Sturge-Weber Syndrome in Children
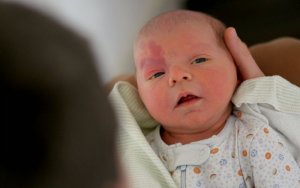
Sturge-Weber syndrome (SSW) is a rare congenital disease. Above all, its most distinctive feature is a birthmark on the face, as well as neurological symptoms. For these reasons, it’s considered a neurocutaneous syndrome.
SSW was first described in 1860, although its most distinctive characteristics were studied later on. Depending on its symptoms, it’s considered that there are three types of SSW:
- SSW Type 1: facial angioma and leptomeninges.
- Type 2: facial angioma alone.
- Type 3: only leptomeninges.
According to several studies, it starts at the beginning of pregnancy, between the first 6 to 9 weeks. Although its cause is unknown, there’s a genetic mutation that triggers it and affects a protein related to certain growth factors, vasoactive peptides, and some neurotransmitters.
Clinical symptoms of Sturge-Weber Syndrome
The symptoms of Sturge-Weber syndrome have three categories:
- Facial angioma.
- Ocular manifestations, like glaucoma.
- Neurological damage.
Facial angioma
The most characteristic of its symptoms, Sturge-Weber’s facial angioma is in the shape of a port-wine birthmark. It’s usually present either on the forehead or the upper eyelid. Although it’s not as common, it can also be found on other parts of the face, or even the torso and limbs.
Often, this facial angioma can be related to soft-tissue hypertrophy, and sometimes it may reach the bones. This can also affect the eyes, ear, speech patterns, among other things.
Ocular manifestations
Ocular manifestation and other ophthalmic trauma are another important part of the diagnosis and prognosis of this disease. One of the most common ocular manifestations is glaucoma. Glaucoma increases eye pressure and can lead to blindness.
Neurological damage
There have been a few cases where Sturge-Weber’s signature birthmark doesn’t show. These types of cases are worse because facial angioma can instead be present in the nervous system, in the leptomeninges to be exact.
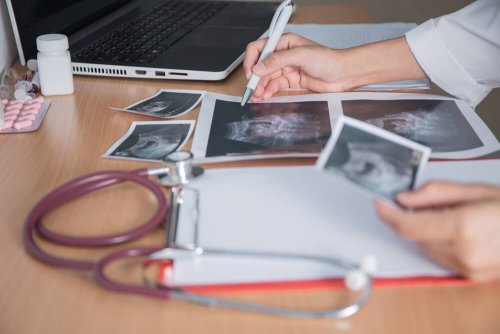
Neurological or brain damage in this syndrome can affect the leptomeninges, as well as lead to seizures and mental retardation. Most certainly, these signs are shown as calcifications of the skull and can be detected through prenatal ultrasounds.
Between 75% and 90% of patients with Sturge-Weber syndrome can suffer seizures – the most common neurological manifestation of the disease. These episodes can be long-lasting, repeat frequently, and are also hard to control with regular treatments.
Because of these seizures, among 50% to 70% of patients can develop mental retardation. These neurological manifestations can also lead to hemiparesis (weakness of the entire left or right side of the body) and hemianopsia (loss of half the visual field in one or both eyes).

Medical treatments for Sturge-Weber syndrome
Medical treatment for Sturge-Weber syndrome has to be multidisciplinary, just as its diagnosis. Likewise, this syndrome requires physicians of different fields, like neurology, neurosurgery, ophthalmology, dermatology, etc.
As for the neurological manifestations, the main concern for treatment is controlling the seizures and epileptic episodes. These can be pharmacological or surgical therapies or the combination of both. This is mostly the case because the pharmacological therapies can only solve almost 50% of epileptic episodes.
Treatment for glaucoma is difficult and it often requires surgery. However, facial angioma is usually an aesthetic issue. A therapy that’s proven to be useful and used frequently is a laser, besides using makeup to hide the mark.

In short, early diagnosis of this syndrome is essential, because it can compromise your child’s health and quality of life. Symptoms won’t always be the same or be present at once but, if you have a slight suspicion, pay attention to what you see and seek medical advice.
Sturge-Weber syndrome (SSW) is a rare congenital disease. Above all, its most distinctive feature is a birthmark on the face, as well as neurological symptoms. For these reasons, it’s considered a neurocutaneous syndrome.
SSW was first described in 1860, although its most distinctive characteristics were studied later on. Depending on its symptoms, it’s considered that there are three types of SSW:
- SSW Type 1: facial angioma and leptomeninges.
- Type 2: facial angioma alone.
- Type 3: only leptomeninges.
According to several studies, it starts at the beginning of pregnancy, between the first 6 to 9 weeks. Although its cause is unknown, there’s a genetic mutation that triggers it and affects a protein related to certain growth factors, vasoactive peptides, and some neurotransmitters.
Clinical symptoms of Sturge-Weber Syndrome
The symptoms of Sturge-Weber syndrome have three categories:
- Facial angioma.
- Ocular manifestations, like glaucoma.
- Neurological damage.

Facial angioma
The most characteristic of its symptoms, Sturge-Weber’s facial angioma is in the shape of a port-wine birthmark. It’s usually present either on the forehead or the upper eyelid. Although it’s not as common, it can also be found on other parts of the face, or even the torso and limbs.
Often, this facial angioma can be related to soft-tissue hypertrophy, and sometimes it may reach the bones. This can also affect the eyes, ear, speech patterns, among other things.
Ocular manifestations
Ocular manifestation and other ophthalmic trauma are another important part of the diagnosis and prognosis of this disease. One of the most common ocular manifestations is glaucoma. Glaucoma increases eye pressure and can lead to blindness.
Neurological damage
There have been a few cases where Sturge-Weber’s signature birthmark doesn’t show. These types of cases are worse because facial angioma can instead be present in the nervous system, in the leptomeninges to be exact.
Neurological or brain damage in this syndrome can affect the leptomeninges, as well as lead to seizures and mental retardation. Most certainly, these signs are shown as calcifications of the skull and can be detected through prenatal ultrasounds.
Between 75% and 90% of patients with Sturge-Weber syndrome can suffer seizures – the most common neurological manifestation of the disease. These episodes can be long-lasting, repeat frequently, and are also hard to control with regular treatments.
Because of these seizures, among 50% to 70% of patients can develop mental retardation. These neurological manifestations can also lead to hemiparesis (weakness of the entire left or right side of the body) and hemianopsia (loss of half the visual field in one or both eyes).

Medical treatments for Sturge-Weber syndrome
Medical treatment for Sturge-Weber syndrome has to be multidisciplinary, just as its diagnosis. Likewise, this syndrome requires physicians of different fields, like neurology, neurosurgery, ophthalmology, dermatology, etc.
As for the neurological manifestations, the main concern for treatment is controlling the seizures and epileptic episodes. These can be pharmacological or surgical therapies or the combination of both. This is mostly the case because the pharmacological therapies can only solve almost 50% of epileptic episodes.
Treatment for glaucoma is difficult and it often requires surgery. However, facial angioma is usually an aesthetic issue. A therapy that’s proven to be useful and used frequently is a laser, besides using makeup to hide the mark.

In short, early diagnosis of this syndrome is essential, because it can compromise your child’s health and quality of life. Symptoms won’t always be the same or be present at once but, if you have a slight suspicion, pay attention to what you see and seek medical advice.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Fernández Concepción, O., Gómez García, A., & Sardiñaz Hernández, N. (1999). Síndrome de Sturge weber. Revisión. Revista Cubana de Pediatria, 71(3), 153-159.
- Mallea, J. M., Heras, I. G., Aguirre, P. B., Serrano, F. M., Tena, J. G., Rubio, J. M., & Delgado, F. M. (1997). Sindrome de Sturge-Weber: Experiencia en 14 casos. An Esp Pediatr, 46, 138-142.
- Rodofile, C., Grees, S. A., Valle, L. E., & Martino, G. (2011). Síndrome de Sturge-Weber: Presentación de un caso con manifestaciones dermatológicas mínimas. Archivos argentinos de pediatría, 109(2), 42-45.
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








