Juvenile Plantar Dermatitis: What You Should Know


Written and verified by the dermatologist Maria del Carmen Hernandez
Juvenile plantar dermatitis is one of the most frequent conditions related to atopic dermatitis. It’s observed with greater prevalence between the ages of 3 and 15, as the Spanish Association of Pediatrics indicates.
It’s characterized by the inflammation of the soles of the foot and, to a lesser extent, the palms of the hand. In addition, itching is usually so intense that we should differentiate it from tinea pedis (athlete’s foot) and palmar psoriasis.
What are the causes of juvenile plantar dermatitis?
Juvenile plantar dermatosis is more prevalent in those who have a history of atopic dermatitis. In addition, it occurs more frequently in children, and sufferers have an average age of 8. Some of the suggested causes are the following:
- Constant friction movements.
- Excessive sweating, also called hyperhidrosis, can cause the foot to remain in a humid condition.
- Occlusive shoes, especially those made of synthetic materials, plastic or waterproof.
- Genetic predisposition and hypersensitivity of the skin.
- Seasonal changes. We can observe aggravation in the summer months due to excessive sweating and heat, and in the winter months due to the use of closed shoes.
You may like to read: Allergies to Sweat in Children: Symptoms and Treatment
Manifestations of juvenile plantar dermatitis
As its name indicates, juvenile plantar dermatitis affects the soles of the feet, except for the plantar arch and between the toes. It usually appears in a bilateral and symmetrical way and, sometimes, as evidenced by this study published in Acta Dermato-Venereologica, it affects the palms of the hands and the fingertips.
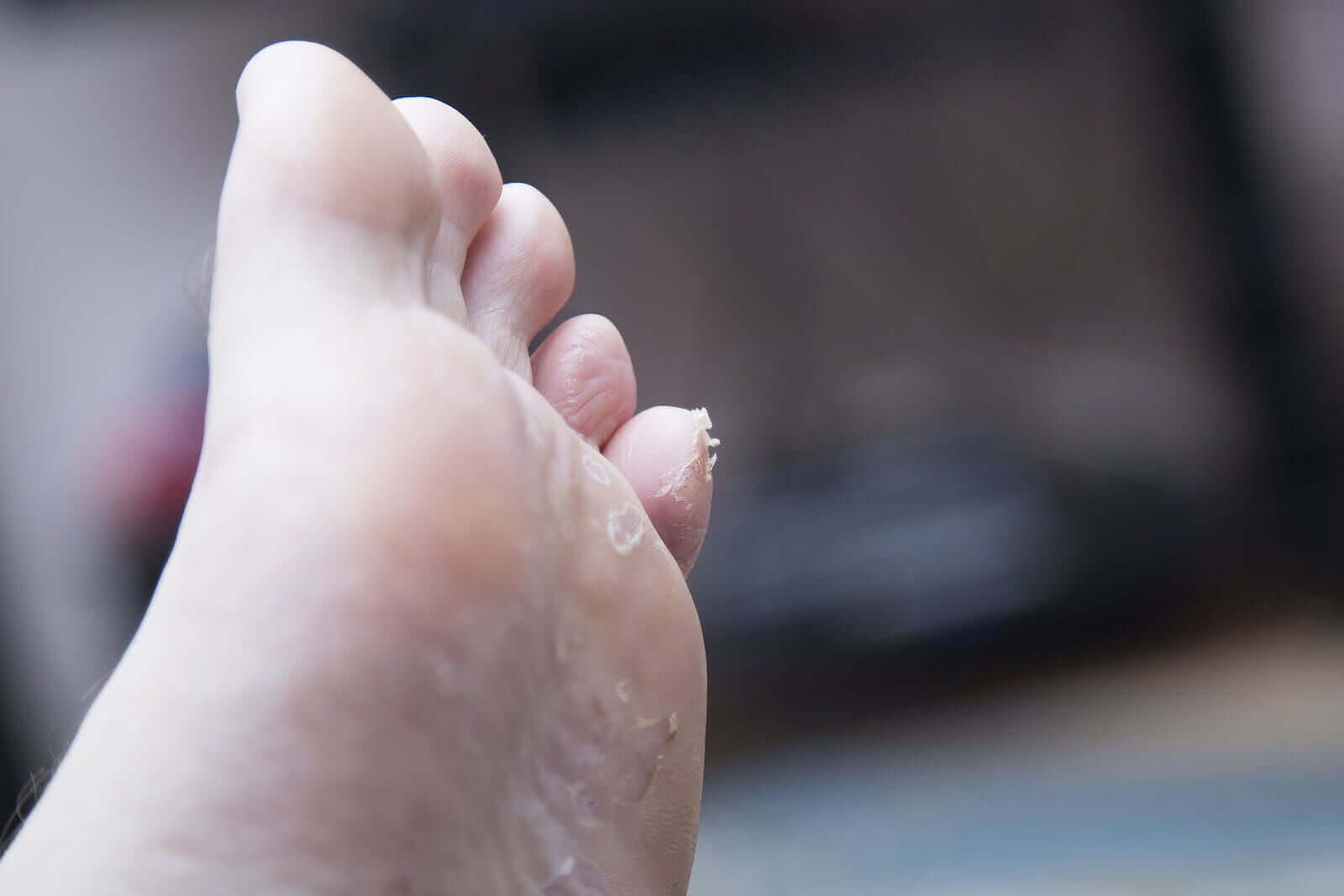
The skin becomes red, shiny, painful and itches constantly. This leads to intense scratching. In addition, this type of injury doesn’t involve secretion, but a moderate peeling of the affected regions is observed.
Sometimes painful fissures and cracks abound, and these are aggravated by the humidity and excessive sweating typical of the affected foot.
Complications of juvenile plantar dermatitis
The most frequent complications that can develop during juvenile plantar dermatitis are skin cracks and painful fissures. These can take weeks or even months to heal and regenerate the epithelium completely.
Sometimes, when there isn’t adequate hygiene, there may be a secondary bacterial infection in the skin. In cases where the skin involvement extends to the periungual area, you may observe nail dystrophy in the future.
Ruling out differential diagnoses
The clinical manifestations of juvenile plantar dermatitis are similar to other dermatological conditions. For this reason, when making a diagnosis, we should rule out the following conditions:
- Psoriasis palmo-plantar
- Palmo-plantar dyshidrosis
- Atopic dermatitis
- Ringworm of the foot
- Allergic contact dermatitis
- Exfoliative keratolysis
In the case of doubts at the time of diagnosis, doctors may use a mycological examination to rule out other diagnostic possibilities.
Read also: 4 Remedies Against Psoriasis for Children
How to make the diagnosis
The dermatologist is responsible for making the diagnosis of juvenile plantar dermatitis. Therefore, the findings, based on the outward signs in the patient, are those that will determine the pathology.
In the case of requiring some type of diagnostic examination, doctors may perform skin scrapings in order to rule out a mycological cause. To rule out contact dermatitis, doctors can carry out the patch test. Doctors don’t usually require a biopsy for this type of pathology.
What are the treatment options?
There’s no specific treatment for juvenile plantar dermatitis. In fact, it’s a condition that, even if the problem is resolved, tends to recur at some point.
Reducing footwear friction
You should always use the correct shoe size and use 100% breathable cotton socks, since synthetics don’t help to solve the problem at all.
Whenever possible, try not to keep sports shoes on too long, especially after perspiring. Where perspiration is excessive, we recommend that you change socks regularly, to avoid the formation of a humid environment.
Moisturize the skin
In a similar way to all conditions with an atopic origin, we recommend, as a first line of treatment, that you also habitually and constantly moisturize the skin.
After each bath or shower, or before going to bed, the skin should be correctly moisturized. In fact, you can use creams with petroleum jelly or urea for the plantar and heel areas.
Prescription creams
When there are cracks and fissures, the use of tacrolimus or corticosteroid based ointments can be very useful. Topical corticosteroids are compounds that you shouldn’t use for more than 10 days, nor should you use them regularly. This is due to the skin getting used to it too easily (thus reducing its effectiveness), and also its adverse effects with prolonged use.
However, it’s always advisable to consult a skin specialist, who’ll be able to resolve any questions you may have, and provide a diagnosis and treatment appropriate to each case.
Juvenile plantar dermatitis is one of the most frequent conditions related to atopic dermatitis. It’s observed with greater prevalence between the ages of 3 and 15, as the Spanish Association of Pediatrics indicates.
It’s characterized by the inflammation of the soles of the foot and, to a lesser extent, the palms of the hand. In addition, itching is usually so intense that we should differentiate it from tinea pedis (athlete’s foot) and palmar psoriasis.
What are the causes of juvenile plantar dermatitis?
Juvenile plantar dermatosis is more prevalent in those who have a history of atopic dermatitis. In addition, it occurs more frequently in children, and sufferers have an average age of 8. Some of the suggested causes are the following:

- Constant friction movements.
- Excessive sweating, also called hyperhidrosis, can cause the foot to remain in a humid condition.
- Occlusive shoes, especially those made of synthetic materials, plastic or waterproof.
- Genetic predisposition and hypersensitivity of the skin.
- Seasonal changes. We can observe aggravation in the summer months due to excessive sweating and heat, and in the winter months due to the use of closed shoes.
You may like to read: Allergies to Sweat in Children: Symptoms and Treatment
Manifestations of juvenile plantar dermatitis
As its name indicates, juvenile plantar dermatitis affects the soles of the feet, except for the plantar arch and between the toes. It usually appears in a bilateral and symmetrical way and, sometimes, as evidenced by this study published in Acta Dermato-Venereologica, it affects the palms of the hands and the fingertips.
The skin becomes red, shiny, painful and itches constantly. This leads to intense scratching. In addition, this type of injury doesn’t involve secretion, but a moderate peeling of the affected regions is observed.
Sometimes painful fissures and cracks abound, and these are aggravated by the humidity and excessive sweating typical of the affected foot.
Complications of juvenile plantar dermatitis
The most frequent complications that can develop during juvenile plantar dermatitis are skin cracks and painful fissures. These can take weeks or even months to heal and regenerate the epithelium completely.
Sometimes, when there isn’t adequate hygiene, there may be a secondary bacterial infection in the skin. In cases where the skin involvement extends to the periungual area, you may observe nail dystrophy in the future.
Ruling out differential diagnoses
The clinical manifestations of juvenile plantar dermatitis are similar to other dermatological conditions. For this reason, when making a diagnosis, we should rule out the following conditions:
- Psoriasis palmo-plantar
- Palmo-plantar dyshidrosis
- Atopic dermatitis
- Ringworm of the foot
- Allergic contact dermatitis
- Exfoliative keratolysis
In the case of doubts at the time of diagnosis, doctors may use a mycological examination to rule out other diagnostic possibilities.
Read also: 4 Remedies Against Psoriasis for Children
How to make the diagnosis
The dermatologist is responsible for making the diagnosis of juvenile plantar dermatitis. Therefore, the findings, based on the outward signs in the patient, are those that will determine the pathology.
In the case of requiring some type of diagnostic examination, doctors may perform skin scrapings in order to rule out a mycological cause. To rule out contact dermatitis, doctors can carry out the patch test. Doctors don’t usually require a biopsy for this type of pathology.
What are the treatment options?
There’s no specific treatment for juvenile plantar dermatitis. In fact, it’s a condition that, even if the problem is resolved, tends to recur at some point.
Reducing footwear friction
You should always use the correct shoe size and use 100% breathable cotton socks, since synthetics don’t help to solve the problem at all.
Whenever possible, try not to keep sports shoes on too long, especially after perspiring. Where perspiration is excessive, we recommend that you change socks regularly, to avoid the formation of a humid environment.
Moisturize the skin
In a similar way to all conditions with an atopic origin, we recommend, as a first line of treatment, that you also habitually and constantly moisturize the skin.
After each bath or shower, or before going to bed, the skin should be correctly moisturized. In fact, you can use creams with petroleum jelly or urea for the plantar and heel areas.
Prescription creams
When there are cracks and fissures, the use of tacrolimus or corticosteroid based ointments can be very useful. Topical corticosteroids are compounds that you shouldn’t use for more than 10 days, nor should you use them regularly. This is due to the skin getting used to it too easily (thus reducing its effectiveness), and also its adverse effects with prolonged use.
However, it’s always advisable to consult a skin specialist, who’ll be able to resolve any questions you may have, and provide a diagnosis and treatment appropriate to each case.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Lachapelle JM, Tennstedt D. Juvenile plantar dermatosis: a report of 80 cases. Am J Ind Med. 1985;8(4-5):291-5. doi: 10.1002/ajim.4700080407. PMID: 4073027.
- Neering H, van Dijk E. Juvenile plantar dermatosis. Acta Derm Venereol. 1978;58(6):531-4. PMID: 83078.
- Ashton RE, Jones RR, Griffiths A. Juvenile plantar dermatosis. A clinicopathologic study. Arch Dermatol. 1985 Feb;121(2):225-8. PMID: 3977336.
- Pirkl S, Tennstedt D, Eggers S, Lachapelle JM. Juvenile plantar dermatosis: wann sind Epikutantestungen indiziert? [Juvenile plantar dermatosis: when are epicutaneous tests indicated?]. Hautarzt. 1990 Jan;41(1):22-6. German. PMID: 2138140.
- Jones SK, English JS, Forsyth A, Mackie RM. Juvenile plantar dermatosis–an 8-year follow-up of 102 patients. Clin Exp Dermatol. 1987 Jan;12(1):5-7. doi: 10.1111/j.1365-2230.1987.tb01843.x. PMID: 3652505.
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








