Erythema Nodosum in Children: Symptoms, Causes and Treatment


Written and verified by the dermatologist Maria del Carmen Hernandez
Erythema nodosum isn’t a pathology in itself, but a manifestation of a disease that causes it. The symptoms are nodules developing on the skin, pain in the joints, and also a high temperature.
It isn’t contagious, and, if its origin isn’t discovered, its treatment is symptomatic and it evolves spontaneously.
What are the causes of erythema nodosum in children?
The causes of this syndrome can be multiple. The Spanish Association of Pediatrics divides them into infectious, non-infectious, and idiopathic etiology.
Non-infectious causes
- Bacterial: streptococcal infections, tuberculosis, leprosy, Mycoplasma pneumonia, Yersinia, Salmonella, Campylobacter, Tularemia, Bartonella (cat scratch disease), nyptospirosis, psittacosis, brucellosis, lymphogranuloma venereum, rickettsia and shigella
- Viral: infectious mononucleosis, hepatitis B, hepatitis C, HIV, Epstein-Barr virus, herpes simplex virus
- Fungi: Coccidioidomycosis, Blastomycosis, Histoplasmosis, tinea
- Parasites: amebiasis, giardiasis
The infectious cause is the most common one to occur during childhood, and so that should be the first one to rule out.
Read also: How to Treat Blisters in Children
Idiopathic causes
This type of origin is one in which doctors can’t identify any apparent cause. In turn, about 50% of cases are idiopathic, or primary, erythema nodosum according to published reviews.
The treatment of this variant is, therefore, to administer non-steroidal anti-inflammatory drugs to relieve the discomfort.
Infectious causes
Drugs: antibiotics (sulfonamides and penicillins)
- Various drugs: oral contraceptives, bromides, iodides, TNF-alpha inhibitor
- Malignancy: leukemia, lymphoma, occult neoplasms
- Inflammatory bowel disease: Crohn’s disease, ulcerative colitis
- Miscellaneous: pregnancy, Behcet’s disease, Whipple’s disease, sarcoidosis-Lofgren’s syndrome (a triad of erythema nodosum, acute arthritis and hilar lymphadenopathy)
Symptoms of erythema nodosum in children
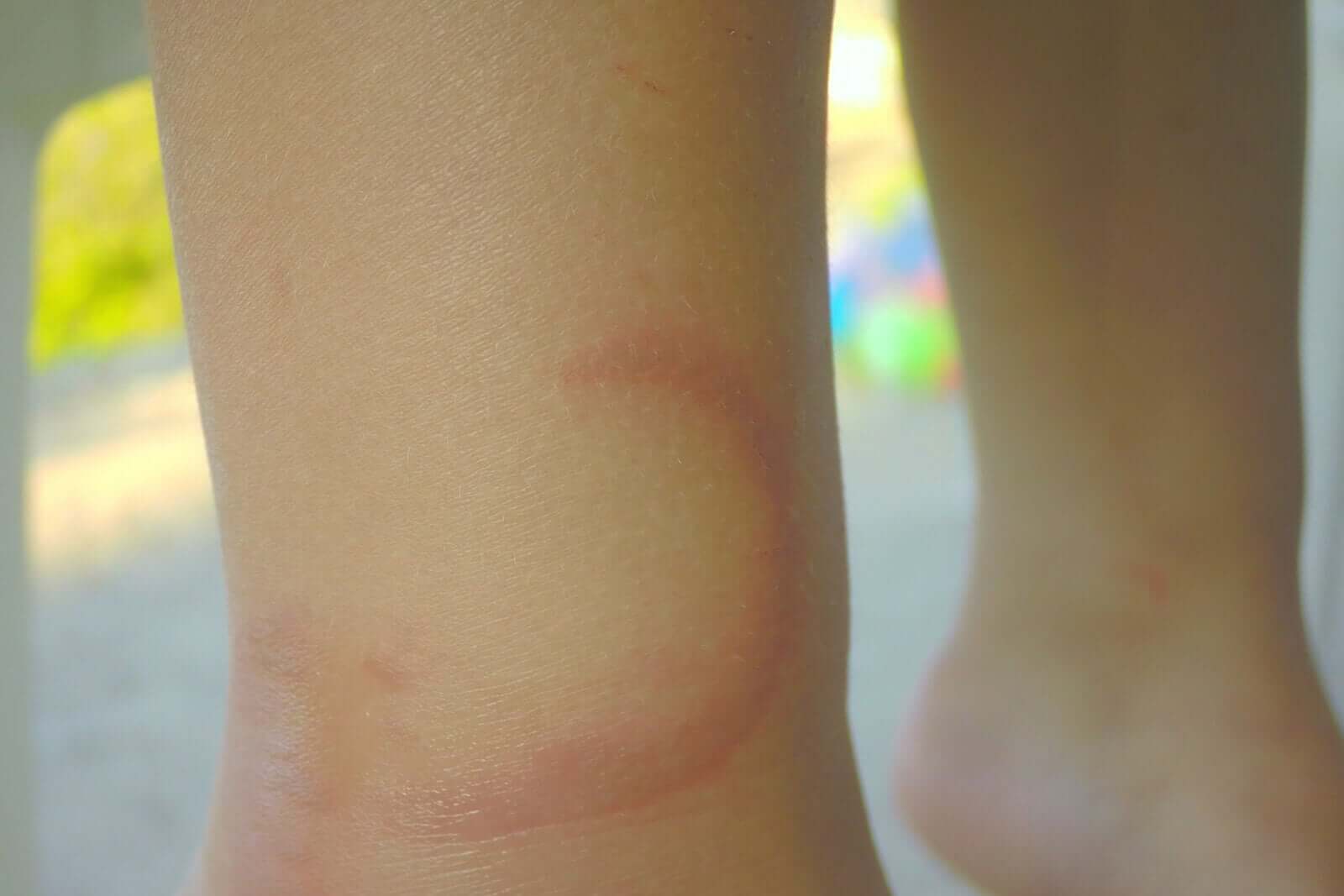
Erythema nodosum is a syndrome characterized by an acute nodular, erythematous rash that most frequently appears in the area of the leg extensor muscles. It can also appear on the forearms, arms, thighs, and other parts of the body.
It can develop idiopathically or be linked to other systemic pathologies. The nodules are firm and appear suddenly. They’re painful and deep to the touch. When it affects children, there’s no gender predilection.
The evolution of the disease
Although it differs as regards to the causative agent, the disease always develops following the same evolutionary pattern. However, it never results in processes of necrosis, scarring, or ulceration.
Prodromal phase
This is a non-specific period of time that may last from 3 to 6 days. In turn, this stage is characterized by high temperatures, pain in the larger joints in the lower extremities, or abdominal pain. A nasopharyngeal infection usually develops, in addition to slightly affecting the child’s general health condition.
Stage phase
The disease stage consolidates in only 1 or 2 days. In addition, the predominant symptom is fever, along with the joint pain that’ll persist, or even increase, from the previous stage.
Nodules of 1 to 3 cm (0.4 – 2.2 inches) in diameter begin to appear on the extensor area of the legs, thighs, knees, and forearms. The nodules can be characterized as follows:
- Small
- Bilateral
- Symmetrical
- Reddish
- Burning
- Superelevated
Sometimes, there can be hilar adenopathy, edema in the ankles, and pain in the area of the rash. This can force the patient to have to lie down and raise their legs to avoid the discomfort.
Regressive phase
Erythema nodosum evolves, and resolves itself, spontaneously, but this process can be accelerated with treatment of the symptoms or with rest.
You may like to read: How to Prevent and Treat Diaper Rash
How do doctors diagnose it?
Erythema nodosum is diagnosed with the specific skin manifestations on the child. In turn, the physician may request complementary studies such as the following:
- Complete blood test
- Chest X-ray
- Rapid streptococcus test
- Mantoux test
The biopsy of the lesion is only carried out when the child’s symptoms aren’t typical.
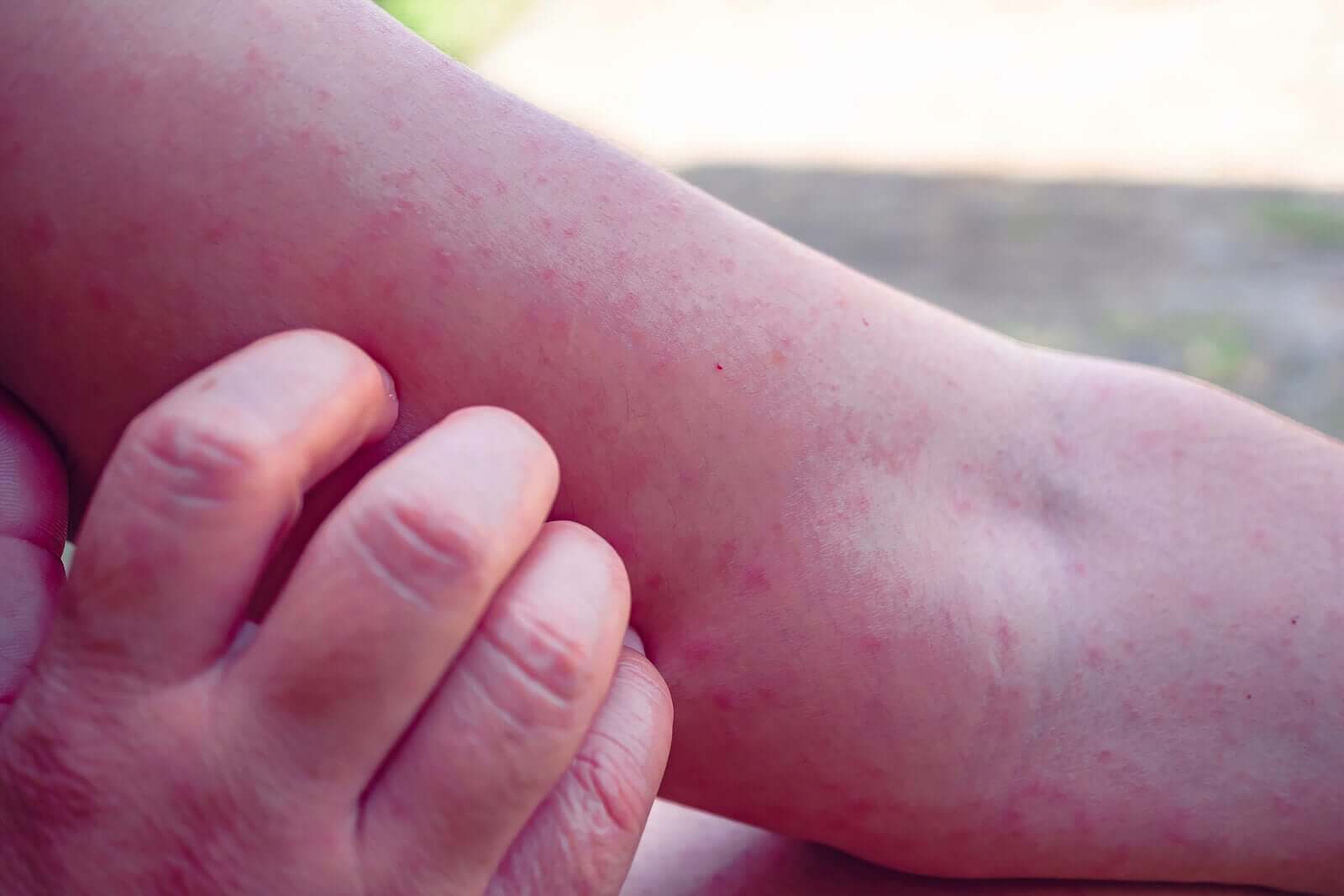
Therapeutic options for erythema nodosum in children
The treatment of erythema nodosum in children resolves itself naturally. However, it may require the child to rest, and also raise their lower limbs, or other measures to minimize symptoms.
Unlike adults, venous compression to reduce pain isn’t recommended in children. In contrast, etiological treatment is essential in certain cases. NSAID analgesics (non-steroidal anti-inflammatory drugs) and paracetamol are part of the preferred treatment to greatly reduce symptoms.
Erythema nodosum and its evolution
In most cases, erythema nodosum in children has a good prognosis. However, the skin lesions usually take months to heal naturally. Thankfully, they don’t leave scars or hyperpigmented macules.
More severe cases of erythema nodosum take much longer to resolve. In turn, one third of patients may have recurrences.
Erythema nodosum isn’t a pathology in itself, but a manifestation of a disease that causes it. The symptoms are nodules developing on the skin, pain in the joints, and also a high temperature.
It isn’t contagious, and, if its origin isn’t discovered, its treatment is symptomatic and it evolves spontaneously.
What are the causes of erythema nodosum in children?
The causes of this syndrome can be multiple. The Spanish Association of Pediatrics divides them into infectious, non-infectious, and idiopathic etiology.
Non-infectious causes
- Bacterial: streptococcal infections, tuberculosis, leprosy, Mycoplasma pneumonia, Yersinia, Salmonella, Campylobacter, Tularemia, Bartonella (cat scratch disease), nyptospirosis, psittacosis, brucellosis, lymphogranuloma venereum, rickettsia and shigella
- Viral: infectious mononucleosis, hepatitis B, hepatitis C, HIV, Epstein-Barr virus, herpes simplex virus
- Fungi: Coccidioidomycosis, Blastomycosis, Histoplasmosis, tinea
- Parasites: amebiasis, giardiasis

The infectious cause is the most common one to occur during childhood, and so that should be the first one to rule out.
Read also: How to Treat Blisters in Children
Idiopathic causes
This type of origin is one in which doctors can’t identify any apparent cause. In turn, about 50% of cases are idiopathic, or primary, erythema nodosum according to published reviews.
The treatment of this variant is, therefore, to administer non-steroidal anti-inflammatory drugs to relieve the discomfort.
Infectious causes
Drugs: antibiotics (sulfonamides and penicillins)
- Various drugs: oral contraceptives, bromides, iodides, TNF-alpha inhibitor
- Malignancy: leukemia, lymphoma, occult neoplasms
- Inflammatory bowel disease: Crohn’s disease, ulcerative colitis
- Miscellaneous: pregnancy, Behcet’s disease, Whipple’s disease, sarcoidosis-Lofgren’s syndrome (a triad of erythema nodosum, acute arthritis and hilar lymphadenopathy)
Symptoms of erythema nodosum in children
Erythema nodosum is a syndrome characterized by an acute nodular, erythematous rash that most frequently appears in the area of the leg extensor muscles. It can also appear on the forearms, arms, thighs, and other parts of the body.
It can develop idiopathically or be linked to other systemic pathologies. The nodules are firm and appear suddenly. They’re painful and deep to the touch. When it affects children, there’s no gender predilection.
The evolution of the disease
Although it differs as regards to the causative agent, the disease always develops following the same evolutionary pattern. However, it never results in processes of necrosis, scarring, or ulceration.
Prodromal phase
This is a non-specific period of time that may last from 3 to 6 days. In turn, this stage is characterized by high temperatures, pain in the larger joints in the lower extremities, or abdominal pain. A nasopharyngeal infection usually develops, in addition to slightly affecting the child’s general health condition.
Stage phase
The disease stage consolidates in only 1 or 2 days. In addition, the predominant symptom is fever, along with the joint pain that’ll persist, or even increase, from the previous stage.
Nodules of 1 to 3 cm (0.4 – 2.2 inches) in diameter begin to appear on the extensor area of the legs, thighs, knees, and forearms. The nodules can be characterized as follows:
- Small
- Bilateral
- Symmetrical
- Reddish
- Burning
- Superelevated
Sometimes, there can be hilar adenopathy, edema in the ankles, and pain in the area of the rash. This can force the patient to have to lie down and raise their legs to avoid the discomfort.
Regressive phase
Erythema nodosum evolves, and resolves itself, spontaneously, but this process can be accelerated with treatment of the symptoms or with rest.
You may like to read: How to Prevent and Treat Diaper Rash
How do doctors diagnose it?
Erythema nodosum is diagnosed with the specific skin manifestations on the child. In turn, the physician may request complementary studies such as the following:
- Complete blood test
- Chest X-ray
- Rapid streptococcus test
- Mantoux test
The biopsy of the lesion is only carried out when the child’s symptoms aren’t typical.

Therapeutic options for erythema nodosum in children
The treatment of erythema nodosum in children resolves itself naturally. However, it may require the child to rest, and also raise their lower limbs, or other measures to minimize symptoms.
Unlike adults, venous compression to reduce pain isn’t recommended in children. In contrast, etiological treatment is essential in certain cases. NSAID analgesics (non-steroidal anti-inflammatory drugs) and paracetamol are part of the preferred treatment to greatly reduce symptoms.
Erythema nodosum and its evolution
In most cases, erythema nodosum in children has a good prognosis. However, the skin lesions usually take months to heal naturally. Thankfully, they don’t leave scars or hyperpigmented macules.
More severe cases of erythema nodosum take much longer to resolve. In turn, one third of patients may have recurrences.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Leung AKC, Leong KF, Lam JM. Erythema nodosum. World J Pediatr. 2018 Dec;14(6):548-554. doi: 10.1007/s12519-018-0191-1. Epub 2018 Sep 29. PMID: 30269303.
- Scarpa R, Scognamiglio A, Casaburo G, Oriente A, Biondi Oriente C, Oriente P. L’eritema nodoso: epidemiologia, etiologia, patogenesi, quadro clinico e terapia [Erythema nodosum: epidemiology, etiology, pathogenesis, clinical picture and therapy]. Recenti Prog Med. 1989 Nov;80(11):615-20. Italian. PMID: 2696021.
- Requena L, Sánchez Yus E. Erythema nodosum. Semin Cutan Med Surg. 2007 Jun;26(2):114-25. doi: 10.1016/j.sder.2007.02.009. PMID: 17544964.
- Faulkes RE. Upper limb erythema nodosum: the first presentation of Crohn’s disease. Clin Case Rep. 2014 Oct;2(5):183-5. doi: 10.1002/ccr3.87. Epub 2014 Jun 30. PMID: 25614807; PMCID: PMC4302621.
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








