White Spots on Children's Skin
White spots on children’s skin can be due to many causes. While some of them are completely harmless, others can be detrimental to their well-being. We’ll tell you everything you need to know about them and how to identify them.
If your child has white spots on their skin, it’s normal to worry. However, not all the white spots that appear on the skin should be cause for concern.
In the following article, we’ll teach you to differentiate those spots that will only pose a mere aesthetic problem from those that should be treated immediately by a dermatologist. Of course, the latter are those that will require specific treatment.
White spots on children’s skin that need treatment and care
Certain white spots on children’s skin are a sign of a more serious disease or condition. The conditions that are frequently related to them are the following:
Yeast infection
The white spots on the skin caused by fungi are usually raised at the edges and are lighter in color in the center. This makes them easy to diagnose, even for people who aren’t specialists.
When the skin becomes infected by fungi, they spread throughout the epidermis – the outer layer of the skin. In this process, they can gradually make the skin lose its natural color.
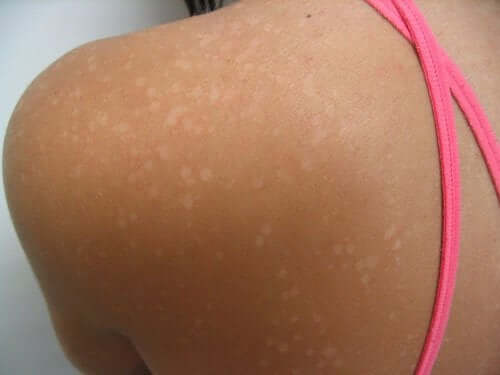
In case you observe this type of spots on your skin or that of your child, it’s very important that you go to the doctor and follow their recommendations. Fungi are very contagious and, if they’re not remedied, they’ll progressively spread over your skin. The affected regions can be very itchy and quite annoying.
Fungi, as well as other agents such as viruses and bacteria, are everywhere. However, it’s during the summer when they’re usually most active.
This is due to the fact that children and adults frequently walk barefoot in public places such as swimming pools or showers, in addition to borrowing and exchanging towels, flip-flops, or any other personal object many times.
Fortunately, these infections usually go away with the use of antifungal creams or shampoos, depending on the affected area. However, it’s always best to go to the doctor to obtain an accurate diagnosis and receive the appropriate treatment.
“Yeast infections on the skin can cause white patches”
Vitiligo
Vitiligo is a disease in which the body itself attacks melanocytes. In other words, the cells that give color to the skin. When the melanocytes are destroyed, the affected area turns completely white.
Vitiligo doesn’t itch nor do the spots have raised edges like fungal spots. However, the spots are whiter than any other skin condition. For this reason, they can be easily identified.
The treatment of this condition is very complex and requires continuous medical monitoring. In many cases, it’s not possible to achieve the remission of the spots, although they can be disguised and become less evident. In these cases, it’s important to instill healthy-self esteem in the child so they can accept their condition. It’s also important to educate those around them about the nature of vitiligo and the fact that it’s not contagious or life-threatening.
Psoriasis
Psoriasis is a multifactorial disease that affects up to 3% of the world population according to some studies. It’s an inflammatory pathology that affects the superficial layer of the skin and causes it to flake.
The clinical manifestations in children are very similar to those in adults. In this sense, a white or red scaly plaque is observed, which produces itching. Plaques are most often located on the scalp, face, knees, and elbows.
As it’s a chronic disease, psoriasis management is aimed at controlling flare-ups. A specialist doctor may indicate the use of moisturizing creams or lotions with corticosteroids to reduce inflammation and itching. They may also recommend the use of certain oral medications or even light therapy.
White spots on children’s skin that aren’t a cause for concern
There are white spots on children’s skin that shouldn’t alarm adults. These may disappear with time or remain for life, but they don’t represent anything more than the imprint they form on the skin.
White birthmarks or moles
Birthmarks and moles don’t go away nor are they treated; They don’t itch, they’re not symptoms of any disease, nor do they spread on the skin. They’re part, let’s say, of the identity of each individual.
Pityriasis alba
Pityriasis alba is a consequence of atopic dermatitis or the sensitivity of the skin to environmental aggressions. As with birthmarks, they’re nothing more than an aesthetic concern.
This skin condition manifests itself with the appearance of white spots —sometimes a little more pinkish—, oval-shaped or round, that have a scaly consistency and are dry to the touch. They usually appear in summer, when the sun’s rays attack the skin much more and minors are more exposed.
Any child can present pityriasis alba, however, the Spanish Association of Pediatrics states that it’s most common between 3 and 16 years of age. Despite the absence of a specific treatment, the spots disappear on their own after a few months.
“The beach during summer vacation is the ideal setting for a child’s skin to become brown and, therefore, the spots are more visible”
Scars
Scratches, wounds, or mosquito bites can be the reason for the appearance of white spots on the skin. Many times children, without realizing it, scratch and cause a scab, which, when healed, becomes a white spot.
Many of them don’t disappear over time because, when the skin rebuilds, it simply doesn’t regain the same color as the rest. Like birthmarks, they shouldn’t be of concern to parents.

White spots on the skin of children, how to avoid them?
While some white spots on children’s skin can’t be avoided, there are others that can be prevented by taking certain precautions. Therefore, we’ll leave you some tips that you should keep in mind, especially in summer:
- Make sure your child puts on sunscreen.
- Don’t allow them to be exposed to the sun during the afternoon hours when the radiation is most intense. In these hours, try to remain in the shade.
- Make them wear hats and sunglasses.
- Make sure they wear fine-knit shirts that cover her arms. Clothing with sun protection is also very beneficial.
- Make sure they always stay hydrated, drink plenty of water, and eat fruits.
Don’t forget that taking care of your child’s skin is equivalent to taking care of their health, so prevention is a fundamental tool. In the long run, they’ll thank you for it.
White spots on children’s skin can be due to many causes. While some of them are completely harmless, others can be detrimental to their well-being. We’ll tell you everything you need to know about them and how to identify them.
If your child has white spots on their skin, it’s normal to worry. However, not all the white spots that appear on the skin should be cause for concern.
In the following article, we’ll teach you to differentiate those spots that will only pose a mere aesthetic problem from those that should be treated immediately by a dermatologist. Of course, the latter are those that will require specific treatment.
White spots on children’s skin that need treatment and care
Certain white spots on children’s skin are a sign of a more serious disease or condition. The conditions that are frequently related to them are the following:
Yeast infection
The white spots on the skin caused by fungi are usually raised at the edges and are lighter in color in the center. This makes them easy to diagnose, even for people who aren’t specialists.
When the skin becomes infected by fungi, they spread throughout the epidermis – the outer layer of the skin. In this process, they can gradually make the skin lose its natural color.

In case you observe this type of spots on your skin or that of your child, it’s very important that you go to the doctor and follow their recommendations. Fungi are very contagious and, if they’re not remedied, they’ll progressively spread over your skin. The affected regions can be very itchy and quite annoying.
Fungi, as well as other agents such as viruses and bacteria, are everywhere. However, it’s during the summer when they’re usually most active.
This is due to the fact that children and adults frequently walk barefoot in public places such as swimming pools or showers, in addition to borrowing and exchanging towels, flip-flops, or any other personal object many times.
Fortunately, these infections usually go away with the use of antifungal creams or shampoos, depending on the affected area. However, it’s always best to go to the doctor to obtain an accurate diagnosis and receive the appropriate treatment.
“Yeast infections on the skin can cause white patches”
Vitiligo
Vitiligo is a disease in which the body itself attacks melanocytes. In other words, the cells that give color to the skin. When the melanocytes are destroyed, the affected area turns completely white.
Vitiligo doesn’t itch nor do the spots have raised edges like fungal spots. However, the spots are whiter than any other skin condition. For this reason, they can be easily identified.
The treatment of this condition is very complex and requires continuous medical monitoring. In many cases, it’s not possible to achieve the remission of the spots, although they can be disguised and become less evident. In these cases, it’s important to instill healthy-self esteem in the child so they can accept their condition. It’s also important to educate those around them about the nature of vitiligo and the fact that it’s not contagious or life-threatening.
Psoriasis
Psoriasis is a multifactorial disease that affects up to 3% of the world population according to some studies. It’s an inflammatory pathology that affects the superficial layer of the skin and causes it to flake.
The clinical manifestations in children are very similar to those in adults. In this sense, a white or red scaly plaque is observed, which produces itching. Plaques are most often located on the scalp, face, knees, and elbows.
As it’s a chronic disease, psoriasis management is aimed at controlling flare-ups. A specialist doctor may indicate the use of moisturizing creams or lotions with corticosteroids to reduce inflammation and itching. They may also recommend the use of certain oral medications or even light therapy.
White spots on children’s skin that aren’t a cause for concern
There are white spots on children’s skin that shouldn’t alarm adults. These may disappear with time or remain for life, but they don’t represent anything more than the imprint they form on the skin.
White birthmarks or moles
Birthmarks and moles don’t go away nor are they treated; They don’t itch, they’re not symptoms of any disease, nor do they spread on the skin. They’re part, let’s say, of the identity of each individual.
Pityriasis alba
Pityriasis alba is a consequence of atopic dermatitis or the sensitivity of the skin to environmental aggressions. As with birthmarks, they’re nothing more than an aesthetic concern.
This skin condition manifests itself with the appearance of white spots —sometimes a little more pinkish—, oval-shaped or round, that have a scaly consistency and are dry to the touch. They usually appear in summer, when the sun’s rays attack the skin much more and minors are more exposed.
Any child can present pityriasis alba, however, the Spanish Association of Pediatrics states that it’s most common between 3 and 16 years of age. Despite the absence of a specific treatment, the spots disappear on their own after a few months.
“The beach during summer vacation is the ideal setting for a child’s skin to become brown and, therefore, the spots are more visible”
Scars
Scratches, wounds, or mosquito bites can be the reason for the appearance of white spots on the skin. Many times children, without realizing it, scratch and cause a scab, which, when healed, becomes a white spot.
Many of them don’t disappear over time because, when the skin rebuilds, it simply doesn’t regain the same color as the rest. Like birthmarks, they shouldn’t be of concern to parents.

White spots on the skin of children, how to avoid them?
While some white spots on children’s skin can’t be avoided, there are others that can be prevented by taking certain precautions. Therefore, we’ll leave you some tips that you should keep in mind, especially in summer:
- Make sure your child puts on sunscreen.
- Don’t allow them to be exposed to the sun during the afternoon hours when the radiation is most intense. In these hours, try to remain in the shade.
- Make them wear hats and sunglasses.
- Make sure they wear fine-knit shirts that cover her arms. Clothing with sun protection is also very beneficial.
- Make sure they always stay hydrated, drink plenty of water, and eat fruits.
Don’t forget that taking care of your child’s skin is equivalent to taking care of their health, so prevention is a fundamental tool. In the long run, they’ll thank you for it.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Ahmed, N. y Masood, S. (2022). Vitiligo. StatPearls. Consultado el 15 de febrero de 2023. Disponible en: https://www.ncbi.nlm.nih.gov/books/NBK559149/
- Arranz, M. y Hernández, A. (2019). Pitiriasis (tiña) versicolor. Asociación Española de Pediatría de Atención Primaria. Consultado el 31 de octubre de 2017. Disponible en: https://www.guia-abe.es/temas-clinicos-pitiriasis-versicolor
- Fernández, J., Gómez, X., Buti, M., et al. (2019). Características epidemiológicas de la psoriasis. Un estudio poblacional. Actas Dermo-Sifiliográficas, 110(5), 385-392. Disponible en: https://www.sciencedirect.com/science/article/abs/pii/S0001731018305350
- Instituto Nacional de Artritis y Enfermedades Musculoesqueléticas y de la Piel. (s.f.). Vitíligo. Consultado el 15 de febrero de 2023. Disponible en: https://www.niams.nih.gov/es/informacion-de-salud/vitiligo
- Karray, M. & McKinney, W. (2021). Tinea versicolor. StatPearls. Consultado el 15 de febrero de 2023. Disponible en: https://www.ncbi.nlm.nih.gov/books/NBK482500/#:~:text=Pityriasis%20versicolor%2C%20also%20known%20as%20tinea%20versicolor%2C%20is%20a%20frequent,or%20hypopigmented%20finely%20scaly%20macules.
- MedlinePlus. (s.f.). Pitiriasis alba. Consultado el 31 de octubre de 2017. Disponible en: https://medlineplus.gov/spanish/ency/article/001463.htm.
- Mayo Clinic. (2022, 4 de mayo). Pitiriasis versicolor. Consultado el 10 febrero de 2023. Disponible en: https://www.mayoclinic.org/es-es/diseases-conditions/tinea-versicolor/symptoms-causes/syc-20378385.
- Nair, P. & Badri, T. (2022). Psoriasis. StatPearls. Consultado el 15 de febrero de 2023. Disponible en:https://www.ncbi.nlm.nih.gov/books/NBK448194/
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








