The Treatment of Cleft Lip

You’ve probably heard of cleft lip at some point, but today, we want to tell you about the treatment of cleft lip. While it’s an unavoidable health condition, there are many ways to help babies that are born with it.
Cleft lip and palate are not purely cosmetic issues. They also interfere with the baby’s feeding, language, and teething. In addition, they predispose you to suffer from certain ear problems.
Taking charge of the situation in a timely manner makes a difference in the quality of life of the child and their family. Keep reading this article and find out how to proceed in these cases.
What is cleft lip?
Cleft lip and cleft palate are two congenital skull-facial malformations. That is, they occur inside the mother’s womb when the bones and soft parts of the baby’s nose and mouth fuse to form the palate and upper lip. If they fail to join completely, a cleft is left on the lip, palate, or both.
This defect can manifest itself in several ways, depending on the affected tissues:
- A small cleft in the lip.
- A wider cleft, extending from the lip to the nose.
- A cleft in the palate, anterior (hard palate), posterior (soft palate), or complete, on one or both sides.
The specific cause that generates this problem is unknown, although experts have identified several associated factors. For example, the consumption of certain drugs and pharmaceuticals by parents, exposure to toxins, contact with certain viruses, and of course, genetic predisposition.

The treatment of cleft lip
The diagnosis of cleft lip and palate takes place at the time of the baby’s birth, through a physical examination of the mouth, nose, and palate.
Thanks to technological advances in obstetric ultrasound, prenatal diagnosis is often performed. This means a great advantage for the child, as it allows doctors and parents to plan in advance the approach to this problem.
An important aspect of this condition is that it requires interdisciplinary care, as it involves various aspects and functions of the child’s body. For this reason, the experience of the different disciplines is needed to guarantee the best health prognosis.
In general, the therapeutic team consists of pediatricians, maxillofacial surgeons, otorhinolaryngologists, pediatric dentists, speech therapists, audiologists, and psychologists. In some cases, the intervention of geneticists and social workers may also be necessary.
Cleft lip treatment can be divided into two main stages. The first is characterized by the surgical interventions necessary to close the fissures. The second includes the rest of the treatments and rehabilitation therapies of the different functions of the child.
Surgical treatment
The objective of the surgery is to close the fissures and, in general, it takes place in several stages or surgical times:
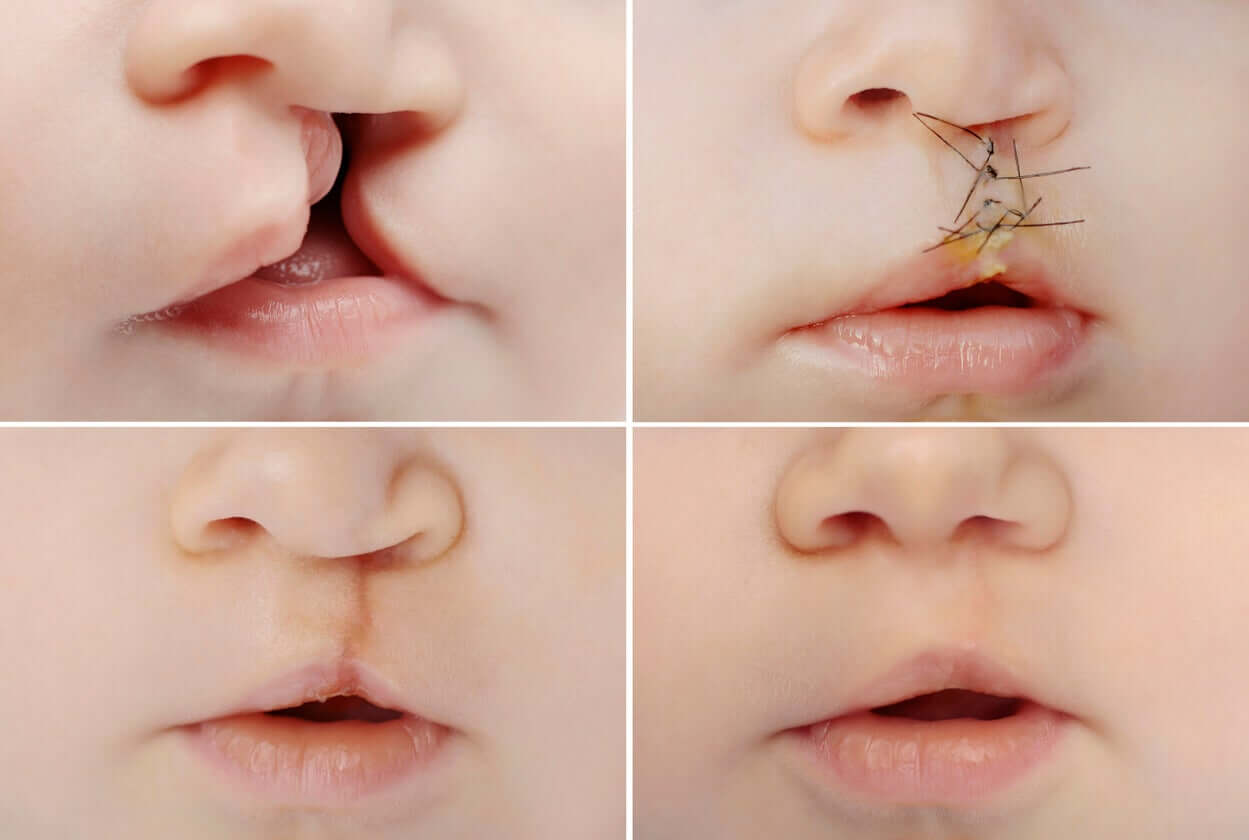
- The first operation consists of the resolution of the lip cleft and is called cheiloplasty. It usually takes place before the first birthday and requires general anesthesia in the operating room. Closing the cleft lip improves the shape of the upper lip and nose and often leaves a small scar.
- If the child also has a cleft palate, then doctors perform a second surgery called a palothoplasty. It takes place between 12 and 18 months of age, before the little one begins to speak. In this procedure, the palate defect is closed to prevent food from going to the nose.
- In some cases, new tissue retouching interventions are required, either to improve certain functions or the patient’s appearance.
Other treatments
Although surgical treatment is essential to correct the defect, it’s not enough to restore the normal functions of the child’s mouth. For this reason, it’s important to complement it with the approach of other specialized disciplines on the subject. Here are some of them:
- Childcare: Children with cleft lip and palate can be breastfed and this is what experts recommend the most. The mother must receive the support and education necessary to feed her baby correctly.
- Temporary prostheses: When there are palatal clefts, placing prosthetic plates is necessary in order to prevent the passage of food into the nose. This is indicated until the time of surgery.
- Dentistry and orthodontics: Monitor the development of the jaws and tooth eruption is necessary. The use of orthodontic appliances is often indicated to guide bone growth and reposition teeth.
- Speech Therapy: Due to the defect in the palate and lip, some patients have difficulty speaking. Speech therapy treatments and exercises will be necessary to resolve these complications.
- Hearing checks: Ear infections are very common in children with cleft palates and, therefore, they need to have regular check-ups with the audiologist or ENT specialist.
- Psychology: Assuming and accepting this type of visible malformation can be difficult, both for the child and for their family. Psychological support can provide them with useful tools to cope with this condition.
The benefits will come in time
An early approach with an experienced professional team is key to providing the best health conditions for these children. Most youngsters respond successfully to treatments, although these require time, interventions, and patience.
It pays to be consistent! Because, after a few years, the cleft lip will be just an anecdote from our little one’s childhood.
You’ve probably heard of cleft lip at some point, but today, we want to tell you about the treatment of cleft lip. While it’s an unavoidable health condition, there are many ways to help babies that are born with it.
Cleft lip and palate are not purely cosmetic issues. They also interfere with the baby’s feeding, language, and teething. In addition, they predispose you to suffer from certain ear problems.
Taking charge of the situation in a timely manner makes a difference in the quality of life of the child and their family. Keep reading this article and find out how to proceed in these cases.
What is cleft lip?
Cleft lip and cleft palate are two congenital skull-facial malformations. That is, they occur inside the mother’s womb when the bones and soft parts of the baby’s nose and mouth fuse to form the palate and upper lip. If they fail to join completely, a cleft is left on the lip, palate, or both.
This defect can manifest itself in several ways, depending on the affected tissues:
- A small cleft in the lip.
- A wider cleft, extending from the lip to the nose.
- A cleft in the palate, anterior (hard palate), posterior (soft palate), or complete, on one or both sides.
The specific cause that generates this problem is unknown, although experts have identified several associated factors. For example, the consumption of certain drugs and pharmaceuticals by parents, exposure to toxins, contact with certain viruses, and of course, genetic predisposition.

The treatment of cleft lip
The diagnosis of cleft lip and palate takes place at the time of the baby’s birth, through a physical examination of the mouth, nose, and palate.
Thanks to technological advances in obstetric ultrasound, prenatal diagnosis is often performed. This means a great advantage for the child, as it allows doctors and parents to plan in advance the approach to this problem.
An important aspect of this condition is that it requires interdisciplinary care, as it involves various aspects and functions of the child’s body. For this reason, the experience of the different disciplines is needed to guarantee the best health prognosis.
In general, the therapeutic team consists of pediatricians, maxillofacial surgeons, otorhinolaryngologists, pediatric dentists, speech therapists, audiologists, and psychologists. In some cases, the intervention of geneticists and social workers may also be necessary.
Cleft lip treatment can be divided into two main stages. The first is characterized by the surgical interventions necessary to close the fissures. The second includes the rest of the treatments and rehabilitation therapies of the different functions of the child.
Surgical treatment
The objective of the surgery is to close the fissures and, in general, it takes place in several stages or surgical times:
- The first operation consists of the resolution of the lip cleft and is called cheiloplasty. It usually takes place before the first birthday and requires general anesthesia in the operating room. Closing the cleft lip improves the shape of the upper lip and nose and often leaves a small scar.
- If the child also has a cleft palate, then doctors perform a second surgery called a palothoplasty. It takes place between 12 and 18 months of age, before the little one begins to speak. In this procedure, the palate defect is closed to prevent food from going to the nose.
- In some cases, new tissue retouching interventions are required, either to improve certain functions or the patient’s appearance.
Other treatments
Although surgical treatment is essential to correct the defect, it’s not enough to restore the normal functions of the child’s mouth. For this reason, it’s important to complement it with the approach of other specialized disciplines on the subject. Here are some of them:
- Childcare: Children with cleft lip and palate can be breastfed and this is what experts recommend the most. The mother must receive the support and education necessary to feed her baby correctly.
- Temporary prostheses: When there are palatal clefts, placing prosthetic plates is necessary in order to prevent the passage of food into the nose. This is indicated until the time of surgery.
- Dentistry and orthodontics: Monitor the development of the jaws and tooth eruption is necessary. The use of orthodontic appliances is often indicated to guide bone growth and reposition teeth.
- Speech Therapy: Due to the defect in the palate and lip, some patients have difficulty speaking. Speech therapy treatments and exercises will be necessary to resolve these complications.
- Hearing checks: Ear infections are very common in children with cleft palates and, therefore, they need to have regular check-ups with the audiologist or ENT specialist.
- Psychology: Assuming and accepting this type of visible malformation can be difficult, both for the child and for their family. Psychological support can provide them with useful tools to cope with this condition.

The benefits will come in time
An early approach with an experienced professional team is key to providing the best health conditions for these children. Most youngsters respond successfully to treatments, although these require time, interventions, and patience.
It pays to be consistent! Because, after a few years, the cleft lip will be just an anecdote from our little one’s childhood.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Plasencia-Dueñas, E. A., Díaz-Vélez, C. & Dueñas-Roque, M. M. (2020). Factores asociados a la presencia de fisura labiopalatina en recién nacidos en un hospital peruano de tercer nivel de atención. Un estudio de casos y controles. Acta Médica Peruana, 37(3), 304-311.
- Leiva, N., Stange, C., Ayala, F. & Fuentes, V. (2018). Clasificación anatómica: una propuesta para categorizar las fisuras labiopalatinas. Odontología sanmarquina, 22(3), 245-249.
- Cabello Gómez, E. (2021). Alimentación en los niños con fisura labiopalatina. Estudio de 31 casos.
- Gamarra Esteban, P. (2021). Protocolo del paciente con fisura labio-palatina congénita.
- Mogrovejo, E. (2017). La importancia de las placas palatinas en recién nacidos con labio y paladar hendido. Revista científica digital INSPILIP Código ISSN, 2588, 0551.
- Villagra, N. L., Layera, L. S. & Parada, R. P. (2017). Tratamiento odontológico multidisciplinario de un paciente complejo con fisura labiopalatina bilateral. Odontología sanmarquina, 20(2), 95-100.
- Worley, M. L., Patel, K. G. & Kilpatrick, L. A. (2018). Cleft lip and palate. Clinics in perinatology, 45(4), 661-678.
- Gatti, G. L., Freda, N., Giacomina, A., Montemagni, M. & Sisti, A. (2017). Cleft lip and palate repair. Journal of craniofacial surgery, 28(8), 1918-1924.
- Dogan, E., Dogan, E. I. & Dogan, S. (2019). Interdisciplinary treatment approaches for cleft lip and palate patients to obtain esthetic and functional results. Journal of Dentistry and Oral Hygiene, 11(1), 1-5.
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








