Bursitis in Children: What You Should Know

Sports activity is one of the most recommended healthy habits for people of all ages. If your child plays sports, it’s important that they learn about taking care of their own body. At the same time, always remind them that the objective of this practice is recreation, as excessive sports demands can lead to injuries, such as bursitis in children.
This disease is a type of progressive joint inflammation that occurs due to the overuse of said structure. Sometimes, it resolves spontaneously but, other times, you need to resort to medical treatment, physical therapy, or both.
If left untreated, bursitis can come, go, and come back again and again. Find out how to prevent it in the following article. Keep reading!
What is bursitis in children?
Bursitis is a health condition characterized by inflammation of the bursa, which is a small sac of synovial fluid that protects the joints. It occurs most often in the most mobile joints of the body, such as the shoulders, elbows, wrists, and knees.
It’s generally a mild condition, although it often limits the activities of daily life. This ailment usually affects the most demanding joints of the body, either due to a type of repetitive movement or a sustained overload over time.
Pediatricians usually diagnose bursitis by means of asking questions and physically examining the child. Sometimes, they must also request complementary imaging studies to rule out other diseases. And in exceptional cases, they may have to resort to the extraction and analysis of the synovial fluid contained in the joint.
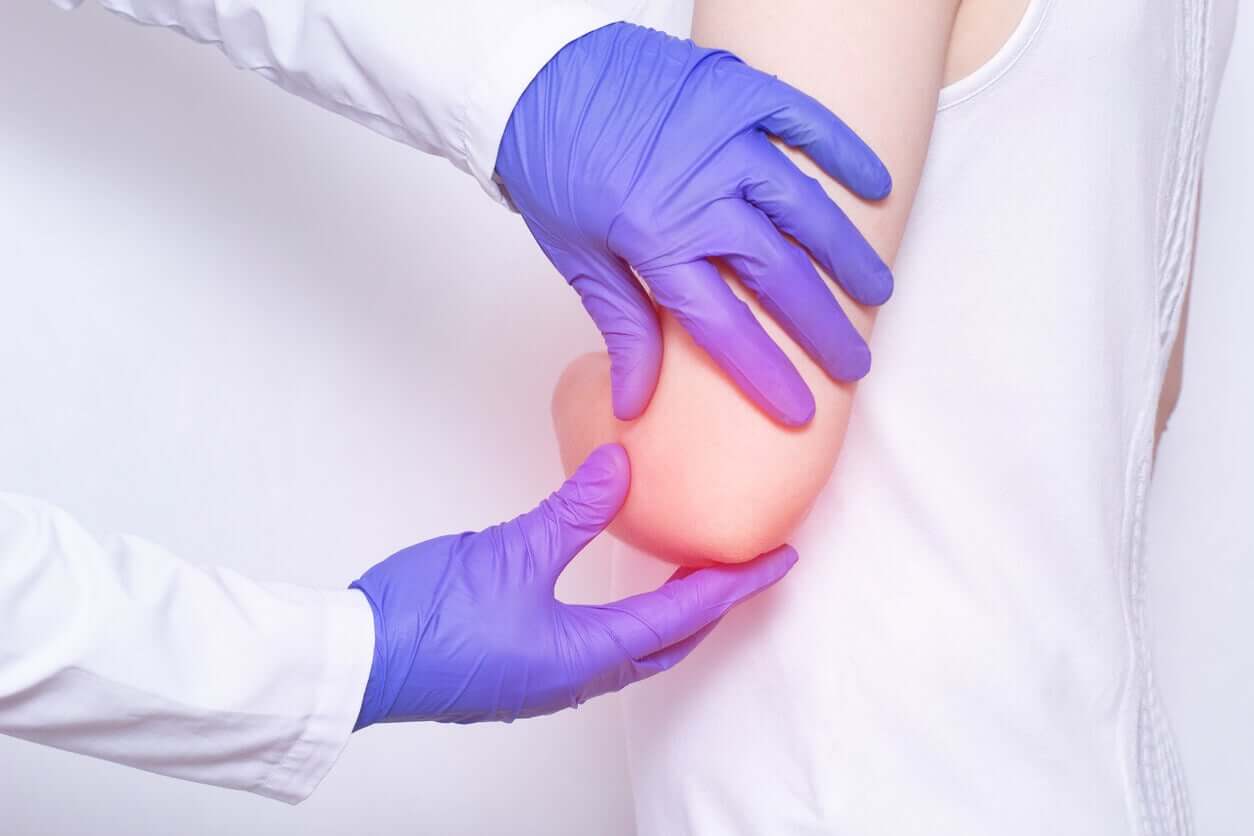
The causes of bursitis in children
Bursa inflammation tends to occur more frequently in adults, but it can manifest itself in children due to a repetitive and sustained movement over time. The risk of suffering these injuries will depend on the activity that’s practiced.
Next, we’ll explain the most frequent causes:
- Sports: This condition is common in tennis and usually affects the elbow and wrists, while in soccer the knees are usually affected. At the same time, ballet requires non-physiological postures of the feet and favors the inflammation of the joints. Therefore, each sport predisposes children to a different type of injury, depending on the predominant movement.
- Musical instruments: For example, with the piano, the wrists and hands are specifically vulnerable.
- Joint infections or inflammatory processes (such as rheumatoid arthritis).
- Direct trauma.
Whatever the activity, the child’s body must be protected and the correct postures for each activity must be respected. Likewise, try not to carry out activities that are too intense for their degree of development.
Symptoms and signs of bursitis
A child with bursitis will present different signs and symptoms, depending on whether the condition’s acute or chronic. In acute bursitis, symptoms appear suddenly and include the following:
- Severe joint pain
- Increased temperature in the affected joint.
- Redness in the area
- Inflammation
- Tenderness to the touch
- Fever (less frequent)
When it comes to chronic bursitis, which is the type that lasts over time, some of the manifestations detailed below can be added:
- Muscular weakness
- Joint limitation
- Functional impotence (inability to perform its main function)
How is bursitis treated?
The treatment of bursitis in children depends on the severity of the disease.
In milder cases, rest and the application of local cold (cryotherapy) are usually sufficient. In addition, you can opt for the use of oral anti-inflammatories, which should be indicated by the pediatrician.
Fewer children need injections (injection of drugs into the joint) and treatment with antibiotics. Surgery to decompress the area and repair the damage is necessary in very few cases.
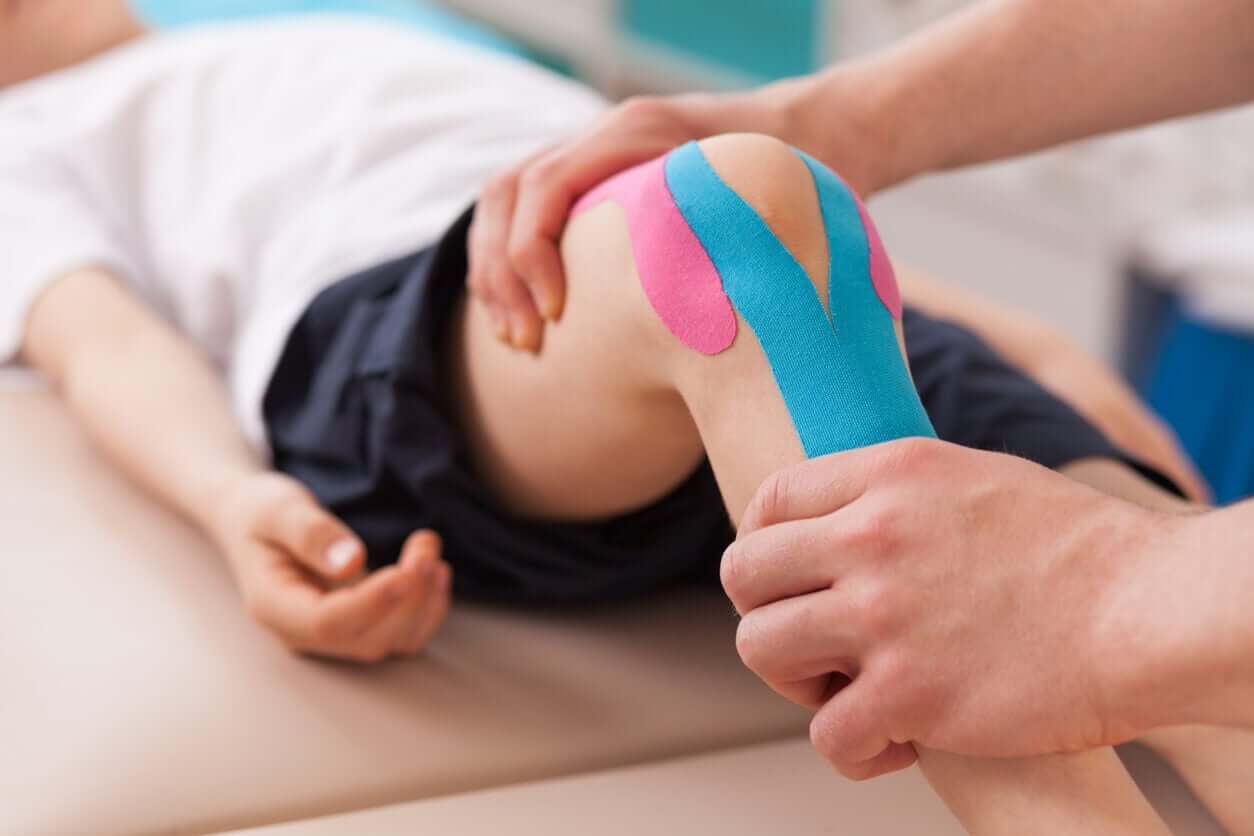
Pediatric physiotherapy offers a conservative, non-invasive, and highly effective treatment for mild to moderate acute cases and also for chronic processes. Through mobilizations and manual techniques, it’s possible to improve the joint range of motion and strengthen the affected muscles. In addition, this discipline uses physical agents such as cryotherapy, ultrasound, and magnetotherapy to reduce local inflammation and relieve symptoms.
You may also be interested in: Wrist Tendonitis in Children: What You Should Know
Prevention is best
In child health issues, prevention is essential in order to avoid complications in the future. Therefore, make sure your child always warms up properly before each activity. Likewise, be sure to take the necessary precautions to prevent injuries, such as bandaging the wrists or ankles and avoiding repetitive movements or overstressing the joints.
Finally, don’t forget the fundamental role that healthy eating and adequate hydration play in the prevention of sports accidents.
Sports activity is one of the most recommended healthy habits for people of all ages. If your child plays sports, it’s important that they learn about taking care of their own body. At the same time, always remind them that the objective of this practice is recreation, as excessive sports demands can lead to injuries, such as bursitis in children.
This disease is a type of progressive joint inflammation that occurs due to the overuse of said structure. Sometimes, it resolves spontaneously but, other times, you need to resort to medical treatment, physical therapy, or both.
If left untreated, bursitis can come, go, and come back again and again. Find out how to prevent it in the following article. Keep reading!
What is bursitis in children?
Bursitis is a health condition characterized by inflammation of the bursa, which is a small sac of synovial fluid that protects the joints. It occurs most often in the most mobile joints of the body, such as the shoulders, elbows, wrists, and knees.
It’s generally a mild condition, although it often limits the activities of daily life. This ailment usually affects the most demanding joints of the body, either due to a type of repetitive movement or a sustained overload over time.
Pediatricians usually diagnose bursitis by means of asking questions and physically examining the child. Sometimes, they must also request complementary imaging studies to rule out other diseases. And in exceptional cases, they may have to resort to the extraction and analysis of the synovial fluid contained in the joint.

The causes of bursitis in children
Bursa inflammation tends to occur more frequently in adults, but it can manifest itself in children due to a repetitive and sustained movement over time. The risk of suffering these injuries will depend on the activity that’s practiced.
Next, we’ll explain the most frequent causes:
- Sports: This condition is common in tennis and usually affects the elbow and wrists, while in soccer the knees are usually affected. At the same time, ballet requires non-physiological postures of the feet and favors the inflammation of the joints. Therefore, each sport predisposes children to a different type of injury, depending on the predominant movement.
- Musical instruments: For example, with the piano, the wrists and hands are specifically vulnerable.
- Joint infections or inflammatory processes (such as rheumatoid arthritis).
- Direct trauma.
Whatever the activity, the child’s body must be protected and the correct postures for each activity must be respected. Likewise, try not to carry out activities that are too intense for their degree of development.
Symptoms and signs of bursitis
A child with bursitis will present different signs and symptoms, depending on whether the condition’s acute or chronic. In acute bursitis, symptoms appear suddenly and include the following:
- Severe joint pain
- Increased temperature in the affected joint.
- Redness in the area
- Inflammation
- Tenderness to the touch
- Fever (less frequent)
When it comes to chronic bursitis, which is the type that lasts over time, some of the manifestations detailed below can be added:
- Muscular weakness
- Joint limitation
- Functional impotence (inability to perform its main function)
How is bursitis treated?
The treatment of bursitis in children depends on the severity of the disease.
In milder cases, rest and the application of local cold (cryotherapy) are usually sufficient. In addition, you can opt for the use of oral anti-inflammatories, which should be indicated by the pediatrician.
Fewer children need injections (injection of drugs into the joint) and treatment with antibiotics. Surgery to decompress the area and repair the damage is necessary in very few cases.
Pediatric physiotherapy offers a conservative, non-invasive, and highly effective treatment for mild to moderate acute cases and also for chronic processes. Through mobilizations and manual techniques, it’s possible to improve the joint range of motion and strengthen the affected muscles. In addition, this discipline uses physical agents such as cryotherapy, ultrasound, and magnetotherapy to reduce local inflammation and relieve symptoms.
You may also be interested in: Wrist Tendonitis in Children: What You Should Know

Prevention is best
In child health issues, prevention is essential in order to avoid complications in the future. Therefore, make sure your child always warms up properly before each activity. Likewise, be sure to take the necessary precautions to prevent injuries, such as bandaging the wrists or ankles and avoiding repetitive movements or overstressing the joints.
Finally, don’t forget the fundamental role that healthy eating and adequate hydration play in the prevention of sports accidents.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Biblioteca Nacional de Medicina (EE. UU.). Bursitis. MedlinePlus en español [Internet]. Actualizado julio 2021. Disponible en: https://medlineplus.gov/spanish/bursitis.html
- Sánchez Ruiz-Cabello, Francisco Javier, et al. Promoción de la actividad física en la infancia y la adolescencia (parte 1). Pediatría Atención Primaria 21.83 (2019): 279-291.
- Iragorri, Diana Sofía Hernández. INVESTIGACIÓN EN LA PRÁCTICA. Revista Virtual Universitaria: 59.
- Botayaa, Enrique Guillén, et al. Osteocondromatosis sinovial de rodilla: una causa infrecuente de gonalgia en edad pediátrica.
- Zuníno, Carlos, et al. Etiología y evolución de las infecciones osteo-articulares 2009-2015: Hospital Pediátrico del Centro Hospitalario Pereira Rossell, Uruguay. Revista chilena de infectología 34.3 (2017): 235-242.
- Hodgson, Felipe, and Angélica Ibáñez. DOLOR DE CADERA EN ADOLESCENTES: ESTUDIO Y TRATAMIENTO. Revista Médica Clínica Las Condes 32.3 (2021): 277-285.
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








