Scabies in Children: Symptoms, Causes and Treatment

Written and verified by the dermatologist Maria del Carmen Hernandez
Scabies in children is a common and contagious skin disease. Although it can affect children of any socioeconomic level, people living in poverty or in overcrowded conditions are at a much higher risk of contracting it.
What’s more, the risk of contracting scabies is greater in young children, the elderly, and people with weakened immune systems.
Causes of scabies in children
Scabies develops from a mite, Sarcoptes Scabiei, which spreads via direct skin-to-skin contact. The mite only remains alive outside of skin contact for about 24 to 36 hours. Therefore, transmission through fomites, clothing, sheets, and blankets is limited.
The infected child develops a hypersensitivity reaction to the mite, its eggs, and faeces. This reaction can occur 3 weeks after exposure to the infectious agent.

In 2009, the World Health Organization (WHO) declared it a neglected skin disease. At the same time, only 10 minutes of skin-to-skin contact is necessary for mites to spread.
You may be interested in: 7 Effective Home Remedies for Dust Mites
Symptoms of scabies in children
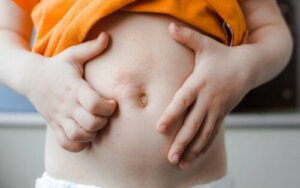
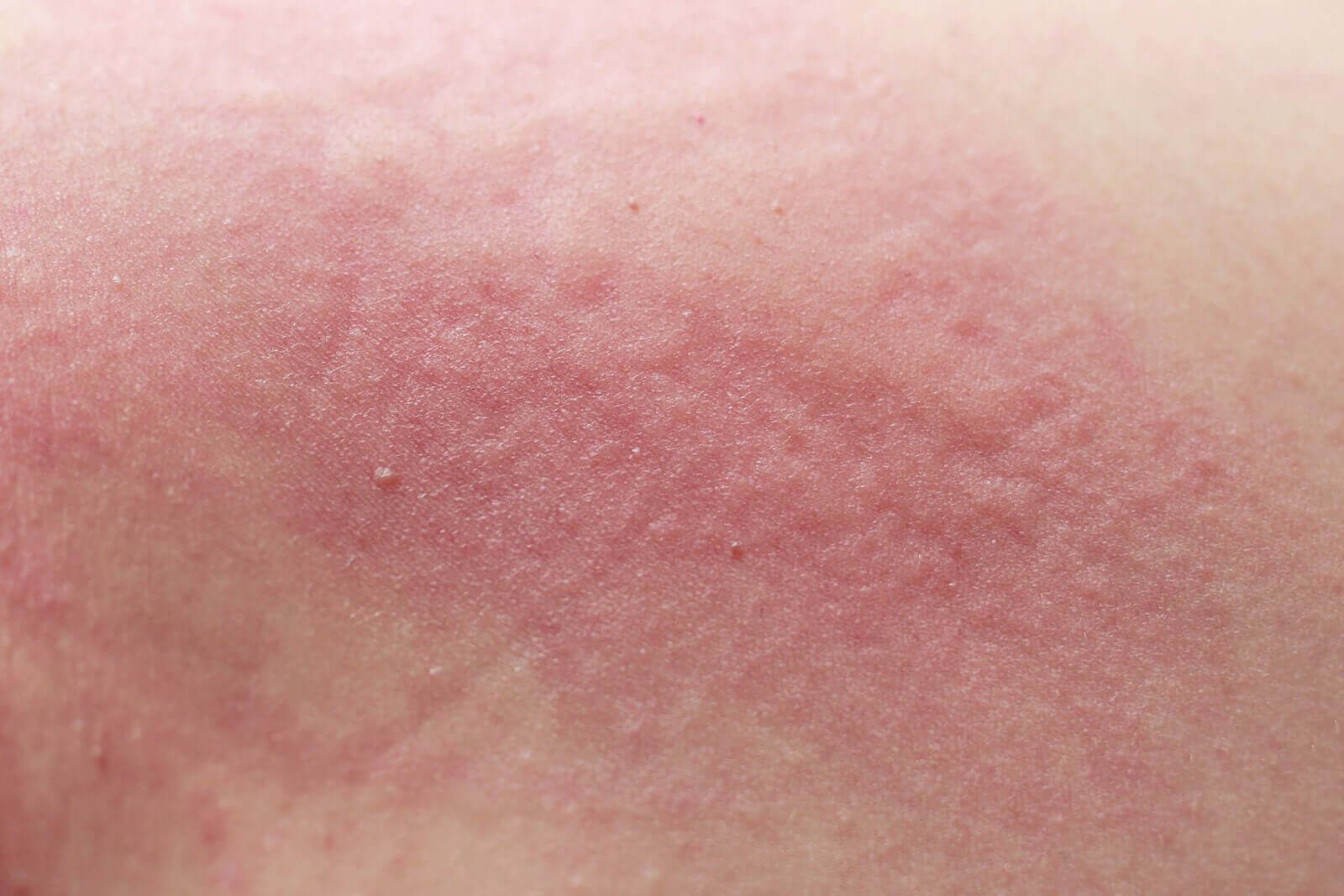
The presentation of the symptoms of this parasitic infection includes erythematous papules and a generalized itching that usually increases at night.
According to a publication by the Asturias Pediatric Society, in children, the lesions are located on the palms of the hands, the soles of the feet, and the cephalic pole.
However, in adults the locations vary and prevail between the fingers, in the flexion of the wrist, elbows, or armpits, or in the genitals and breasts.
All these symptoms take about 3 weeks to appear after contact with the mite. However, in the case of reinfections, clinical manifestations may arise within hours.
How is the diagnosis made?
Observation of the skin lesions by a specialist at the time of consultation is the basis of the diagnosis of scabies in children. At the same time, the doctor will carry out a thorough interrogation to rule out the patient’s history.
However, to confirm the diagnosis, a specialist can observe the mites, eggs, or feces from a skin scraping under the microscope.
If the diagnosis is uncertain, they can also take a biopsy of the lesion to obtain more certainty. But this type of procedure isn’t common.
Differential diagnostics
It’s easy to confuse scabies with other itchy rashes:
- Eczema
- Impetigo
- Tinea corporis
- Prurigo nodularis
- Dermatitis
- Pruriginous pathologies
- Psoriasis
However, in scabies it’s possible to find the routes that the mite takes to advance; these are called tunnels. These are white serpinginous lines which indicate the excavation of the parasites.
Read also: Contagious Diseases that Spread in Daycare Centers
Therapeutic options for scabies in children
It’s crucial to simultaneously treat symptomatic or asymptomatic household members to avoid transmission or reinfection. The main reason for treating those without symptoms is that it can take weeks for symptoms to appear.
Permethrin
Permethrin topical lotions or creams at 5% are the first-line treatment. You should apply them to the skin from the neck to the toes, usually at night; the next day you rinse it off.
For babies with scabies, you should apply it to the face as well. One week after the initial application, you’ll need to repeat the procedure in order to kill any larvae born during this period. Also, you should warn patients and relatives about the likelihood that the itching will persist for a long time.
Ivermectin
Oral ivermectin is another option available in order to manage scabies treatment in children ages 10 and up. Again, it requires an initial treatment followed by a second dose after one week.
This therapeutic option may be preferable because of the following advantages:
- For its convenience, as it increases compliance rates
- Safety
- Ease of administration, as it reduces the probability of misuse or improper application
- Few adverse effects
- Other variants
What’s more, you’ll need to disinfect sheets, quilts, towels, and clothing. Other therapeutic options are topical lindane, 5% precipitated sulphur, malathion, and topical ivermectin.
When it comes to pregnant women and young children, you should use precipitated sulphur at 5% in petroleum jelly. Although its odor and messy application make treatment undesirable, it’s the safest option.
Ultimately, even with proper treatment, symptoms and signs can persist for several weeks and then resolve completely.
The good prognosis of the disease is related to the treatment of the patient and his or her close contacts. Therefore, if treatment isn’t carried out properly, scabies can spread to the rest of the close contacts.
Scabies in children is a common and contagious skin disease. Although it can affect children of any socioeconomic level, people living in poverty or in overcrowded conditions are at a much higher risk of contracting it.
What’s more, the risk of contracting scabies is greater in young children, the elderly, and people with weakened immune systems.
Causes of scabies in children
Scabies develops from a mite, Sarcoptes Scabiei, which spreads via direct skin-to-skin contact. The mite only remains alive outside of skin contact for about 24 to 36 hours. Therefore, transmission through fomites, clothing, sheets, and blankets is limited.
The infected child develops a hypersensitivity reaction to the mite, its eggs, and faeces. This reaction can occur 3 weeks after exposure to the infectious agent.

In 2009, the World Health Organization (WHO) declared it a neglected skin disease. At the same time, only 10 minutes of skin-to-skin contact is necessary for mites to spread.
You may be interested in: 7 Effective Home Remedies for Dust Mites
Symptoms of scabies in children
The presentation of the symptoms of this parasitic infection includes erythematous papules and a generalized itching that usually increases at night.
According to a publication by the Asturias Pediatric Society, in children, the lesions are located on the palms of the hands, the soles of the feet, and the cephalic pole.
However, in adults the locations vary and prevail between the fingers, in the flexion of the wrist, elbows, or armpits, or in the genitals and breasts.
All these symptoms take about 3 weeks to appear after contact with the mite. However, in the case of reinfections, clinical manifestations may arise within hours.
How is the diagnosis made?
Observation of the skin lesions by a specialist at the time of consultation is the basis of the diagnosis of scabies in children. At the same time, the doctor will carry out a thorough interrogation to rule out the patient’s history.
However, to confirm the diagnosis, a specialist can observe the mites, eggs, or feces from a skin scraping under the microscope.
If the diagnosis is uncertain, they can also take a biopsy of the lesion to obtain more certainty. But this type of procedure isn’t common.
Differential diagnostics
It’s easy to confuse scabies with other itchy rashes:
- Eczema
- Impetigo
- Tinea corporis
- Prurigo nodularis
- Dermatitis
- Pruriginous pathologies
- Psoriasis
However, in scabies it’s possible to find the routes that the mite takes to advance; these are called tunnels. These are white serpinginous lines which indicate the excavation of the parasites.
Read also: Contagious Diseases that Spread in Daycare Centers
Therapeutic options for scabies in children
It’s crucial to simultaneously treat symptomatic or asymptomatic household members to avoid transmission or reinfection. The main reason for treating those without symptoms is that it can take weeks for symptoms to appear.
Permethrin
Permethrin topical lotions or creams at 5% are the first-line treatment. You should apply them to the skin from the neck to the toes, usually at night; the next day you rinse it off.
For babies with scabies, you should apply it to the face as well. One week after the initial application, you’ll need to repeat the procedure in order to kill any larvae born during this period. Also, you should warn patients and relatives about the likelihood that the itching will persist for a long time.

Ivermectin
Oral ivermectin is another option available in order to manage scabies treatment in children ages 10 and up. Again, it requires an initial treatment followed by a second dose after one week.
This therapeutic option may be preferable because of the following advantages:
- For its convenience, as it increases compliance rates
- Safety
- Ease of administration, as it reduces the probability of misuse or improper application
- Few adverse effects
- Other variants
What’s more, you’ll need to disinfect sheets, quilts, towels, and clothing. Other therapeutic options are topical lindane, 5% precipitated sulphur, malathion, and topical ivermectin.
When it comes to pregnant women and young children, you should use precipitated sulphur at 5% in petroleum jelly. Although its odor and messy application make treatment undesirable, it’s the safest option.
Ultimately, even with proper treatment, symptoms and signs can persist for several weeks and then resolve completely.
The good prognosis of the disease is related to the treatment of the patient and his or her close contacts. Therefore, if treatment isn’t carried out properly, scabies can spread to the rest of the close contacts.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Hengge UR, Currie BJ, Jäger G, Lupi O, Schwartz RA. Scabies: a ubiquitous neglected skin disease. Lancet Infect Dis. 2006 Dec;6(12):769-79. doi: 10.1016/S1473-3099(06)70654-5. PMID: 17123897.
- Anderson KL, Strowd LC. Epidemiology, Diagnosis, and Treatment of Scabies in a Dermatology Office. J Am Board Fam Med. 2017 Jan 2;30(1):78-84. doi: 10.3122/jabfm.2017.01.160190. PMID: 28062820.
- Mounsey KE, McCarthy JS. Treatment and control of scabies. Curr Opin Infect Dis. 2013 Apr;26(2):133-9. doi: 10.1097/QCO.0b013e32835e1d57. PMID: 23438966.
- Dressler C, Rosumeck S, Sunderkötter C, Werner RN, Nast A. The Treatment of Scabies. Dtsch Arztebl Int. 2016 Nov 14;113(45):757-762. doi: 10.3238/arztebl.2016.0757. PMID: 27974144; PMCID: PMC5165060.
- Chhaiya SB, Patel VJ, Dave JN, Mehta DS, Shah HA. Comparative efficacy and safety of topical permethrin, topical ivermectin, and oral ivermectin in patients of uncomplicated scabies. Indian J Dermatol Venereol Leprol. 2012 Sep-Oct;78(5):605-10. doi: 10.4103/0378-6323.100571. PMID: 22960817.
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








