How to Remove Cradle Cap from Babies?


Written and verified by the dermatologist Maria del Carmen Hernandez
Baby cradle cap is a common and benign condition that most often occurs on the scalp. Although it’s a condition that resolves spontaneously, there are easy and simple measures to accelerate its elimination. In general, it doesn’t cause discomfort, itching, or pain in the infant. However, many parents may have concerns about it and wonder how to remove cradle cap.
What is cradle cap?
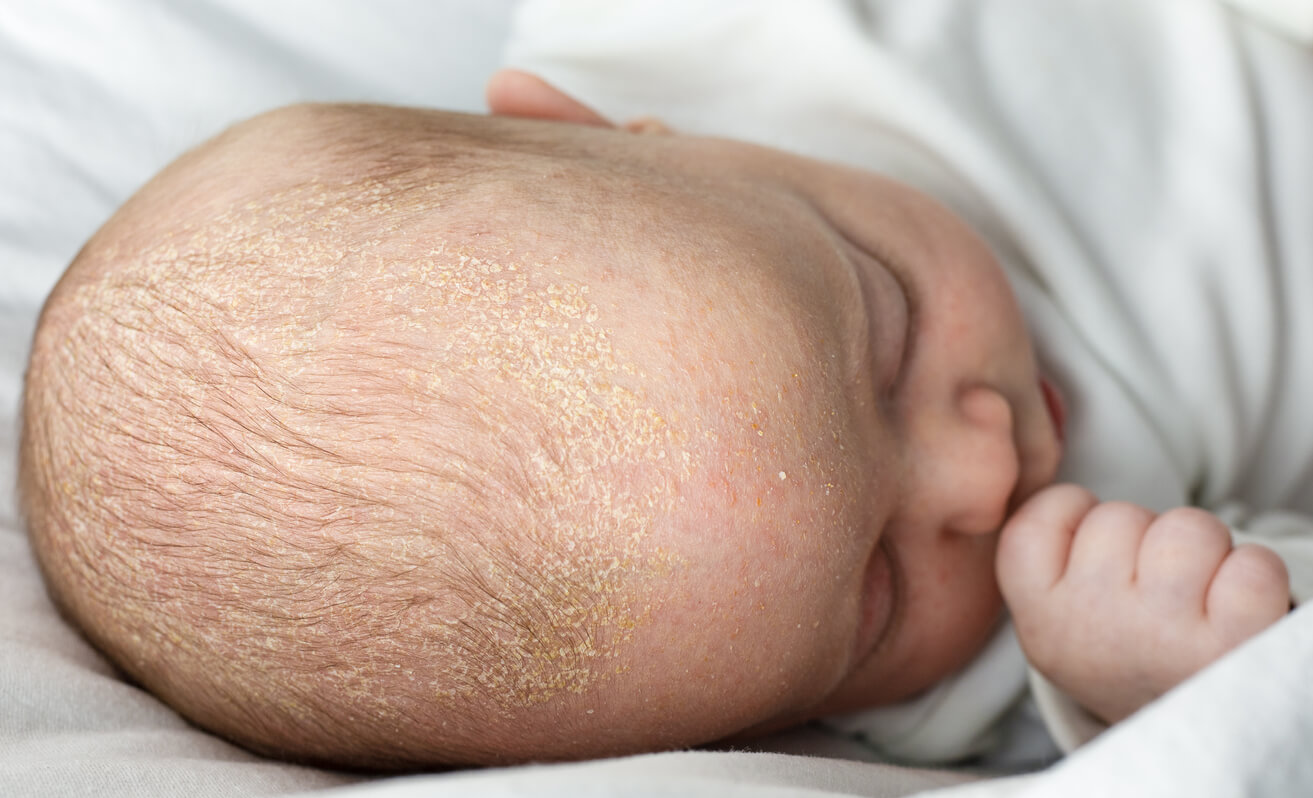
Cradle cap is a variant of infantile seborrheic dermatitis characterized by a non-inflammatory scaly reaction on the scalp. This usually occurs in the first weeks of life. The cutaneous manifestations are characterized by erythematous plaques with yellowish, greasy-looking scales in areas with a higher concentration of sebaceous glands. For example, on the T-line of the face, scalp, and outer ears.
It’s even common in early childhood, without symptoms, itching, or pain, according to studies by the American Family Physician. Infants have no side effects of the condition and their feeding and sleep aren’t disturbed. In turn, there’s no evidence associating its presence with lactose intolerance or poor hygiene.
You may be interested in: Seborrheic Dermatitis in Children
How to eliminate cradle cap
Parents should be properly instructed on the management and benign nature of cradle cap. In general, it’s a self-limiting skin condition, so treatment should be conservative in mild and localized cases. Unless there’s an inflammatory process or secondary bacterial infection, medical treatment is not recommended.
The use of oils
Moisturizing the scalp is effective in softening the adherent scales. Therefore, the use of oils helps to soften the scale and facilitates removal. Almond or olive oil can be effective in removing scales adhering to the skin surface. After application, it should be left on for a few minutes and then circular motions should be used to help remove cradle cap.
Scalp washing
Scalp rinsing with mild, neutral hygiene products, along with an emollient (baby oil or white petroleum jelly), is a very useful recommendation. Emollients are very effective if kept in contact with the skin surface for a prolonged period of time.
Constant brushing
Gently brushing the baby’s scalp is a good way to remove some scales. However, care should be taken not to scratch or injure the skin. It’s advisable to brush at least once a day; however, in case of irritation, less frequent brushing is recommended. This method is safe and even stimulates blood circulation while removing scales.
Medical treatment
The use of specific drugs isn’t recommended as an initial management option. However, the Spanish Association of Pediatrics recommends taking some measures in case of resistant cases.
- Topical corticosteroids: They should be prescribed by the treating physician, who will indicate a low-potency option. In general, they act quickly after a few days.
- Oral corticosteroids: They’re used in severe or generalized cases and must be prescribed by the physician to administer the correct doses.
- Shampoos: There are specific products on the market to help with the shedding of scalp scales. They contain zinc pyrithione or sulfur, which can be a bit irritating.
- Keratolytics: These are products whose purpose is to cause the crusts to break up and fall off.
- Antifungals: They usually take the form of creams containing 2% ketoconazole.
- Borage oil: Its prolonged use is effective in the elimination of scabs due to its high content of 24% gamma-linolenic acid.
In addition, it’s best to keep the baby’s nails short to avoid injury in case of scratching.
Read also: Top 10 Baby Skin Irritants

Differential diagnoses
One condition that’s commonly confused with cradle cap is atopic dermatitis. However, atopic skin appears with moderate to severe itching and disturbs the feeding and sleep of the newborn. It even produces scaly, erythematous lesions and, sometimes, crusts that aren’t well-defined in the region of the cheeks, extensor surfaces, and scalp.
It can also resemble impetigo lesions; however, its manifestations begin with fragile vesicles. In turn, tinea capitis presents similar manifestations that are often accompanied by hair loss and lymphadenopathy.
What to remember about cradle cap
Although it’s a condition that’s not serious and disappears spontaneously, it’s the first sign of infantile seborrheic dermatitis. In addition, it’s not a condition that’s contagious or passed from person to person. If the condition persists beyond 12 months of age, alternative diagnoses should be further investigated.
Baby cradle cap is a common and benign condition that most often occurs on the scalp. Although it’s a condition that resolves spontaneously, there are easy and simple measures to accelerate its elimination. In general, it doesn’t cause discomfort, itching, or pain in the infant. However, many parents may have concerns about it and wonder how to remove cradle cap.
What is cradle cap?
Cradle cap is a variant of infantile seborrheic dermatitis characterized by a non-inflammatory scaly reaction on the scalp. This usually occurs in the first weeks of life. The cutaneous manifestations are characterized by erythematous plaques with yellowish, greasy-looking scales in areas with a higher concentration of sebaceous glands. For example, on the T-line of the face, scalp, and outer ears.
It’s even common in early childhood, without symptoms, itching, or pain, according to studies by the American Family Physician. Infants have no side effects of the condition and their feeding and sleep aren’t disturbed. In turn, there’s no evidence associating its presence with lactose intolerance or poor hygiene.
You may be interested in: Seborrheic Dermatitis in Children
How to eliminate cradle cap
Parents should be properly instructed on the management and benign nature of cradle cap. In general, it’s a self-limiting skin condition, so treatment should be conservative in mild and localized cases. Unless there’s an inflammatory process or secondary bacterial infection, medical treatment is not recommended.

The use of oils
Moisturizing the scalp is effective in softening the adherent scales. Therefore, the use of oils helps to soften the scale and facilitates removal. Almond or olive oil can be effective in removing scales adhering to the skin surface. After application, it should be left on for a few minutes and then circular motions should be used to help remove cradle cap.
Scalp washing
Scalp rinsing with mild, neutral hygiene products, along with an emollient (baby oil or white petroleum jelly), is a very useful recommendation. Emollients are very effective if kept in contact with the skin surface for a prolonged period of time.
Constant brushing
Gently brushing the baby’s scalp is a good way to remove some scales. However, care should be taken not to scratch or injure the skin. It’s advisable to brush at least once a day; however, in case of irritation, less frequent brushing is recommended. This method is safe and even stimulates blood circulation while removing scales.
Medical treatment
The use of specific drugs isn’t recommended as an initial management option. However, the Spanish Association of Pediatrics recommends taking some measures in case of resistant cases.
- Topical corticosteroids: They should be prescribed by the treating physician, who will indicate a low-potency option. In general, they act quickly after a few days.
- Oral corticosteroids: They’re used in severe or generalized cases and must be prescribed by the physician to administer the correct doses.
- Shampoos: There are specific products on the market to help with the shedding of scalp scales. They contain zinc pyrithione or sulfur, which can be a bit irritating.
- Keratolytics: These are products whose purpose is to cause the crusts to break up and fall off.
- Antifungals: They usually take the form of creams containing 2% ketoconazole.
- Borage oil: Its prolonged use is effective in the elimination of scabs due to its high content of 24% gamma-linolenic acid.
In addition, it’s best to keep the baby’s nails short to avoid injury in case of scratching.
Read also: Top 10 Baby Skin Irritants

Differential diagnoses
One condition that’s commonly confused with cradle cap is atopic dermatitis. However, atopic skin appears with moderate to severe itching and disturbs the feeding and sleep of the newborn. It even produces scaly, erythematous lesions and, sometimes, crusts that aren’t well-defined in the region of the cheeks, extensor surfaces, and scalp.
It can also resemble impetigo lesions; however, its manifestations begin with fragile vesicles. In turn, tinea capitis presents similar manifestations that are often accompanied by hair loss and lymphadenopathy.
What to remember about cradle cap
Although it’s a condition that’s not serious and disappears spontaneously, it’s the first sign of infantile seborrheic dermatitis. In addition, it’s not a condition that’s contagious or passed from person to person. If the condition persists beyond 12 months of age, alternative diagnoses should be further investigated.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Nobles T, Harberger S, Krishnamurthy K. Cradle Cap. 2021 Aug 11. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2021 Jan–. PMID: 30285358.
- Sheffield RC, Crawford P, Wright ST, King VJ. Clinical inquiries. What’s the best treatment for cradle cap? J Fam Pract. 2007 Mar;56(3):232-3. PMID: 17343816.
- Micali G, Pulvirenti N, Dall’Oglio F, Tedeschi A, Quattrocchi E, Lacarrubba F. Treatment of cradle cap in infants with a new cosmetic non-steroidal gel cream: Clinical, laboratory, and instrumental evaluation. J Cosmet Dermatol. 2021 Apr;20 Suppl 1(Suppl 1):14-17. doi: 10.1111/jocd.14095. PMID: 33934474; PMCID: PMC8252604.
- Victoire A, Magin P, Coughlan J, van Driel ML. Intervenciones para la dermatitis seborreica infantil (incluida la costra láctea). Cochrane Database Syst Rev.2019 4 de marzo; 3 (3): CD011380. doi: 10.1002 / 14651858.CD011380.pub2. PMID: 30828791; PMCID: PMC6397947.
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








