Uterine Cancer and the Human Papillomavirus Infection

Written and verified by the biologist Olga Carbajo
The uterus is the woman’s reproductive organ, and is where gestation takes place. It’s located in the pelvic cavity and is made up of two layers: the myometrium, or outer membrane, and the endometrium, which is the innermost part. Depending on where the tumor is, and the biological makeup of the uterine cancer, scientists classify them into different types. This can then help in the choice of treatment.
What is uterine cancer?
The cells of our body are in constant regeneration. Following the cell cycle, they grow, reproduce, and die. But sometimes our body doesn’t follow this pattern. Control systems fail and uncontrolled growth occurs, leading to the appearance of a tumor.
According to the National Cancer Institute (NIH), there are three types of cancer of the uterus: endometrial cancer, the most common, cervical cancer, and uterine sarcoma. The latter is more difficult to treat and is usually malignant.
In addition to this, there can be an uncontrolled growth of the tumor cells which then infiltrates the adjacent tissues. This can also migrate to other organs and initiate a process of metastasis. Therefore, depending on the location of the nodule or tumor, we can classify the tumor into three subtypes:
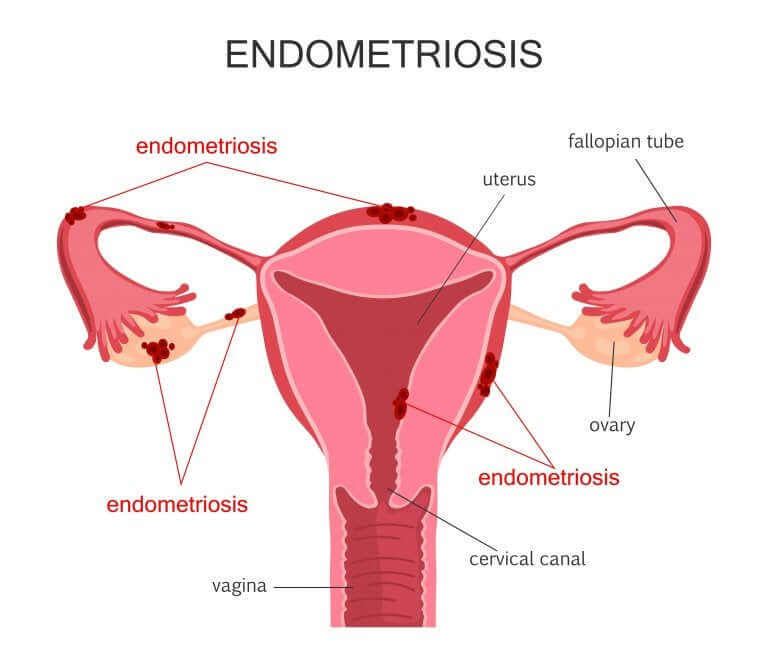
- Local. This type spreads to the cervix, or to the outer part, the myometrium.
- Lymphatic. The lymphatic system is one of the most important parts of the immune system, as it’s the body’s drainage mechanism. When tumor cells reach it, then this may affect the pelvic nodes.
- Hematogenous. In this rare case, the tumor reaches the bloodstream, and so, from here, it can invade any organ in the body.
The science behind uterine cancer
The main risk factor with uterine cancer is infection with the Human Papillomavirus Infection (HPV). The malignant cells will be almost exclusively in the cervix (if there hasn’t been any metastasis). This is at the lower end of the uterus and connects the uterus to the vagina.
It’s a disease that progresses very slowly, and the cells with an abnormal growth go through different stages. These stages are called dysplasia and, despite being abnormal cells, they still aren’t cancerous. We should point out here that tumors won’t necessarily develop in all cases.
After a positive diagnosis, doctors will usually perform several tests to determine the extent and severity of the disease. They’ll check to see if it has spread or if it’s localized. On this basis, experts classify cervical cancer into the following stages of increased to decreased severity: IV, III, II, I, and carcinoma in situ (subtype 0).
The Human Papillomavirus Infection (HPV)
Experts consider this to be one of the most common sexually transmitted infections in existence. It’s usually asymptomatic and disappears automatically. However, recent studies have shown that it can remain dormant for more than two years and be transmitted unknowingly.

Among the more than 100 identified genotypes of HPV, some can cause warts by infecting the mucous membranes and others, the most aggressive types, can trigger a cancerous process. However, Dr. Pedro Herranz Pinto, a dermatologist at Hospital La Paz in Madrid, gives us the following advice:
“The patient should be treated only if they have cytological alterations, not if they have HPV.”
– Dr. Pedro Herranz Pinto –
In addition to this, there probably won’t be any signs or symptoms of early uterine cancer. In this regard, the CDC (Center for Infectious Disease Control) tells us on its website what we can do to prevent the spread of HPV:
- Vaccination. The HPV vaccine is totally safe and effective, and protects both women and men.
- Get a cervical cancer screening test from age 30 onwards on a regular basis.
- Use a condom if you aren’t in a monogamous relationship.
Early detection allows for a better recovery if doctors detect cancer at an early stage:
“Declare the past, diagnose the present and predict the future.”
– Hypocrates –
The uterus is the woman’s reproductive organ, and is where gestation takes place. It’s located in the pelvic cavity and is made up of two layers: the myometrium, or outer membrane, and the endometrium, which is the innermost part. Depending on where the tumor is, and the biological makeup of the uterine cancer, scientists classify them into different types. This can then help in the choice of treatment.
What is uterine cancer?
The cells of our body are in constant regeneration. Following the cell cycle, they grow, reproduce, and die. But sometimes our body doesn’t follow this pattern. Control systems fail and uncontrolled growth occurs, leading to the appearance of a tumor.
According to the National Cancer Institute (NIH), there are three types of cancer of the uterus: endometrial cancer, the most common, cervical cancer, and uterine sarcoma. The latter is more difficult to treat and is usually malignant.
In addition to this, there can be an uncontrolled growth of the tumor cells which then infiltrates the adjacent tissues. This can also migrate to other organs and initiate a process of metastasis. Therefore, depending on the location of the nodule or tumor, we can classify the tumor into three subtypes:

- Local. This type spreads to the cervix, or to the outer part, the myometrium.
- Lymphatic. The lymphatic system is one of the most important parts of the immune system, as it’s the body’s drainage mechanism. When tumor cells reach it, then this may affect the pelvic nodes.
- Hematogenous. In this rare case, the tumor reaches the bloodstream, and so, from here, it can invade any organ in the body.
The science behind uterine cancer
The main risk factor with uterine cancer is infection with the Human Papillomavirus Infection (HPV). The malignant cells will be almost exclusively in the cervix (if there hasn’t been any metastasis). This is at the lower end of the uterus and connects the uterus to the vagina.
It’s a disease that progresses very slowly, and the cells with an abnormal growth go through different stages. These stages are called dysplasia and, despite being abnormal cells, they still aren’t cancerous. We should point out here that tumors won’t necessarily develop in all cases.
After a positive diagnosis, doctors will usually perform several tests to determine the extent and severity of the disease. They’ll check to see if it has spread or if it’s localized. On this basis, experts classify cervical cancer into the following stages of increased to decreased severity: IV, III, II, I, and carcinoma in situ (subtype 0).
The Human Papillomavirus Infection (HPV)
Experts consider this to be one of the most common sexually transmitted infections in existence. It’s usually asymptomatic and disappears automatically. However, recent studies have shown that it can remain dormant for more than two years and be transmitted unknowingly.

Among the more than 100 identified genotypes of HPV, some can cause warts by infecting the mucous membranes and others, the most aggressive types, can trigger a cancerous process. However, Dr. Pedro Herranz Pinto, a dermatologist at Hospital La Paz in Madrid, gives us the following advice:
“The patient should be treated only if they have cytological alterations, not if they have HPV.”
– Dr. Pedro Herranz Pinto –
In addition to this, there probably won’t be any signs or symptoms of early uterine cancer. In this regard, the CDC (Center for Infectious Disease Control) tells us on its website what we can do to prevent the spread of HPV:
- Vaccination. The HPV vaccine is totally safe and effective, and protects both women and men.
- Get a cervical cancer screening test from age 30 onwards on a regular basis.
- Use a condom if you aren’t in a monogamous relationship.
Early detection allows for a better recovery if doctors detect cancer at an early stage:
“Declare the past, diagnose the present and predict the future.”
– Hypocrates –
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- AECC (última consulta junio 2019). Estadística del cáncer de cerviz [artículo en web]. Recuperado de: www.aecc.es
- AECC (última consulta junio 2019). Qué es el cáncer de útero [artículo en web]. Recuperado de: www.aecc.es
- NIH (19 abril 2019). Tratamiento del cáncer de cuello uterino [artículo en web]. Recuperado de www.cáncer.gov
- Salaber, E. (28 agosto 2013). Entrevista al DR. Pedro Herranz Pinto. Recuperado de www.webconsultas.com
- CDC (07 de febrero de 2017). Virus del papiloma humano genital [artículo en revista]. Recuperado de: www.cdc.gov
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








