10 Skin Conditions Due to Autoimmune Diseases


Written and verified by the dermatologist Maria del Carmen Hernandez
The skin is the largest organ of the body and acts as a protective barrier against the external environment. However, in certain cases, the immune system can trigger an overactive response and target the body’s own tissues. These conditions, known as autoimmune diseases, can affect various organs, including the skin.
In this article, we’ll tell you about some of the most common autoimmune skin conditions and their treatments. Keep reading to the end to learn more.
Skin diseases associated with autoimmune disorders
Autoimmune skin diseases can manifest themselves in a variety of ways, from rashes and blisters to pigmentation changes and hardening of the skin. These conditions can cause significant discomfort and affect quality of life. Below, you’ll learn about the ten most common.
1. Systemic Lupus Erythematosus (SLE)
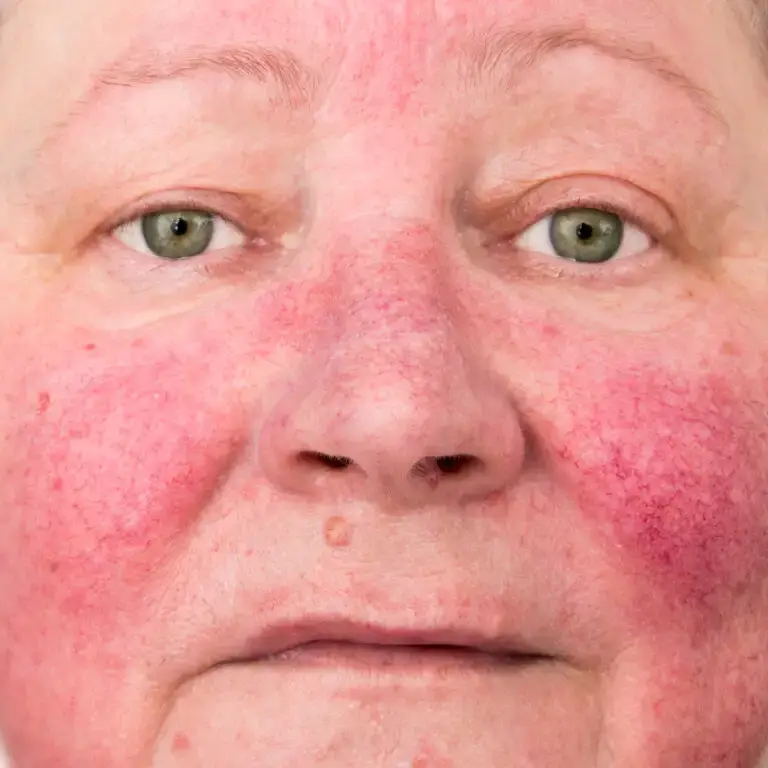
SLE is a chronic autoimmune disease that can affect different body systems, including the skin. In fact, it’s possible to experience a butterfly wing rash on the face.
Skin lesions may also occur on other areas of the body and worsen with sun exposure. Therefore, it’s important to protect yourself by wearing broad-spectrum sunscreen and protective clothing.
Treatments may include topical or oral corticosteroids to reduce inflammation and relieve skin symptoms. Immunosuppressants may also be indicated to control the excessive immune response.
2. Dermatomyositis

Dermatomyositis is an autoimmune disease that causes inflammation of the muscles and skin. Skin symptoms include red or purple rashes on the cheeks, shoulders, and chest area.
Muscle weakness may also be seen. Oral or injectable corticosteroids are often used to reduce inflammation and improve skin symptoms. In some cases, additional immunosuppressants are indicated to control the autoimmune response.
3. Scleroderma
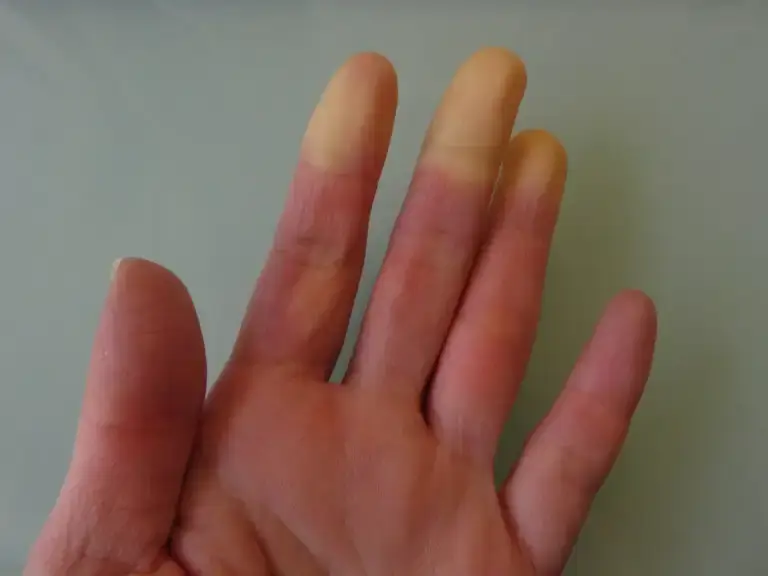
Scleroderma is an autoimmune disease that causes hardening and thickening of the skin. Hard patches may also develop on the skin surface that can affect the hands, face, and other parts of the body. They can also cause dry, itchy skin.
The U.S. National Library of Medicine notes that while there’s no cure, medications can be prescribed to control symptoms and prevent complications. Creams and ointments that help moisturize dry skin and relieve itching are useful. Even managing body temperature and avoiding cold temperatures are recommended to prevent cutaneous vasoconstriction.
4. Pemphigus vulgaris
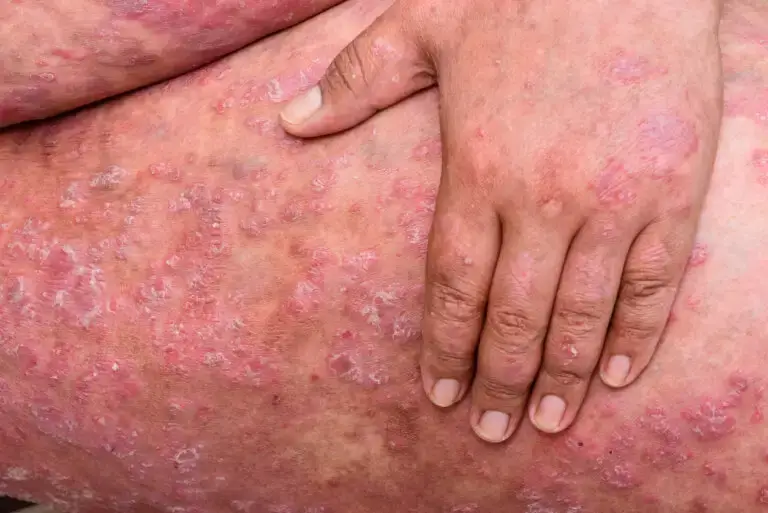
Pemphigus vulgaris is an autoimmune disease that causes painful blisters on the skin and mucous membranes. These are prone to rupture easily.
Patients with pemphigus vulgaris require intense medical treatment involving the use of corticosteroids and other immunosuppressive drugs. Antibiotics may also be prescribed to prevent infections in the blisters. Therefore, blister care and close follow-up with the physician are critical.
5. Psoriasis

According to a study published in the Indian Dermatology Online Journal, psoriasis is one of the chronic autoimmune diseases that affects the skin. It’s characterized by the appearance of red, inflamed, silvery, and scaly patches on the surface of the skin.
These patches can be itchy and cause discomfort for patients. In these cases, treatments may include topical corticosteroids, phototherapy, oral or injectable medications, and targeted therapies.
In addition, it’s important to keep the skin hydrated and avoid known triggers, such as stress and certain foods.
6. Vitiligo

Vitiligo is a fairly common skin disease of autoimmune origin in which pigment cells in the skin are attacked by the immune system. This results in the loss of pigment and the appearance of white patches.
This condition can affect any part of the body and have a significant impact on a patient’s quality of life due to embarrassment and the increased risk of sunburn. Also, treatment may include topical steroid creams or ointments, ultraviolet light therapy (PUVA), and immunomodulatory medications.
7. Dermatitis herpetiformis
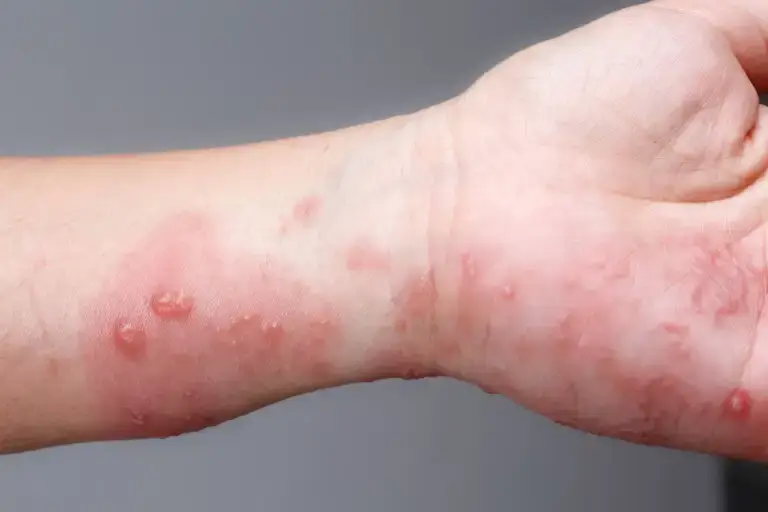
Dermatitis herpetiformis is a skin condition related to celiac disease, which is an autoimmune disease triggered by gluten. It’s characterized by blisters and very itchy skin lesions, usually appearing on knees, elbows, and buttocks.
The main treatment involves a gluten-free diet to control the underlying celiac disease. Topical or systemic medications may also be prescribed to alleviate skin symptoms. An article published in the American Journal of Clinical Dermatology recommends avoiding gluten in the diet in order to avoid this disease and reading food labels carefully.
8. Lichen planus
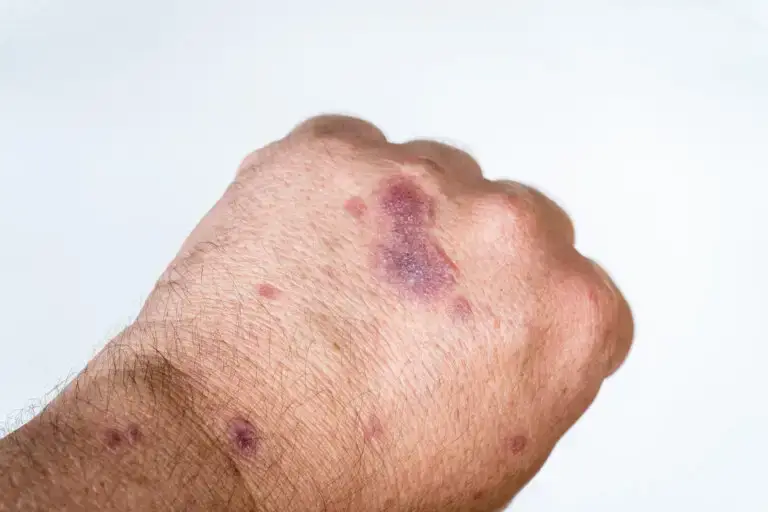
Lichen planus is an autoimmune disease that affects the skin, mucous membranes, and sometimes the nails. It appears in the form of small, flat, red, or purplish bumps on the skin, which may cause itching and discomfort.
It may resolve on its own or persist for a long time. In these cases, topical or oral corticosteroids are often used to reduce inflammation and relieve symptoms. In addition, it’s important to avoid stress and resort to antihistamine drugs to control itching.
9. Sjogren’s syndrome
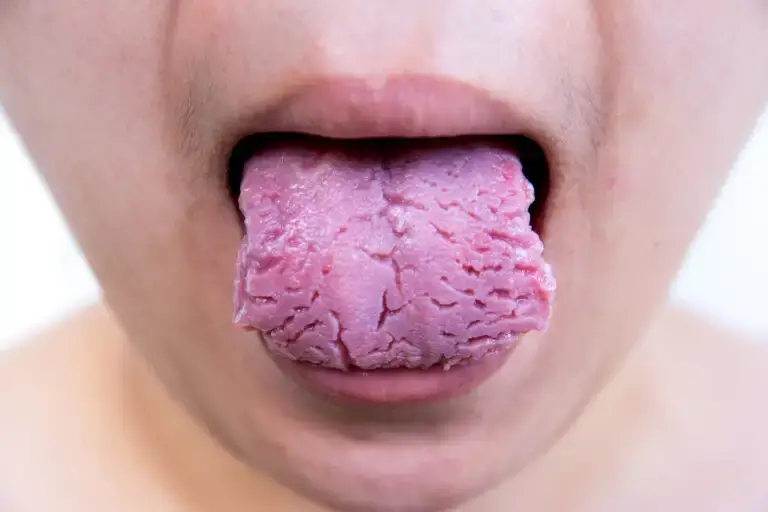
Sjogren’s syndrome is an autoimmune disease that affects the exocrine glands, such as the salivary and lacrimal glands. An article published in the journal Clinical and Experimental Medicine describes that you may experience dry skin and develop a characteristic skin rash called patchy erythema.
Treatment focuses on relieving symptoms, such as dry skin, with moisturizers and eye lubricants. In turn, drugs to stimulate saliva and tear production may be indicated.
10. Thrombotic thrombocytopenic purpura (TTP)
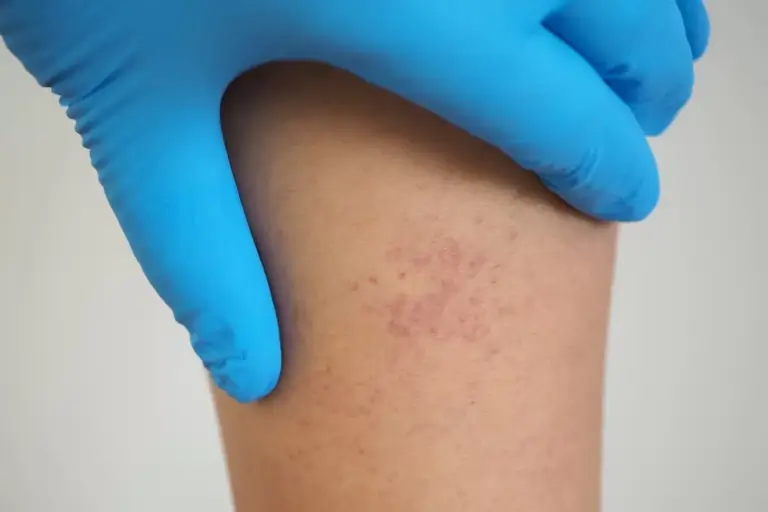
TTP is a rare but serious autoimmune disease characterized by blood clots in small blood vessels throughout the body.
These clots can affect the skin and cause red or purple spots as well as blisters or ulcers. For this, treatment usually requires plasma replacement therapy and platelet transfusions. In addition, the use of immunosuppressants may reduce the autoimmune response.
Autoimmune skin conditions and consultation
It’s important to seek appropriate medical care for accurate diagnosis and treatment if autoimmune skin disease is suspected. As a result, treatments and recommendations may vary depending on the severity of the condition and the individual patient’s response.
A comprehensive approach involving dermatologists and other specialists can help improve symptoms and provide appropriate management for those with these autoimmune skin conditions.
The skin is the largest organ of the body and acts as a protective barrier against the external environment. However, in certain cases, the immune system can trigger an overactive response and target the body’s own tissues. These conditions, known as autoimmune diseases, can affect various organs, including the skin.
In this article, we’ll tell you about some of the most common autoimmune skin conditions and their treatments. Keep reading to the end to learn more.
Skin diseases associated with autoimmune disorders
Autoimmune skin diseases can manifest themselves in a variety of ways, from rashes and blisters to pigmentation changes and hardening of the skin. These conditions can cause significant discomfort and affect quality of life. Below, you’ll learn about the ten most common.
1. Systemic Lupus Erythematosus (SLE)

SLE is a chronic autoimmune disease that can affect different body systems, including the skin. In fact, it’s possible to experience a butterfly wing rash on the face.
Skin lesions may also occur on other areas of the body and worsen with sun exposure. Therefore, it’s important to protect yourself by wearing broad-spectrum sunscreen and protective clothing.
Treatments may include topical or oral corticosteroids to reduce inflammation and relieve skin symptoms. Immunosuppressants may also be indicated to control the excessive immune response.
2. Dermatomyositis

Dermatomyositis is an autoimmune disease that causes inflammation of the muscles and skin. Skin symptoms include red or purple rashes on the cheeks, shoulders, and chest area.
Muscle weakness may also be seen. Oral or injectable corticosteroids are often used to reduce inflammation and improve skin symptoms. In some cases, additional immunosuppressants are indicated to control the autoimmune response.
3. Scleroderma

Scleroderma is an autoimmune disease that causes hardening and thickening of the skin. Hard patches may also develop on the skin surface that can affect the hands, face, and other parts of the body. They can also cause dry, itchy skin.
The U.S. National Library of Medicine notes that while there’s no cure, medications can be prescribed to control symptoms and prevent complications. Creams and ointments that help moisturize dry skin and relieve itching are useful. Even managing body temperature and avoiding cold temperatures are recommended to prevent cutaneous vasoconstriction.
4. Pemphigus vulgaris

Pemphigus vulgaris is an autoimmune disease that causes painful blisters on the skin and mucous membranes. These are prone to rupture easily.
Patients with pemphigus vulgaris require intense medical treatment involving the use of corticosteroids and other immunosuppressive drugs. Antibiotics may also be prescribed to prevent infections in the blisters. Therefore, blister care and close follow-up with the physician are critical.
5. Psoriasis

According to a study published in the Indian Dermatology Online Journal, psoriasis is one of the chronic autoimmune diseases that affects the skin. It’s characterized by the appearance of red, inflamed, silvery, and scaly patches on the surface of the skin.
These patches can be itchy and cause discomfort for patients. In these cases, treatments may include topical corticosteroids, phototherapy, oral or injectable medications, and targeted therapies.
In addition, it’s important to keep the skin hydrated and avoid known triggers, such as stress and certain foods.
6. Vitiligo

Vitiligo is a fairly common skin disease of autoimmune origin in which pigment cells in the skin are attacked by the immune system. This results in the loss of pigment and the appearance of white patches.
This condition can affect any part of the body and have a significant impact on a patient’s quality of life due to embarrassment and the increased risk of sunburn. Also, treatment may include topical steroid creams or ointments, ultraviolet light therapy (PUVA), and immunomodulatory medications.
7. Dermatitis herpetiformis

Dermatitis herpetiformis is a skin condition related to celiac disease, which is an autoimmune disease triggered by gluten. It’s characterized by blisters and very itchy skin lesions, usually appearing on knees, elbows, and buttocks.
The main treatment involves a gluten-free diet to control the underlying celiac disease. Topical or systemic medications may also be prescribed to alleviate skin symptoms. An article published in the American Journal of Clinical Dermatology recommends avoiding gluten in the diet in order to avoid this disease and reading food labels carefully.
8. Lichen planus

Lichen planus is an autoimmune disease that affects the skin, mucous membranes, and sometimes the nails. It appears in the form of small, flat, red, or purplish bumps on the skin, which may cause itching and discomfort.
It may resolve on its own or persist for a long time. In these cases, topical or oral corticosteroids are often used to reduce inflammation and relieve symptoms. In addition, it’s important to avoid stress and resort to antihistamine drugs to control itching.
9. Sjogren’s syndrome

Sjogren’s syndrome is an autoimmune disease that affects the exocrine glands, such as the salivary and lacrimal glands. An article published in the journal Clinical and Experimental Medicine describes that you may experience dry skin and develop a characteristic skin rash called patchy erythema.
Treatment focuses on relieving symptoms, such as dry skin, with moisturizers and eye lubricants. In turn, drugs to stimulate saliva and tear production may be indicated.
10. Thrombotic thrombocytopenic purpura (TTP)

TTP is a rare but serious autoimmune disease characterized by blood clots in small blood vessels throughout the body.
These clots can affect the skin and cause red or purple spots as well as blisters or ulcers. For this, treatment usually requires plasma replacement therapy and platelet transfusions. In addition, the use of immunosuppressants may reduce the autoimmune response.
Autoimmune skin conditions and consultation
It’s important to seek appropriate medical care for accurate diagnosis and treatment if autoimmune skin disease is suspected. As a result, treatments and recommendations may vary depending on the severity of the condition and the individual patient’s response.
A comprehensive approach involving dermatologists and other specialists can help improve symptoms and provide appropriate management for those with these autoimmune skin conditions.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Negrini, S., Emmi, G., Greco, M., Borro, M., Sardanelli, F., Murdaca, G., Indiveri, F., & Puppo, F. (2022). Sjögren’s syndrome: a systemic autoimmune disease. Clinical and experimental medicine, 22(1), 9–25. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8863725/
- Odonwodo, A., Badri, T., Hariz, A. (2022) Scleroderma. StatPearls. National Library of Medicine. https://www.ncbi.nlm.nih.gov/books/NBK537335/
-
Reunala, T., Hervonen, K., & Salmi, T. (2021). Dermatitis Herpetiformis: An Update on Diagnosis and Management. American journal of clinical dermatology, 22(3), 329–338. https://pubmed.ncbi.nlm.nih.gov/33432477/
-
Vashist, S., Mahajan, V. K., Mehta, K. S., Chauhan, P. S., Yadav, R. S., Sharma, S. B., Sharma, V., Sharma, A., Chowdhary, B., & Kumar, P. (2020). Association of Psoriasis with Autoimmune Disorders: Results of a Pilot Study. Indian dermatology online journal, 11(5), 753–759. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7678535/
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








