Cold Sores During Pregnancy: What You Need to Know

Written and verified by the dermatologist Maria del Carmen Hernandez
Cold sores during pregnancy can be very annoying and painful, and they can also become more frequent.
Fortunately, this infection in the mouth of the pregnant woman doesn’t usually have an impact on the development or growth of the baby in the womb. Even so, it’s important to take a series of precautions during birth in order to avoid the contagion of the newborn. We’ll tell you everything you need to know.
What is herpes?
Herpes is a mucocutaneous infection caused by the herpes simplex virus (HSV) of any type. In general, HSV-1 causes cold sores, while HSV-2 causes genital herpes.
After the first infection, the virus remains in a latent state within local neurons. But under certain circumstances, such as a decrease in defenses, it sprouts again and causes the same injuries in the same places.
If you’ve never had a cold sore, you can only get it through direct contact with the bodily fluids of someone who carries the virus. The most common routes of infection are the following:
- Kisses
- Shared utensils, makeup, or food
- Oral sex
The herpes virus is very contagious, but it doesn’t usually affect the baby in the womb. However, it can be passed to the baby during labor under certain circumstances.
In general, the contagion stage culminates when a scab forms over the lesions, at which point they begin to heal and the virus goes into dormancy.
Also read: Why Do I Have Itchy Skin during Pregnancy?
Manifestations of cold sores during pregnancy
If the cold sore has already appeared on the skin, this indicates that the virus is in the body (in a latent state) and that it can reappear in situations of stress or hormonal alterations. About 50% of the population contracts it before the age of 6.
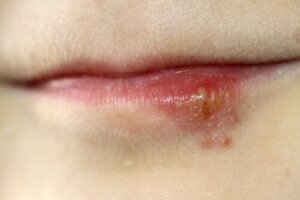
In general, a cold sore is a localized infection that tends to manifest itself in some region around the mouth. The natural history of the disease can be summarized in the following stages:
- Prodrome: Before the vesicles appear, there’s itching, burning, and tingling in the area of the injury.
- Active infection: Within a few hours, tiny, bouquet-shaped vesicles appear on the vermilion of the lip or at the corner of the mouth. They may drain a serous fluid, which contains viral particles.
- Resolution: After 15 days, the vesicles disappear and crusts form that fall off on their own.
The consequences of the presence of cold sores in the developing baby
When there’s a recurrent cold sore outbreak (that is, the infection isn’t first acquired during pregnancy) it’s likely that there will be no impact on the growth of the baby. In general, as it’s a localized infection, the virus doesn’t cross the placenta and doesn’t reach the baby.
In contrast, when the virus is contracted for the first time during pregnancy, the situation is quite different. The mother’s body hasn’t yet generated any antibodies against this infectious agent and then, it’s possible to infect the fetus.
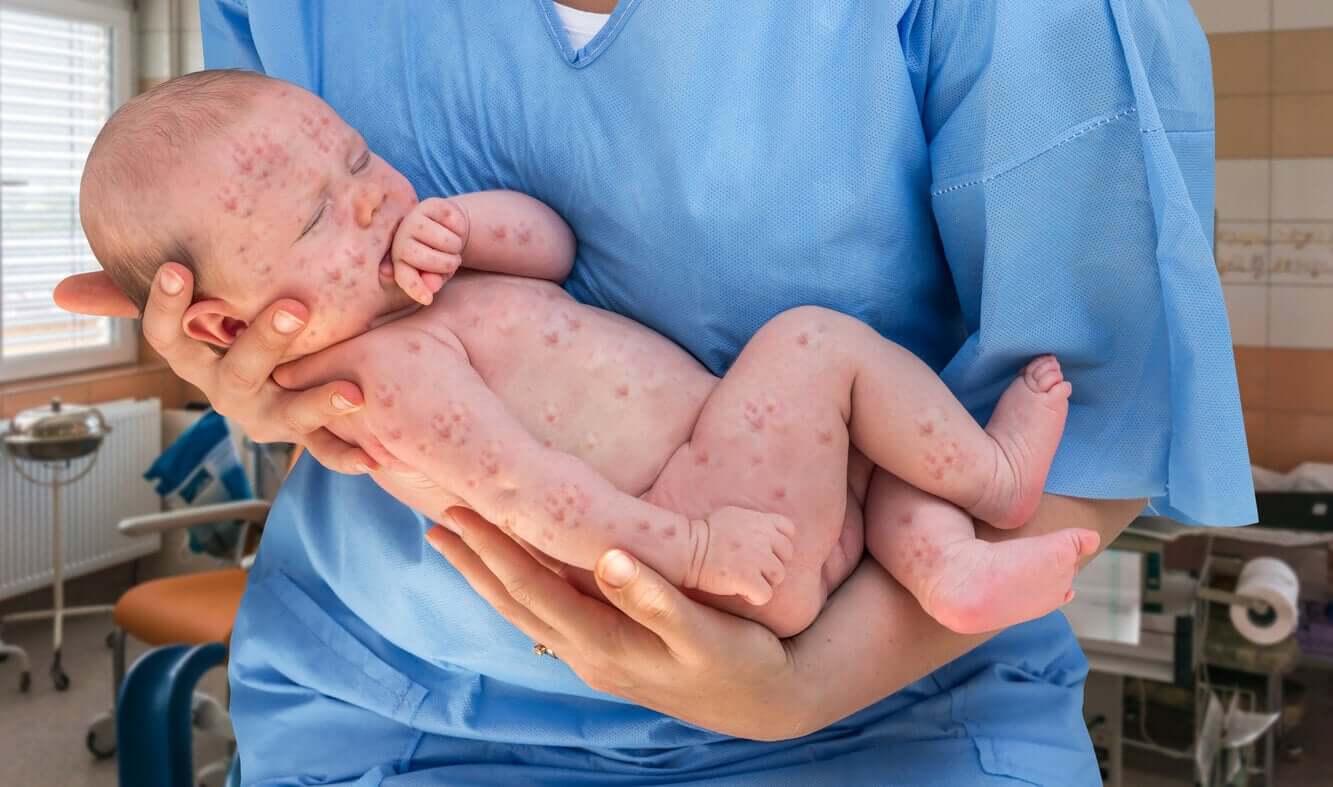
Herpes acquired at birth (or congenital herpes) is a potentially serious disease and the risk of contracting it is greater when the mother acquires the virus in the third trimester of pregnancy. Especially the genital variant, because at the time of delivery, the baby can be infected by direct contact with the infected mucosa.
You may be interested: Oily Skin During Pregnancy: Advice and Care
The prevention and treatment of cold sores during pregnancy
The most common treatment option for cold sores is an over-the-counter topical cream, made up of an antiviral medication. In general, cold sores are more of a nuisance to the pregnant woman than a risk to the developing baby.
If the cold sore occurs in the third trimester of pregnancy, or if the virus is contracted for the first time during this period, the doctor will need to prescribe certain treatments. They may even indicate cesarean delivery.
The pregnant woman who has acquired the virus in the last stage of pregnancy can prevent transmission and contagion to her baby through the following measures:
- Ensure proper hand-washing as one of the most important hygienic measures.
- Carry out monthly or fortnightly serological controls.
- After delivery, take extreme care and hygiene measures.

Is a cesarean section recommended for herpes?
The doctor’s indication to carry out this type of delivery will depend on the exact moment in which the infection occurred.
- If the mother contracted HSV before pregnancy or before the third trimester and has no symptoms, she can give birth naturally. This is because it’s assumed that she had enough time to develop antibodies and pass them on to the baby.
- On the contrary, if the pregnant woman presents symptoms for the first time in the stage close to delivery, a cesarean section should be performed.
The importance of recognizing symptoms during pregnancy
In conclusion, it’s quite common for women to experience cold sores during pregnancy, even if they haven’t had them for a long time.
Therefore, it’s important to know and learn about the behavior of this virus and its transmission method in order to avoid accidental infections that may affect the baby.
Cold sores during pregnancy can be very annoying and painful, and they can also become more frequent.
Fortunately, this infection in the mouth of the pregnant woman doesn’t usually have an impact on the development or growth of the baby in the womb. Even so, it’s important to take a series of precautions during birth in order to avoid the contagion of the newborn. We’ll tell you everything you need to know.
What is herpes?
Herpes is a mucocutaneous infection caused by the herpes simplex virus (HSV) of any type. In general, HSV-1 causes cold sores, while HSV-2 causes genital herpes.
After the first infection, the virus remains in a latent state within local neurons. But under certain circumstances, such as a decrease in defenses, it sprouts again and causes the same injuries in the same places.
If you’ve never had a cold sore, you can only get it through direct contact with the bodily fluids of someone who carries the virus. The most common routes of infection are the following:
- Kisses
- Shared utensils, makeup, or food
- Oral sex
The herpes virus is very contagious, but it doesn’t usually affect the baby in the womb. However, it can be passed to the baby during labor under certain circumstances.
In general, the contagion stage culminates when a scab forms over the lesions, at which point they begin to heal and the virus goes into dormancy.

Also read: Why Do I Have Itchy Skin during Pregnancy?
Manifestations of cold sores during pregnancy
If the cold sore has already appeared on the skin, this indicates that the virus is in the body (in a latent state) and that it can reappear in situations of stress or hormonal alterations. About 50% of the population contracts it before the age of 6.
In general, a cold sore is a localized infection that tends to manifest itself in some region around the mouth. The natural history of the disease can be summarized in the following stages:
- Prodrome: Before the vesicles appear, there’s itching, burning, and tingling in the area of the injury.
- Active infection: Within a few hours, tiny, bouquet-shaped vesicles appear on the vermilion of the lip or at the corner of the mouth. They may drain a serous fluid, which contains viral particles.
- Resolution: After 15 days, the vesicles disappear and crusts form that fall off on their own.
The consequences of the presence of cold sores in the developing baby
When there’s a recurrent cold sore outbreak (that is, the infection isn’t first acquired during pregnancy) it’s likely that there will be no impact on the growth of the baby. In general, as it’s a localized infection, the virus doesn’t cross the placenta and doesn’t reach the baby.
In contrast, when the virus is contracted for the first time during pregnancy, the situation is quite different. The mother’s body hasn’t yet generated any antibodies against this infectious agent and then, it’s possible to infect the fetus.
Herpes acquired at birth (or congenital herpes) is a potentially serious disease and the risk of contracting it is greater when the mother acquires the virus in the third trimester of pregnancy. Especially the genital variant, because at the time of delivery, the baby can be infected by direct contact with the infected mucosa.
You may be interested: Oily Skin During Pregnancy: Advice and Care
The prevention and treatment of cold sores during pregnancy
The most common treatment option for cold sores is an over-the-counter topical cream, made up of an antiviral medication. In general, cold sores are more of a nuisance to the pregnant woman than a risk to the developing baby.
If the cold sore occurs in the third trimester of pregnancy, or if the virus is contracted for the first time during this period, the doctor will need to prescribe certain treatments. They may even indicate cesarean delivery.
The pregnant woman who has acquired the virus in the last stage of pregnancy can prevent transmission and contagion to her baby through the following measures:
- Ensure proper hand-washing as one of the most important hygienic measures.
- Carry out monthly or fortnightly serological controls.
- After delivery, take extreme care and hygiene measures.

Is a cesarean section recommended for herpes?
The doctor’s indication to carry out this type of delivery will depend on the exact moment in which the infection occurred.
- If the mother contracted HSV before pregnancy or before the third trimester and has no symptoms, she can give birth naturally. This is because it’s assumed that she had enough time to develop antibodies and pass them on to the baby.
- On the contrary, if the pregnant woman presents symptoms for the first time in the stage close to delivery, a cesarean section should be performed.
The importance of recognizing symptoms during pregnancy
In conclusion, it’s quite common for women to experience cold sores during pregnancy, even if they haven’t had them for a long time.
Therefore, it’s important to know and learn about the behavior of this virus and its transmission method in order to avoid accidental infections that may affect the baby.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Wood S. Answering questions about herpes in pregnancy. J Perinat Educ. 2011;20(1):61-64. doi:10.1891/1058-1243.20.1.61. Disponible en: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3209744/
- Oral herpes simplex virus infection in pregnancy: what are the concerns? [Internet] Disponible en: https://www.cda-adc.ca/jcda/vol-75/issue-7/523.pdf
- Straface G, Selmin A, Zanardo V, De Santis M, Ercoli A, Scambia G. Herpes simplex virus infection in pregnancy. Infect Dis Obstet Gynecol. 2012;2012:385697. doi: 10.1155/2012/385697. Epub 2012 Apr 11. PMID: 22566740; PMCID: PMC3332182. Disponible en: https://pubmed.ncbi.nlm.nih.gov/22566740/
- Perozzi KJ, Zalice KK, Howard V, Skariot L. HSV: what you need to know to care for your pregnant patient. MCN Am J Matern Child Nurs. 2007 Nov-Dec;32(6):345-50. doi: 10.1097/01.NMC.0000298128.09290.bb. PMID: 17968215. Disponible en: https://pubmed.ncbi.nlm.nih.gov/17968215/
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








