What is the Nuchal Fold Measurement?
In all pregnancies, there’s a risk that the baby has a genetic alteration, and to assess the risk of these diseases, it’s possible to carry out some specific studies. One of them is the measurement of the nuchal fold, a presumptive test obtained from ultrasound observation.
This study isn’t performed at any time during pregnancy or in any way, and this is closely related to its usefulness. In the following article, we’ll tell you all about the test and why it’s so important that you have it done.
What is the nuchal fold?
When we talk about the nuchal fold, we’re referring to a thickening of the posterior area of the neck, where an accumulation of amniotic fluid occurs.
The amount of fluid that’s retained there can give the specialist some clues about the possibility of a baby having an alteration in its genes or chromosomes. Fetuses with these health conditions usually have larger nuchal folds, which is why it’s extremely useful to practice this measurement during pregnancy.
Nuchal fold measurement
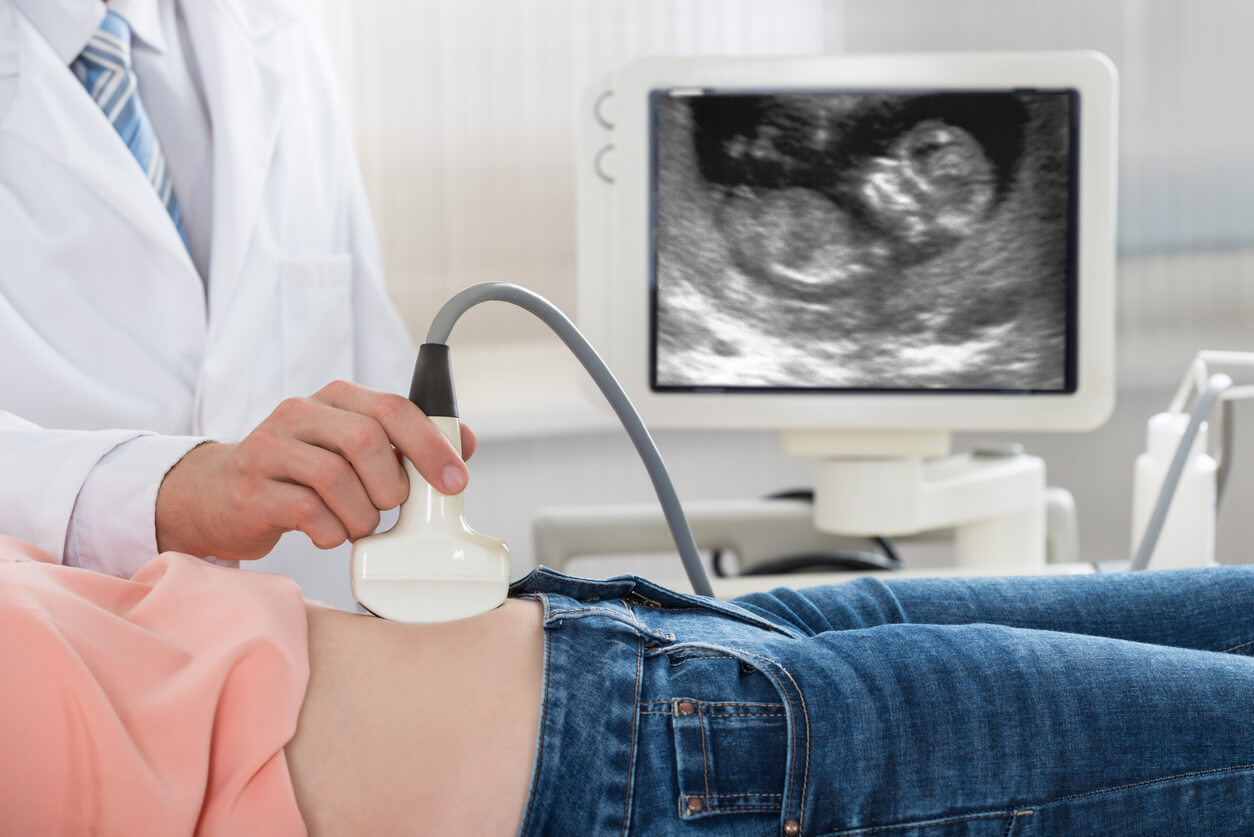
The nuchal fold measurement, also known as the nuchal translucency test, is a non-invasive test that’s performed between the 11th and 14th week of pregnancy. As we’ve mentioned, its purpose is to find data suggestive of a disease in the baby’s DNA.
To perform it, the doctor performs an abdominal ultrasound with a high-resolution ultrasound machine and thus achieves a more precise measurement. During the test, the professional must look for a lateral plane, which allows them to evaluate the craniocaudal length (CCL) of the child, which is the distance from the head to the coccyx. Ideally, the fetus should measure between 45 and 84 mm for the study to be done correctly.
Once the device is located, the maximum thickness of the nuchal fold is measured, specifically the shadow (or translucency) that remains between the skin and the soft tissue that covers the cervical spine. Normally, this thickness is less than 3 mm.
When the nuchal translucency is above this value, it can be associated with an increased risk of certain genetic diseases, such as Down syndrome.
Through the nuchal translucency measurement, it’s possible to identify more than 75% of fetuses with this condition. However, it should be emphasized that this test isn’t diagnostic or confirmatory, but is taken as a reference to assess the need for more specific studies.
My baby has an increased nuchal fold, what should I do?
If this measurement is increased, this isn’t synonymous with a genetic disease. In fact, in more than 3% of cases, increased nuchal translucency occurs in completely normal fetuses.
What the study does suggest is the need for more specific tests to confirm or rule out this possibility. For example, the measurement of the nasal bone in the same ultrasound and the determination of the growth rate according to the weeks of pregnancy.
If these results are also altered, the doctor will proceed to request two more triple tests, which is a complementary screening based on three different studies.
Nuchal fold measurement and triple test
The measurement of the nuchal fold is part of the combined test of the first trimester or triple test. In other words, it’s necessary to complement the results of three screening tests to determine the true risk of the baby presenting a genetic disorder.
The remaining two measurements are carried out by means of a blood test, which is carried out between weeks 11 and 13. They look for two biochemical markers: PAPP-A (pregnancy-associated blood plasma protein A) and ßhCG (free portion of human chorionic gonadotropin).
When ßHCG levels are above normal and PAPP-A levels are decreased, in a baby whose nuchal translucency is also increased, the risk of Down syndrome is high.
These 3 results are checked against other data (maternal age, weight, and ethnicity) on a computer. From there, the percentage of risk is obtained that the baby actually suffers from one of the most frequent trisomies, in chromosomes 13, 18, or 21.
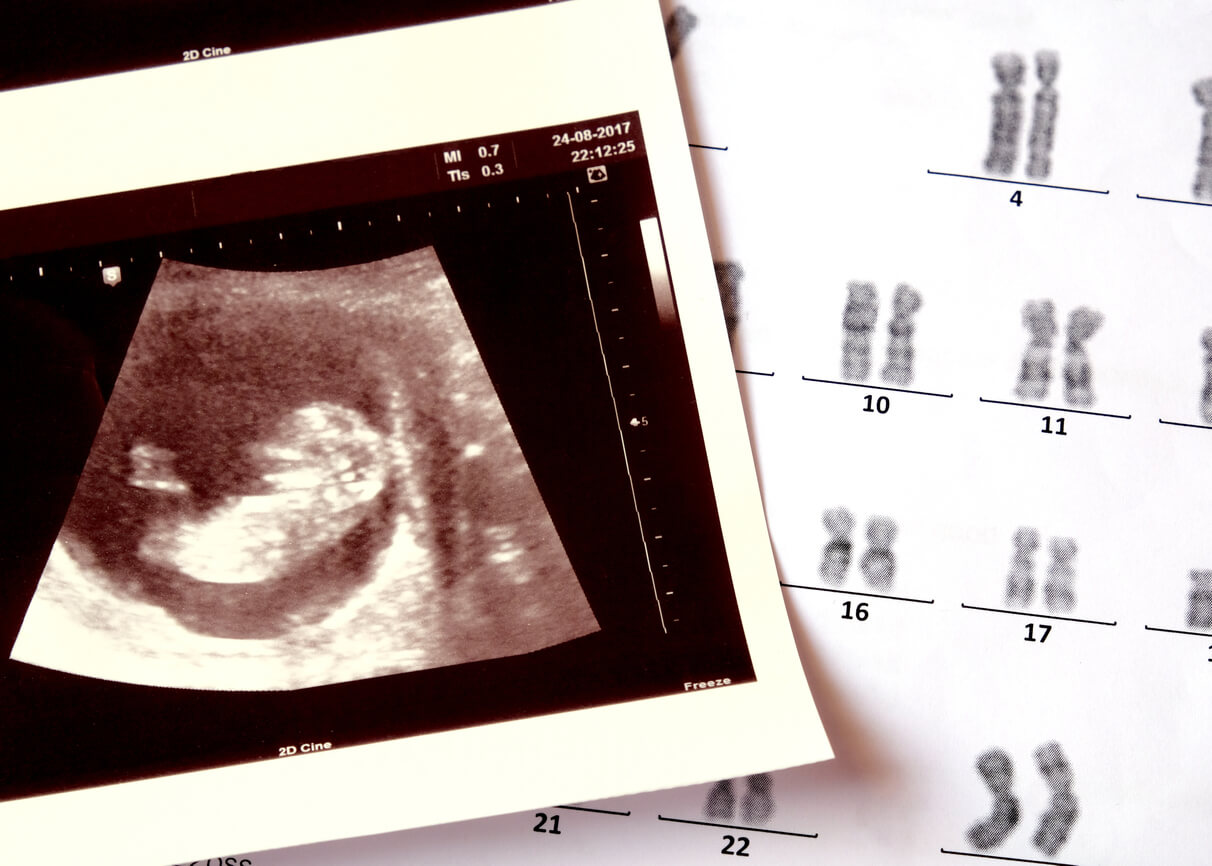
When are other studies indicated?
When the triple test result is greater than 1/270 (that is, one possibility for every 270 pregnancies), the risk of suffering from one of the trisomies mentioned is low. This isn’t definitive, but the chances of error are low.
On the contrary, when it’s less than 1/270, the probability that the baby actually carries a defect in its genes is high. To corroborate this result, the specialist will indicate the performance of other diagnostic studies, such as amniocentesis or chorionic villus biopsy. Both prenatal tests are invasive, but provide highly reliable results.
Another possible option is for the mother to undergo the fetal DNA test using maternal blood, which is non-invasive and serves to detect the previously mentioned diseases. However, this study isn’t done routinely in all pregnant women.
About prenatal tests
The measurement of the nuchal fold is one of the presumptive tests with which it’s been possible to reduce the need to resort to invasive tests (such as amniocentesis) to assess the well-being of the baby.
However, it’s worth clarifying that in many cases, the results of these screening studies can cause concern in pregnant women because they’re not 100% specific. For this reason, it’s best to follow the specialist’s instructions to the letter and wait calmly for the definitive diagnostic results.
In all pregnancies, there’s a risk that the baby has a genetic alteration, and to assess the risk of these diseases, it’s possible to carry out some specific studies. One of them is the measurement of the nuchal fold, a presumptive test obtained from ultrasound observation.
This study isn’t performed at any time during pregnancy or in any way, and this is closely related to its usefulness. In the following article, we’ll tell you all about the test and why it’s so important that you have it done.
What is the nuchal fold?
When we talk about the nuchal fold, we’re referring to a thickening of the posterior area of the neck, where an accumulation of amniotic fluid occurs.
The amount of fluid that’s retained there can give the specialist some clues about the possibility of a baby having an alteration in its genes or chromosomes. Fetuses with these health conditions usually have larger nuchal folds, which is why it’s extremely useful to practice this measurement during pregnancy.

Nuchal fold measurement
The nuchal fold measurement, also known as the nuchal translucency test, is a non-invasive test that’s performed between the 11th and 14th week of pregnancy. As we’ve mentioned, its purpose is to find data suggestive of a disease in the baby’s DNA.
To perform it, the doctor performs an abdominal ultrasound with a high-resolution ultrasound machine and thus achieves a more precise measurement. During the test, the professional must look for a lateral plane, which allows them to evaluate the craniocaudal length (CCL) of the child, which is the distance from the head to the coccyx. Ideally, the fetus should measure between 45 and 84 mm for the study to be done correctly.
Once the device is located, the maximum thickness of the nuchal fold is measured, specifically the shadow (or translucency) that remains between the skin and the soft tissue that covers the cervical spine. Normally, this thickness is less than 3 mm.
When the nuchal translucency is above this value, it can be associated with an increased risk of certain genetic diseases, such as Down syndrome.
Through the nuchal translucency measurement, it’s possible to identify more than 75% of fetuses with this condition. However, it should be emphasized that this test isn’t diagnostic or confirmatory, but is taken as a reference to assess the need for more specific studies.
My baby has an increased nuchal fold, what should I do?
If this measurement is increased, this isn’t synonymous with a genetic disease. In fact, in more than 3% of cases, increased nuchal translucency occurs in completely normal fetuses.
What the study does suggest is the need for more specific tests to confirm or rule out this possibility. For example, the measurement of the nasal bone in the same ultrasound and the determination of the growth rate according to the weeks of pregnancy.
If these results are also altered, the doctor will proceed to request two more triple tests, which is a complementary screening based on three different studies.
Nuchal fold measurement and triple test
The measurement of the nuchal fold is part of the combined test of the first trimester or triple test. In other words, it’s necessary to complement the results of three screening tests to determine the true risk of the baby presenting a genetic disorder.
The remaining two measurements are carried out by means of a blood test, which is carried out between weeks 11 and 13. They look for two biochemical markers: PAPP-A (pregnancy-associated blood plasma protein A) and ßhCG (free portion of human chorionic gonadotropin).
When ßHCG levels are above normal and PAPP-A levels are decreased, in a baby whose nuchal translucency is also increased, the risk of Down syndrome is high.
These 3 results are checked against other data (maternal age, weight, and ethnicity) on a computer. From there, the percentage of risk is obtained that the baby actually suffers from one of the most frequent trisomies, in chromosomes 13, 18, or 21.

When are other studies indicated?
When the triple test result is greater than 1/270 (that is, one possibility for every 270 pregnancies), the risk of suffering from one of the trisomies mentioned is low. This isn’t definitive, but the chances of error are low.
On the contrary, when it’s less than 1/270, the probability that the baby actually carries a defect in its genes is high. To corroborate this result, the specialist will indicate the performance of other diagnostic studies, such as amniocentesis or chorionic villus biopsy. Both prenatal tests are invasive, but provide highly reliable results.
Another possible option is for the mother to undergo the fetal DNA test using maternal blood, which is non-invasive and serves to detect the previously mentioned diseases. However, this study isn’t done routinely in all pregnant women.
About prenatal tests
The measurement of the nuchal fold is one of the presumptive tests with which it’s been possible to reduce the need to resort to invasive tests (such as amniocentesis) to assess the well-being of the baby.
However, it’s worth clarifying that in many cases, the results of these screening studies can cause concern in pregnant women because they’re not 100% specific. For this reason, it’s best to follow the specialist’s instructions to the letter and wait calmly for the definitive diagnostic results.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Grupo de trabajo de la Sociedad Española de Ginecología y Obstetricia (SEGO) (2013). Guía de práctica clínica: Diagnóstico prenatal de los defectos congénitos. Cribado de anomalías cromosómicas. Elsevier. Vol. 24. Núm. 2. Pp. 57-72. Recuperado de: https://www.elsevier.es/es-revista-diagnostico-prenatal-327-articulo-guia-practica-clinica-diagnostico-prenatal-S2173412712001059
- Hernández, J. (2010) Evaluación de la translucencia del pliegue nucal en la detección de aneuploidias. Revista médica de Costa Rica y Centroamérica LXVII (594) 385-390.
- Ramos, D. et al (2005). Translucencia nucal. Clínica e Investigación en Ginecología y Obstetricia. Vol. 32. Núm. 2. Pp.54-60 Recuperado de: https://www.elsevier.es/es-revista-clinica-e-investigacion-ginecologia-obstetricia-7-articulo-translucencia-nucal-13074916
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








