What to Do if My Child Touches Poison Ivy?


Written and verified by the dermatologist Maria del Carmen Hernandez
Children’s contact with poison ivy plants is greatly feared by parents because of the clinical manifestations it often triggers. While it’s not usually serious, it’s important to know the signs and symptoms it causes so that early action can be taken.
What’s poison ivy?
Poison ivy belongs to Toxicodendron, a genus of shrubs, plants, trees, and vines in the family Anacardiaceae. All parts of these plants contain a type of oil called urushiol, which is one of the causes of exposure dermatitis.
Poison ivy usually appears as a vine with almond-shaped leaves in a group of three leaves per cluster. These in turn may change from green to red in the fall. Poison ivy contact dermatitis is one of the most common allergic causes, and is triggered by skin contact with urushiol.
Read also: 10 Tips for Treating Contact Dermatitis in Children
How does the allergic reaction appear?
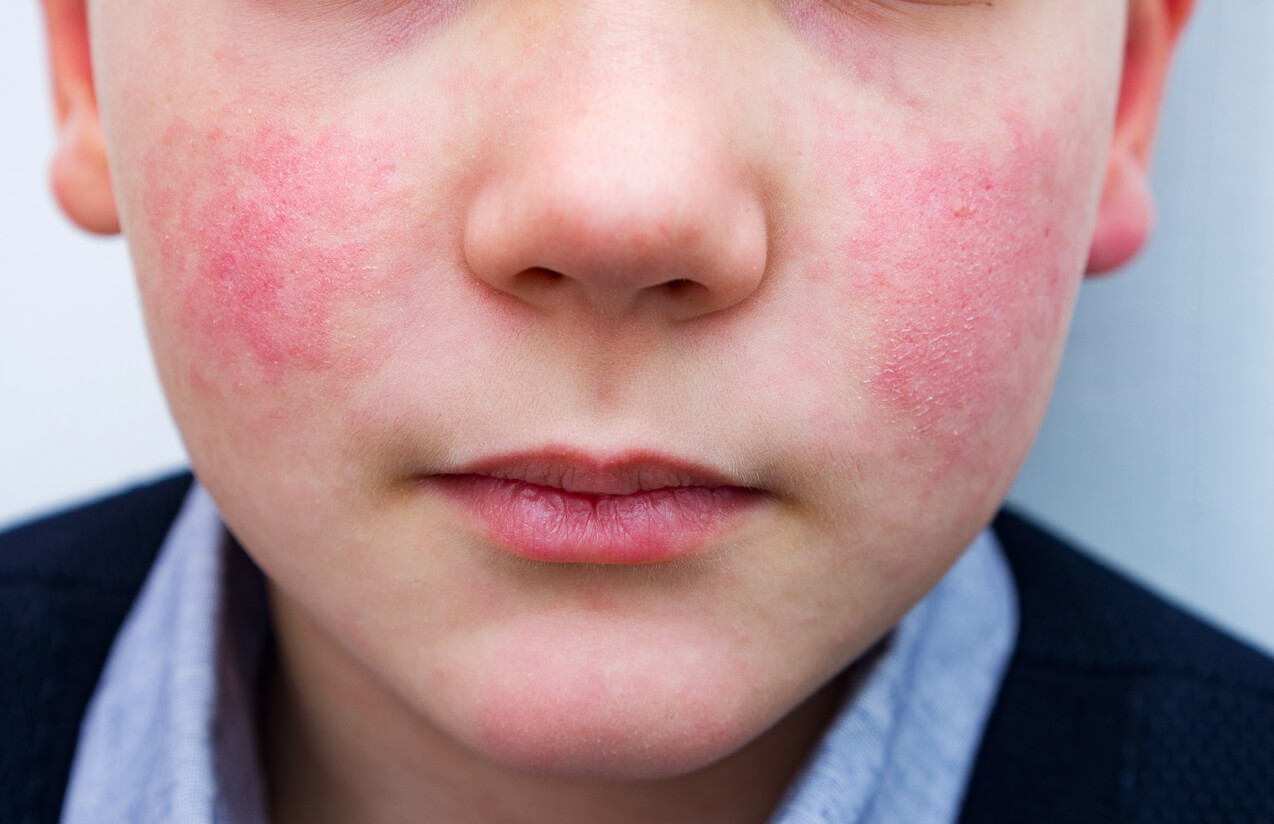
Acute allergic dermatitis is generated when the child comes into contact with the plant. Symptoms caused by poison ivy include the following:
- Edema
- Erythema
- Itching
- Painful blisters
- Vesicles
According to studies published by Archives of Dermatology, these manifestations are usually more acute and appear within 24-72 hours in cases of re-exposure.
What to do if a child has contact with poison ivy?
Occasionally, the resulting dermatitis may be self-limiting and resolve spontaneously within a couple of weeks. However, early action should always be taken to avoid possible complications.
Wash the area
Early management includes quick washing with soap of the area of the body that came in contact with the poison ivy. Keep in mind that the substance is rapidly absorbed because of its lipophilic nature. Therefore, in some cases, this makes further efforts to rinse it off or attempt to remove it ineffective. Nails should also be considered in the post-exposure rinse.
Provide antihistamines
Oral and topical antihistamines are indicated to reduce itching, although they’re not usually very effective. Even lotions with calamine may also be useful to soothe itching.
Administration of antihistamines before bedtime and application of topical creams contribute to the improvement of the clinical picture. On the other hand, scratching the lesions worsens the situation and prolongs the symptoms. An infection may even develop if the skin is injured, which could intensify the itching.
Apply topical and oral corticosteroids
Treatment is based on the use of moderate to high-dose systemic and topical corticosteroids, which are effective at the onset of signs and symptoms. Those children who aren’t candidates for systemic medication may opt for moderate-potency topical corticosteroids.
Glucocorticoids should be indicated with a gradual taper over 2 to 3 weeks and start with 60 mg per day for 5 days. Then taper to 40 mg per day for 5 days, and then to 20 mg per day for 5 days.
Wash clothing
Once the toxic substance has been removed from the skin, the toxicity can’t be transmitted from one person to another or from one region of the body to another, so it’s not contagious. However, contact with urushiol that remains residual on clothing, pets, or tools may trigger new rashes. Therefore, they should be decontaminated after contact with the plant.
You may be interested in: Allergies to Bites and Stings in Infants and Children
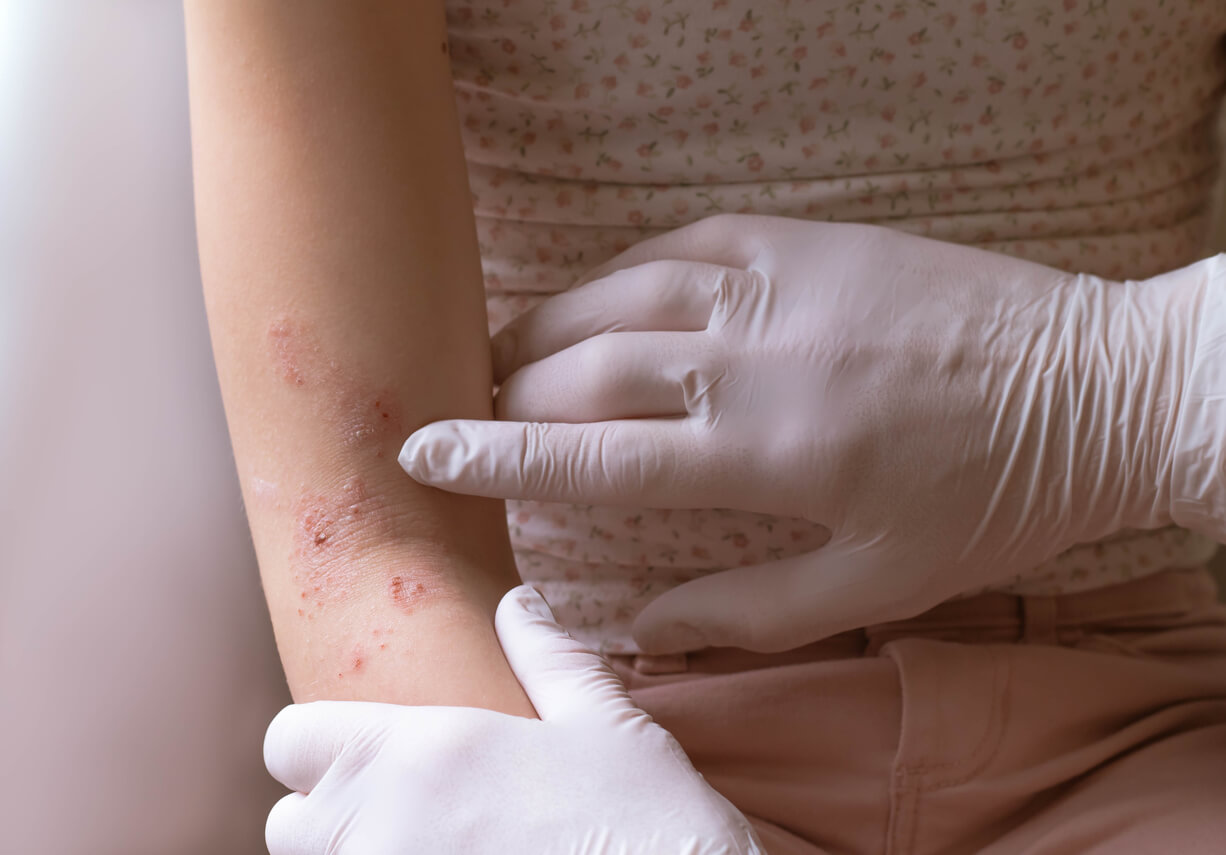
When to see a doctor urgently?
A doctor should be consulted urgently for care in the following cases:
- Difficulty breathing
- Rash on the genitals or face
- Difficulty swallowing
- The rash covers a large proportion of the body
- The areas affected by the rash are swollen
- Elevated temperature
- The lesions don’t improve with treatment
Rare complications include secondary bacterial infection or hyperpigmentation of the skin. Continued and repeated scratching may cause tiny fissures. Consequently, bacteria can use the cracks in the skin to enter and trigger an infection, which should be treated with specific antibiotic medication.
Children and poison ivy exposure
The most important thing is prevention and knowing how to recognize the appearance of the plant to teach the child not to come into contact with it. Poison ivy not only causes skin manifestations but can also have a negative impact on the child’s quality of life, including loss of sleep.
Children’s contact with poison ivy plants is greatly feared by parents because of the clinical manifestations it often triggers. While it’s not usually serious, it’s important to know the signs and symptoms it causes so that early action can be taken.
What’s poison ivy?
Poison ivy belongs to Toxicodendron, a genus of shrubs, plants, trees, and vines in the family Anacardiaceae. All parts of these plants contain a type of oil called urushiol, which is one of the causes of exposure dermatitis.
Poison ivy usually appears as a vine with almond-shaped leaves in a group of three leaves per cluster. These in turn may change from green to red in the fall. Poison ivy contact dermatitis is one of the most common allergic causes, and is triggered by skin contact with urushiol.
Read also: 10 Tips for Treating Contact Dermatitis in Children
How does the allergic reaction appear?
Acute allergic dermatitis is generated when the child comes into contact with the plant. Symptoms caused by poison ivy include the following:
- Edema
- Erythema
- Itching
- Painful blisters
- Vesicles
According to studies published by Archives of Dermatology, these manifestations are usually more acute and appear within 24-72 hours in cases of re-exposure.

What to do if a child has contact with poison ivy?
Occasionally, the resulting dermatitis may be self-limiting and resolve spontaneously within a couple of weeks. However, early action should always be taken to avoid possible complications.
Wash the area
Early management includes quick washing with soap of the area of the body that came in contact with the poison ivy. Keep in mind that the substance is rapidly absorbed because of its lipophilic nature. Therefore, in some cases, this makes further efforts to rinse it off or attempt to remove it ineffective. Nails should also be considered in the post-exposure rinse.
Provide antihistamines
Oral and topical antihistamines are indicated to reduce itching, although they’re not usually very effective. Even lotions with calamine may also be useful to soothe itching.
Administration of antihistamines before bedtime and application of topical creams contribute to the improvement of the clinical picture. On the other hand, scratching the lesions worsens the situation and prolongs the symptoms. An infection may even develop if the skin is injured, which could intensify the itching.
Apply topical and oral corticosteroids
Treatment is based on the use of moderate to high-dose systemic and topical corticosteroids, which are effective at the onset of signs and symptoms. Those children who aren’t candidates for systemic medication may opt for moderate-potency topical corticosteroids.
Glucocorticoids should be indicated with a gradual taper over 2 to 3 weeks and start with 60 mg per day for 5 days. Then taper to 40 mg per day for 5 days, and then to 20 mg per day for 5 days.
Wash clothing
Once the toxic substance has been removed from the skin, the toxicity can’t be transmitted from one person to another or from one region of the body to another, so it’s not contagious. However, contact with urushiol that remains residual on clothing, pets, or tools may trigger new rashes. Therefore, they should be decontaminated after contact with the plant.
You may be interested in: Allergies to Bites and Stings in Infants and Children

When to see a doctor urgently?
A doctor should be consulted urgently for care in the following cases:
- Difficulty breathing
- Rash on the genitals or face
- Difficulty swallowing
- The rash covers a large proportion of the body
- The areas affected by the rash are swollen
- Elevated temperature
- The lesions don’t improve with treatment
Rare complications include secondary bacterial infection or hyperpigmentation of the skin. Continued and repeated scratching may cause tiny fissures. Consequently, bacteria can use the cracks in the skin to enter and trigger an infection, which should be treated with specific antibiotic medication.
Children and poison ivy exposure
The most important thing is prevention and knowing how to recognize the appearance of the plant to teach the child not to come into contact with it. Poison ivy not only causes skin manifestations but can also have a negative impact on the child’s quality of life, including loss of sleep.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Fisher AA. Poison ivy/oak/sumac. Part II: Specific features. Cutis. 1996 Jul;58(1):22-4. PMID: 8823544.
- Williams JV, Light J, Marks JG Jr. Individual variations in allergic contact dermatitis from urushiol. Arch Dermatol. 1999 Aug;135(8):1002-3. doi: 10.1001/archderm.135.8.1002. PMID: 10456367.
- Moe JF. How much steroid for poison ivy? Postgrad Med. 1999 Oct 1;106(4):21, 24. PMID: 10533503.
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








