Oral Candidiasis in Children: Symptoms, Causes and Treatment


Written and verified by the dermatologist Maria del Carmen Hernandez
Oral candidiasis in children – or thrush – is a common opportunistic infection of the oral cavity due to an overgrowth of Candida species of fungus, the most common being Candida Albicans. The incidence varies according to age and certain predisposing factors. It most frequently affects infants under 6 months of age and newborns.
Causes of oral candidiasis in children
Certain microorganisms (bacteria, fungi, etc.) live regularly in the body. Some of them are harmless, but others can trigger an infection.
Since the immune system of children and infants has yet to fully develop, they’re more prone to infections from fungi that live regularly in the body. Risk factors include the following:
- Impaired salivary gland function
- Medications (certain antibiotics or corticosteroids)
- Dentures
- High carbohydrate diet and extreme life situations
- Smoking
- Diabetes mellitus
- Cushing’s syndrome
- Malignant neoplasms
- Immunosuppressive conditions, the elderly, and newborns
The classification of candidiasis
When the yeast Candida Albicans develops and proliferates excessively in the oral cavity, we often refer to the lesions as “thrush.” According to studies that appeared in Dermatologic Therapy, the classification of oral candidiasis, according to evolution or location, is as follows:
- Acute candidiasis: Subdivided into its pseudomembranous and erythematous forms
- Chronic candidiasis: Pseudomembranous, erythematous (atrophic), and hyperplastic forms
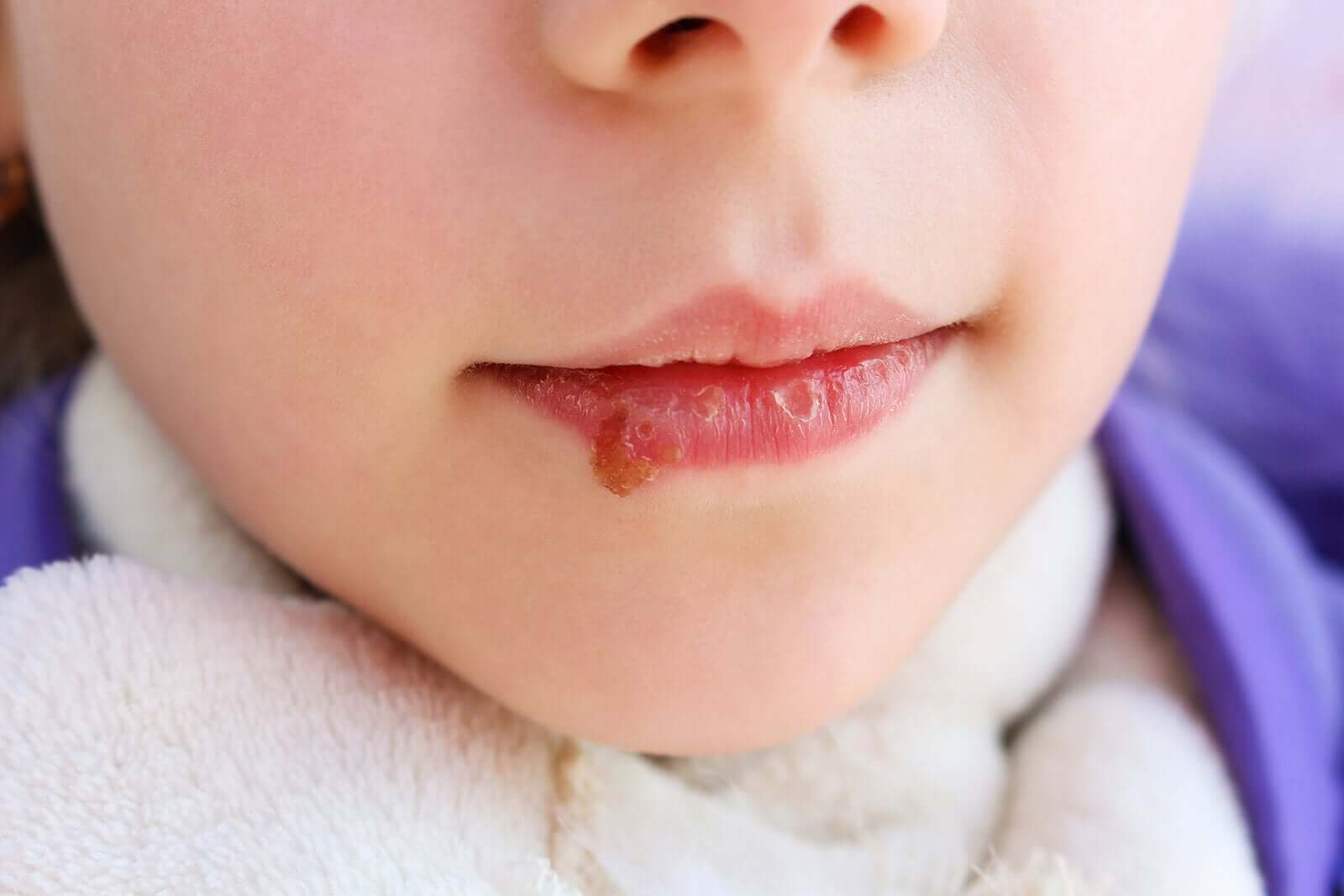
- Angular cheilitis: Or infectious angular cheilitis, which are cold sores at the corner of the lips
Symptoms and signs of oral candidiasis
The clinical picture that Candida yeast infections trigger can be similar to other health problems. Symptoms of oral thrush include the following:
- Odynophagia (sore throat)
- Dysphagia (pain when swallowing)
- Halitosis or loss of taste and appetite
- Bleeding when rubbing the lesions
- White, velvety lesions on the tongue and mouth
There are usually no symptoms of general discomfort or seriousness. In fact, in some cases, there are no symptoms and the lesions are painless.
You may be interested in: Contagious Diseases that Spread in Daycare Centers
Diagnosis of candidiasis in children
A medical specialist will carry out the diagnosis of candidiasis in children. Here, the professional will question the child or the mother to investigate possible predisposing factors and health history. The clinical findings in the patient will complement the answers to the questions and both will contribute to the making of a definitive diagnosis.
In cases in which there are certain doubts at the moment of making and defining a diagnosis, the doctor may perform a scraping of the lesion to analyze under a microscope. There are even more serious cases in which candidiasis spreads to regions of the esophagus. Consequently, the doctor must do a culture of the affected tissue to study the microbe that produced it.
What are the therapeutic options?
An important part of the treatment of candidiasis in children is proper mouth rinsing. That’s to say, patients who are in good health will recover more easily than those who have an underlying illness.
Antifungals are the medications used for the treatment of candidiasis. Also, the specific type of antifungal will depend on the location of the lesion in the body (nystatin, clotrimazole, fluconazole, miconazole, amphotericin B).
In mild cases of oral candidiasis in children, doctors prescribe appropriate oral medication, whether tablets, pills or capsules. In turn, children should consume yogurt or ingest probiotics such as Lactobacillus that reduce the growth of Candida Albicans and prevent infections, according to published studies in the medical journal Micosis.
Tips to prevent future outbreaks of candidiasis
It’s important to know that there’s a high likelihood of future outbreaks of candidiasis if the cause wasn’t addressed correctly and efficiently. Therefore, the best way to treat thrush and prevent recurrent infections is to address the underlying cause.

Some of the following recommendations help to avoid new episodes over time:
- Maintain proper oral hygiene: Don’t share toothbrushes, and replace them on a regular basis. Perform proper oral hygiene every day.
- Disinfect items: Disinfect bottles, pacifiers and utensils that are commonly used by infants and children.
- Mouth rinses: Perform mouth rinses to ensure the cleanliness of the oral cavity. One of the options to do this is with mouthwashes with warm saltwater.
Prognosis of oral candidiasis in children
As we’ve mentioned, candidiasis in children may develop without symptoms or signs. However, when lesions are present and treatment begins, it usually goes away within 2 weeks. However, in children with weakened immune systems, treatment processes take longer and require more care.
Oral candidiasis in children – or thrush – is a common opportunistic infection of the oral cavity due to an overgrowth of Candida species of fungus, the most common being Candida Albicans. The incidence varies according to age and certain predisposing factors. It most frequently affects infants under 6 months of age and newborns.
Causes of oral candidiasis in children
Certain microorganisms (bacteria, fungi, etc.) live regularly in the body. Some of them are harmless, but others can trigger an infection.
Since the immune system of children and infants has yet to fully develop, they’re more prone to infections from fungi that live regularly in the body. Risk factors include the following:
- Impaired salivary gland function
- Medications (certain antibiotics or corticosteroids)
- Dentures
- High carbohydrate diet and extreme life situations
- Smoking
- Diabetes mellitus
- Cushing’s syndrome
- Malignant neoplasms
- Immunosuppressive conditions, the elderly, and newborns

The classification of candidiasis
When the yeast Candida Albicans develops and proliferates excessively in the oral cavity, we often refer to the lesions as “thrush.” According to studies that appeared in Dermatologic Therapy, the classification of oral candidiasis, according to evolution or location, is as follows:
- Acute candidiasis: Subdivided into its pseudomembranous and erythematous forms
- Chronic candidiasis: Pseudomembranous, erythematous (atrophic), and hyperplastic forms
- Angular cheilitis: Or infectious angular cheilitis, which are cold sores at the corner of the lips
Symptoms and signs of oral candidiasis
The clinical picture that Candida yeast infections trigger can be similar to other health problems. Symptoms of oral thrush include the following:
- Odynophagia (sore throat)
- Dysphagia (pain when swallowing)
- Halitosis or loss of taste and appetite
- Bleeding when rubbing the lesions
- White, velvety lesions on the tongue and mouth
There are usually no symptoms of general discomfort or seriousness. In fact, in some cases, there are no symptoms and the lesions are painless.
You may be interested in: Contagious Diseases that Spread in Daycare Centers
Diagnosis of candidiasis in children
A medical specialist will carry out the diagnosis of candidiasis in children. Here, the professional will question the child or the mother to investigate possible predisposing factors and health history. The clinical findings in the patient will complement the answers to the questions and both will contribute to the making of a definitive diagnosis.
In cases in which there are certain doubts at the moment of making and defining a diagnosis, the doctor may perform a scraping of the lesion to analyze under a microscope. There are even more serious cases in which candidiasis spreads to regions of the esophagus. Consequently, the doctor must do a culture of the affected tissue to study the microbe that produced it.
What are the therapeutic options?
An important part of the treatment of candidiasis in children is proper mouth rinsing. That’s to say, patients who are in good health will recover more easily than those who have an underlying illness.
Antifungals are the medications used for the treatment of candidiasis. Also, the specific type of antifungal will depend on the location of the lesion in the body (nystatin, clotrimazole, fluconazole, miconazole, amphotericin B).
In mild cases of oral candidiasis in children, doctors prescribe appropriate oral medication, whether tablets, pills or capsules. In turn, children should consume yogurt or ingest probiotics such as Lactobacillus that reduce the growth of Candida Albicans and prevent infections, according to published studies in the medical journal Micosis.
Tips to prevent future outbreaks of candidiasis
It’s important to know that there’s a high likelihood of future outbreaks of candidiasis if the cause wasn’t addressed correctly and efficiently. Therefore, the best way to treat thrush and prevent recurrent infections is to address the underlying cause.

Some of the following recommendations help to avoid new episodes over time:
- Maintain proper oral hygiene: Don’t share toothbrushes, and replace them on a regular basis. Perform proper oral hygiene every day.
- Disinfect items: Disinfect bottles, pacifiers and utensils that are commonly used by infants and children.
- Mouth rinses: Perform mouth rinses to ensure the cleanliness of the oral cavity. One of the options to do this is with mouthwashes with warm saltwater.
Prognosis of oral candidiasis in children
As we’ve mentioned, candidiasis in children may develop without symptoms or signs. However, when lesions are present and treatment begins, it usually goes away within 2 weeks. However, in children with weakened immune systems, treatment processes take longer and require more care.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Berdicevsky I, Ben-Aryeh H, Szargel R, Gutman D. Oral Candida in children. Oral Surg Oral Med Oral Pathol. 1984 Jan;57(1):37-40. doi: 10.1016/0030-4220(84)90257-3. PMID: 6582432.
- Sharon V, Fazel N. Oral candidiasis and angular cheilitis. Dermatol Ther. 2010 May-Jun;23(3):230-42. doi: 10.1111/j.1529-8019.2010.01320.x. PMID: 20597942.
- PUERTO, J.L. et al. Candidiasis orofaríngea. Rev Diagn Biol [online]. 2001, vol.50, n.4 [citado 2020-12-01], pp.177-181. Disponible en: <http://scielo.isciii.es/scielo.php?script=sci_arttext&pid=S0034-79732001000400001&lng=es&nrm=iso>. ISSN 0034-7973.
- Mailänder-Sánchez D, Wagener J, Schaller M. Potential role of probiotic bacteria in the treatment and prevention of localised candidosis. Mycoses. 2012 Jan;55(1):17-26. doi: 10.1111/j.1439-0507.2010.01967.x. Epub 2011 Jun 14. PMID: 21672043.
- Fang J, Huang B, Ding Z. Efficacy of antifungal drugs in the treatment of oral candidiasis: A Bayesian network meta-analysis. J Prosthet Dent. 2020 Mar 10:S0022-3913(20)30076-7. doi: 10.1016/j.prosdent.2019.12.025. Epub ahead of print. PMID: 32165010.
- Martins N, Ferreira IC, Barros L, Silva S, Henriques M. Candidiasis: predisposing factors, prevention, diagnosis and alternative treatment. Mycopathologia. 2014 Jun;177(5-6):223-40. doi: 10.1007/s11046-014-9749-1. Epub 2014 May 1. PMID: 24789109.
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








