The good news is that this mouth infection can be prevented with proper oral hygiene, the use of fluorides, and a healthy diet. Brushing your child’s teeth every day with fluoride toothpaste and cutting down on sweets and soft drinks is one of the best ways to prevent cavities.
And if the decaying process occurs anyway, there are dental treatments to put an end to the problem and restore your child’s oral health. The earlier they’re performed, the simpler and more comfortable they’ll be, so regular check-ups with the pediatric dentist are essential.

2. Gingivitis and periodontal disease
Gingivitis is another disease caused by the accumulation of bacterial plaque. When the germs in the mouth aren’t eliminated correctly with brushing, they irritate the gingival tissue and inflame it.
Inflamed gums look red and swollen, are uncomfortable, and bleed during brushing. If this problem isn’t treated in time, it can progress to pyorrhea or periodontal disease. This last scenario isn’t the most common in children, but it’s still a possibility. In this scenario, inflammation and infection move to deeper areas and eventually affect the supporting tissues of the teeth.
Daily oral hygiene and professional dental cleanings are the best options to prevent gingivitis in children’s mouths. Performing proper tooth brushing, flossing and using fluoride toothpastes, and visiting the dentist every 6 months can prevent gum problems.
3. Candidiasis or thrush
Candidiasis, also known as thrush, is another common mouth infection in children.
This infection is caused by the fungus Candida albicans, which is part of the usual flora of the mouth. Under certain conditions favorable to the microorganism, its growth increases, thus disrupting the balance of the oral ecosystem and infecting oral tissues.
Excessive or frequent use of antibiotics, excessive oral hygiene, certain medical treatments, or some systemic diseases are examples of conditions that may favor its appearance.
Thrush is characterized by the appearance of small white patches on the tongue, corner of the lips, cheeks, palate, and other areas of the oral mucosa. It has the appearance of coagulated milk and doesn’t come off when trying to remove it with gauze.
When the child presents these spots in the mouth, it’s appropriate to take them to the pediatrician or pediatric dentist for appropriate treatment.
4. Oral herpes
Herpes virus infections are quite common in childhood and the same agent can give rise to two different processes.
Herpetic gingivostomatitis
This is the clinical picture caused by the first infection of the herpes virus. It’s most common in young children, between 0 and 3 years of age.
The characteristic symptom is inflammation and bleeding of the gums and the appearance of small blisters and ulcers throughout the mouth. These are very painful and make feeding and hydration of the infant difficult. In addition, they may be accompanied by fever, excessive drooling, irritability and tiredness.
The process usually lasts about a week and disappears spontaneously. However, the doctor may prescribe medication to alleviate pain and help the child to continue feeding. Dehydration is a very common complication that should be prevented.
Like all herpes, it’s easily spread, so it’s best to avoid contact with other children during the outbreak. Washing hands and the utensils and toys that babies put in their mouths is essential to preventing transmission at home.
You should know that the first infection of the herpes virus doesn’t always cause this clinical picture and that in some children, it may go completely unnoticed.
Recurrent cold sores
Oral herpes also causes small, painful lesions in the mouth or on the skin of the lips, in the form of cluster blisters. And when they break (because they itch a lot), they leave yellowish crusts that heal after a few days.
This infection is caused by the herpes simplex virus and once the child has already been infected, this infectious agent remains latent in his body for the rest of their life.
When for some reason the defenses decrease and the virus finds an opportune situation, it reactivates and causes the symptomatology again. The consumption of certain foods, exposure to the sun, colds, trauma, or moments of stress are some of the factors that can contribute to the appearance of the symptoms again.
The whole process usually lasts from one week to 10 days and, in general, doesn’t require treatment. However, an antiviral can be applied topically to the lesions to accelerate healing.
Oral herpes outbreaks are contagious, so it’s important to wash your children’s hands thoroughly and prevent them from touching the sores. Keep in mind that the virus can move to other mucous membranes from contaminated hands.
5. Hand, foot, and mouth disease
Hand, foot, and mouth disease is an infection caused by Coxsackievirus A16 or enterovirus 71. It affects not only the mouth, but also the skin on other parts of the body.
The symptoms are characterized by a sore throat and fever. Painful blisters develop on the cheeks and tongue, palms of the hands, soles of the feet, and buttocks.
This process affects young children and school-age children and, although often annoying, tends to disappear within three to seven days.
6. Herpangina
Herpangina is another common mouth infection in children also caused by a virus. The origin, in fact, is usually the same as that of hand, foot, and mouth disease: Coxsackie A and enteroviruses.
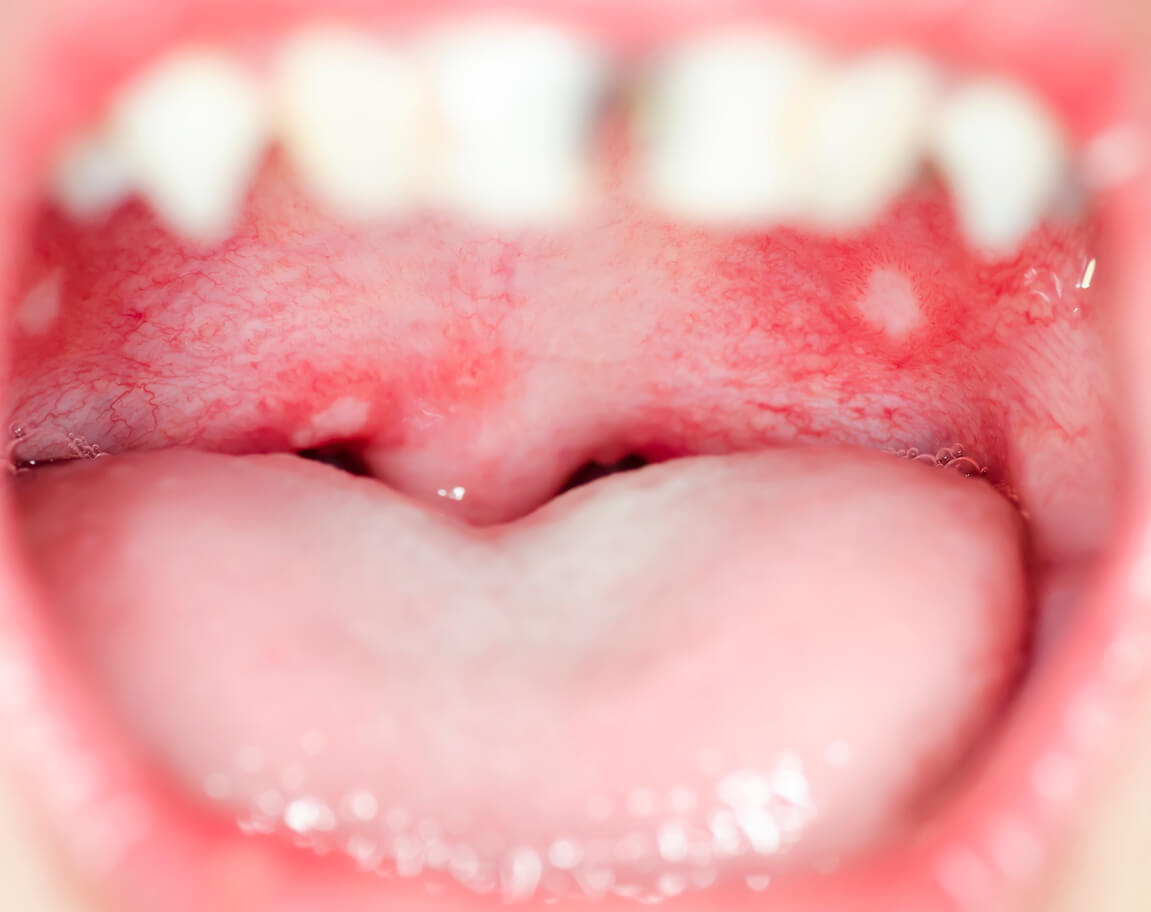
The most frequent location is the soft palate, tonsils, and throat and the symptoms are usually accompanied by fever, sore throat, and difficulty in swallowing.
This infection manifests itself through small red spots at the back of the mouth. These quickly turn into liquid blisters, which then rupture and give rise to the painful sores. The latter are so annoying that they cause the child to refuse food and water. However, they disappear on their own within 5 to 10 days.
It most often affects infants between the ages of 3 and 10 years, especially in the summer and autumn seasons.
At this stage, it’s important to ensure that the child is hydrated. Pain medication or home remedies can also be used to alleviate symptoms.

How to prevent mouth infections in children
The most common causes of mouth infections in children can be viruses, bacteria, and fungi. The arrival of germs sometimes can’t be avoided. But with some simple measures, it’ll be possible to reduce the risk of getting sick.
Diet care and proper oral hygiene are two fundamental strategies to reduce the accumulation of bacterial plaque. Regular visits to the dentist are also key to controlling bacteria and maintaining oral health.
Avoid tasting babies’ food, cleaning their utensils with saliva, or kissing them on the mouth helps to reduce the transmission of germs. Cleaning the home and the products used by little ones, together with proper hand hygiene also favors prevention.
And if infections appear, going to the pediatrician or dentist to seek professional help is the best way to accompany your little one.
Bacteria, viruses, and fungi can cause diseases that manifest within the oral cavity. Knowing about them will help you to be prepared to prevent them and in case they appear, to know what to expect and how to best accompany your little one. That’s why today we’re going to tell you which are the most common mouth infections in children. Don’t stop reading!
The 6 most common mouth infections in children
1. Tooth decay
Tooth decay is one of the most common and frequent mouth infections in children. It’s the destruction of the hard tissues of the teeth by the action of acids that are obtained by metabolizing sugars in the diet.
According to the World Health Organization (WHO):
“According to the Global Burden of Disease Study, in 2017 more than 530 million children worldwide had dental caries in baby teeth.“
It’s considered an infection because one of the necessary factors for its development is the accumulation of bacteria in the mouth. Streptococcus mutans is the most significant microbial agent in this process of dental destruction.
When a cavity first starts, it’s observed as white spots on the teeth, which later turn yellow, brown, and even black. If the child doesn’t receive dental care in a timely manner, the process continues and advances in extension and depth until the complete loss of the tooth. This causes problems with esthetics, eating, speaking, and occluding the mouth properly.
You may be interested in: 5 Dietary Recommendations to Prevent Cavities in Children
The good news is that this mouth infection can be prevented with proper oral hygiene, the use of fluorides, and a healthy diet. Brushing your child’s teeth every day with fluoride toothpaste and cutting down on sweets and soft drinks is one of the best ways to prevent cavities.
And if the decaying process occurs anyway, there are dental treatments to put an end to the problem and restore your child’s oral health. The earlier they’re performed, the simpler and more comfortable they’ll be, so regular check-ups with the pediatric dentist are essential.

2. Gingivitis and periodontal disease
Gingivitis is another disease caused by the accumulation of bacterial plaque. When the germs in the mouth aren’t eliminated correctly with brushing, they irritate the gingival tissue and inflame it.
Inflamed gums look red and swollen, are uncomfortable, and bleed during brushing. If this problem isn’t treated in time, it can progress to pyorrhea or periodontal disease. This last scenario isn’t the most common in children, but it’s still a possibility. In this scenario, inflammation and infection move to deeper areas and eventually affect the supporting tissues of the teeth.
Daily oral hygiene and professional dental cleanings are the best options to prevent gingivitis in children’s mouths. Performing proper tooth brushing, flossing and using fluoride toothpastes, and visiting the dentist every 6 months can prevent gum problems.
3. Candidiasis or thrush
Candidiasis, also known as thrush, is another common mouth infection in children.
This infection is caused by the fungus Candida albicans, which is part of the usual flora of the mouth. Under certain conditions favorable to the microorganism, its growth increases, thus disrupting the balance of the oral ecosystem and infecting oral tissues.
Excessive or frequent use of antibiotics, excessive oral hygiene, certain medical treatments, or some systemic diseases are examples of conditions that may favor its appearance.
Thrush is characterized by the appearance of small white patches on the tongue, corner of the lips, cheeks, palate, and other areas of the oral mucosa. It has the appearance of coagulated milk and doesn’t come off when trying to remove it with gauze.
When the child presents these spots in the mouth, it’s appropriate to take them to the pediatrician or pediatric dentist for appropriate treatment.
4. Oral herpes
Herpes virus infections are quite common in childhood and the same agent can give rise to two different processes.
Herpetic gingivostomatitis
This is the clinical picture caused by the first infection of the herpes virus. It’s most common in young children, between 0 and 3 years of age.
The characteristic symptom is inflammation and bleeding of the gums and the appearance of small blisters and ulcers throughout the mouth. These are very painful and make feeding and hydration of the infant difficult. In addition, they may be accompanied by fever, excessive drooling, irritability and tiredness.
The process usually lasts about a week and disappears spontaneously. However, the doctor may prescribe medication to alleviate pain and help the child to continue feeding. Dehydration is a very common complication that should be prevented.
Like all herpes, it’s easily spread, so it’s best to avoid contact with other children during the outbreak. Washing hands and the utensils and toys that babies put in their mouths is essential to preventing transmission at home.
You should know that the first infection of the herpes virus doesn’t always cause this clinical picture and that in some children, it may go completely unnoticed.

Recurrent cold sores
Oral herpes also causes small, painful lesions in the mouth or on the skin of the lips, in the form of cluster blisters. And when they break (because they itch a lot), they leave yellowish crusts that heal after a few days.
This infection is caused by the herpes simplex virus and once the child has already been infected, this infectious agent remains latent in his body for the rest of their life.
When for some reason the defenses decrease and the virus finds an opportune situation, it reactivates and causes the symptomatology again. The consumption of certain foods, exposure to the sun, colds, trauma, or moments of stress are some of the factors that can contribute to the appearance of the symptoms again.
The whole process usually lasts from one week to 10 days and, in general, doesn’t require treatment. However, an antiviral can be applied topically to the lesions to accelerate healing.
Oral herpes outbreaks are contagious, so it’s important to wash your children’s hands thoroughly and prevent them from touching the sores. Keep in mind that the virus can move to other mucous membranes from contaminated hands.
5. Hand, foot, and mouth disease
Hand, foot, and mouth disease is an infection caused by Coxsackievirus A16 or enterovirus 71. It affects not only the mouth, but also the skin on other parts of the body.
The symptoms are characterized by a sore throat and fever. Painful blisters develop on the cheeks and tongue, palms of the hands, soles of the feet, and buttocks.
This process affects young children and school-age children and, although often annoying, tends to disappear within three to seven days.
6. Herpangina
Herpangina is another common mouth infection in children also caused by a virus. The origin, in fact, is usually the same as that of hand, foot, and mouth disease: Coxsackie A and enteroviruses.
The most frequent location is the soft palate, tonsils, and throat and the symptoms are usually accompanied by fever, sore throat, and difficulty in swallowing.
This infection manifests itself through small red spots at the back of the mouth. These quickly turn into liquid blisters, which then rupture and give rise to the painful sores. The latter are so annoying that they cause the child to refuse food and water. However, they disappear on their own within 5 to 10 days.
It most often affects infants between the ages of 3 and 10 years, especially in the summer and autumn seasons.
At this stage, it’s important to ensure that the child is hydrated. Pain medication or home remedies can also be used to alleviate symptoms.

How to prevent mouth infections in children
The most common causes of mouth infections in children can be viruses, bacteria, and fungi. The arrival of germs sometimes can’t be avoided. But with some simple measures, it’ll be possible to reduce the risk of getting sick.
Diet care and proper oral hygiene are two fundamental strategies to reduce the accumulation of bacterial plaque. Regular visits to the dentist are also key to controlling bacteria and maintaining oral health.
Avoid tasting babies’ food, cleaning their utensils with saliva, or kissing them on the mouth helps to reduce the transmission of germs. Cleaning the home and the products used by little ones, together with proper hand hygiene also favors prevention.
And if infections appear, going to the pediatrician or dentist to seek professional help is the best way to accompany your little one.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Muñoz-Sandoval, C., Gambetta-Tessini, K., Santamaría, R. M., Splieth, C., Paris, S., Schwendicke, F., & Giacaman, R. A. (2022). ¿ Cómo Intervenir el Proceso de Caries en Niños? Adaptación del Consenso de ORCA/EFCD/DGZ. International journal of interdisciplinary dentistry, 15(1), 48-53.
- Castro-Rodríguez, Y. (2018). Enfermedad periodontal en niños y adolescentes. A propósito de un caso clínico. Revista clínica de periodoncia, implantología y rehabilitación oral, 11(1), 36-38.
- Chuchuca Mite, G. D. (2019). Prevalencia de gingivitis en niños de 5 a 8 años de edad de la Escuela Coronel Luciano Coral de Guayaquil (Bachelor’s thesis, Universidad de Guayaquil. Facultad Piloto de Odontología).
- Proaño Añazco, V. S. (2020). Patologías de mucosa oral en niños de 4 a 12 años (Bachelor’s thesis, Quito: UCE).
- López, M. D. R., Vila, P. G., & Torreira, M. G. (2021). Patologías de la mucosa oral más frecuentes en la edad pediátrica. Revista de Odontopediatría Latinoamericana, 11(Suplemento).
- Morones, D. G., Rosas, M. P., Villalba, M. N., Becerra, A. E. S., & Salvio, J. M. L. (2021). Herpes intraoral recidivante. Revista Mexicana de Periodontología, 12(1-3), 30-33.
- Corsino, C. B., Ali, R., & Linklater, D. R. (2018). Herpangina.
- Apriasari, M. L., & Utami, J. P. (2020). Management of Herpangina. DENTA, 14(2), 77-81.
- Cabrera Escobar, D., Ramos Plasencia, A., & Espinosa González, L. (2018). Enfermedad boca mano pie. Presentación de un caso. Medisur, 16(3), 469-474.
- Laurencio Vallina, S. C., Álvarez Caballero, M., & Hernández Lin, T. (2019). Enfermedad de boca, mano, pie en un lactante. MediSan, 23(1), 106-113.
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








